Adapalene (Differin) for Teens: The Complete Starter Guide
Medically reviewed by Dr. Rachel Torres, MD, Pediatric Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated April 29, 2026
Adapalene (Differin) for Teens: The Complete Starter Guide

In 2016, the FDA did something that quietly changed teen skincare: they approved adapalene 0.1% gel for over-the-counter sale. Before that, retinoids required a prescription and a dermatologist visit. Now you can pick one up at CVS for about $13.
Adapalene (sold as Differin, plus generics) is a third-generation retinoid, and retinoids are considered the gold standard for treating acne by basically every dermatological organization on the planet. The American Academy of Dermatology recommends them as a foundation of acne therapy [1]. They work differently from benzoyl peroxide or salicylic acid, and in many cases they work better.
But here's the problem. Adapalene has a rocky start. Your skin will probably get worse before it gets better. If nobody tells you that ahead of time, you'll quit during week three, convinced it's making everything worse. Most teens do exactly this. I want to make sure you don't.
What Adapalene Actually Does
Adapalene belongs to the retinoid family, which means it's derived from vitamin A. What makes retinoids special is that they change how your skin cells behave at a fundamental level.
Your acne starts when dead skin cells inside a hair follicle stick together instead of shedding normally. This creates a plug. Oil gets trapped behind the plug. Bacteria grow in the trapped oil. Inflammation follows. That's the simplified version, but it captures the sequence.
Adapalene interrupts this process right at the beginning. It binds to specific retinoic acid receptors in your skin cells (RAR-beta and RAR-gamma, if you're curious) and changes gene expression in a way that normalizes cell turnover [2]. Your skin cells stop clumping together. Plugs don't form. Without plugs, you don't get the cascade that leads to pimples.
It also has anti-inflammatory properties independent of its effects on cell turnover. A 2008 study in the British Journal of Dermatology demonstrated that adapalene inhibits lipoxygenase activity and the oxidative metabolism of arachidonic acid, which reduces inflammation through a pathway completely separate from how it prevents clogged pores [3].
This dual action, preventing new acne from forming while calming existing inflammation, is why retinoids are the backbone of acne treatment, not just one option among many.
The Purging Period: Weeks 2-6
I'm putting this near the top because it's the single most important thing to understand before you start.
Somewhere around week two, your skin is going to break out. Maybe worse than before you started. This is called purging, and it happens because adapalene is speeding up your skin's cell turnover. All those microcomedones (tiny clogs you couldn't see yet) that were going to become pimples over the next few weeks or months get pushed to the surface all at once.
Purging is not the same as a bad reaction. Here's how to tell the difference:
Purging looks like: breakouts in places where you normally get acne, appearing and resolving faster than your usual pimples, mostly whiteheads and small inflamed bumps.
A bad reaction looks like: breakouts in places you've never had acne before, tiny bumps all over (possibly an allergic response), intense redness or burning that doesn't calm down, rash-like patterns.
Purging typically peaks between weeks 2 and 4, then starts improving by weeks 5-6. Some people purge mildly. Others have a rough month. A study published in the Journal of the American Academy of Dermatology tracking adapalene use over 12 weeks showed that early worsening was common but that most patients showed significant improvement by week 8, with continued improvement through week 12 [4].

This purging period is why so many teens give up on adapalene. They try it for three weeks, their skin explodes, and they throw it away. Completely understandable reaction. But if they'd pushed through to week 8, many of them would have seen real results.
How to Start: The Slow Introduction Method
Jumping into nightly adapalene use is a mistake almost everyone makes. Your skin has never experienced a retinoid before, and it needs time to adjust. Here's the approach most dermatologists recommend:
Week 1-2: Apply adapalene every other night. Just two to three times the first week.
Week 3-4: Move to every other night consistently if your skin is handling it.
Week 5-6: Try every night. If you're getting significant dryness or irritation, stay at every other night for another couple of weeks.
Week 7+: Nightly use for most people. Some people with sensitive skin do better with every other night permanently, and that's fine.
Always apply at night. Adapalene breaks down in sunlight (more on that below), and your skin does most of its repair work overnight anyway.
The Pea-Sized Amount Rule
This is not a figure of speech. You literally need a pea-sized amount for your entire face. I'm talking about a small dot, roughly the size of an actual green pea, on your fingertip.
Squeeze it out. Look at it. If you're thinking "that's not enough," you have the right amount.
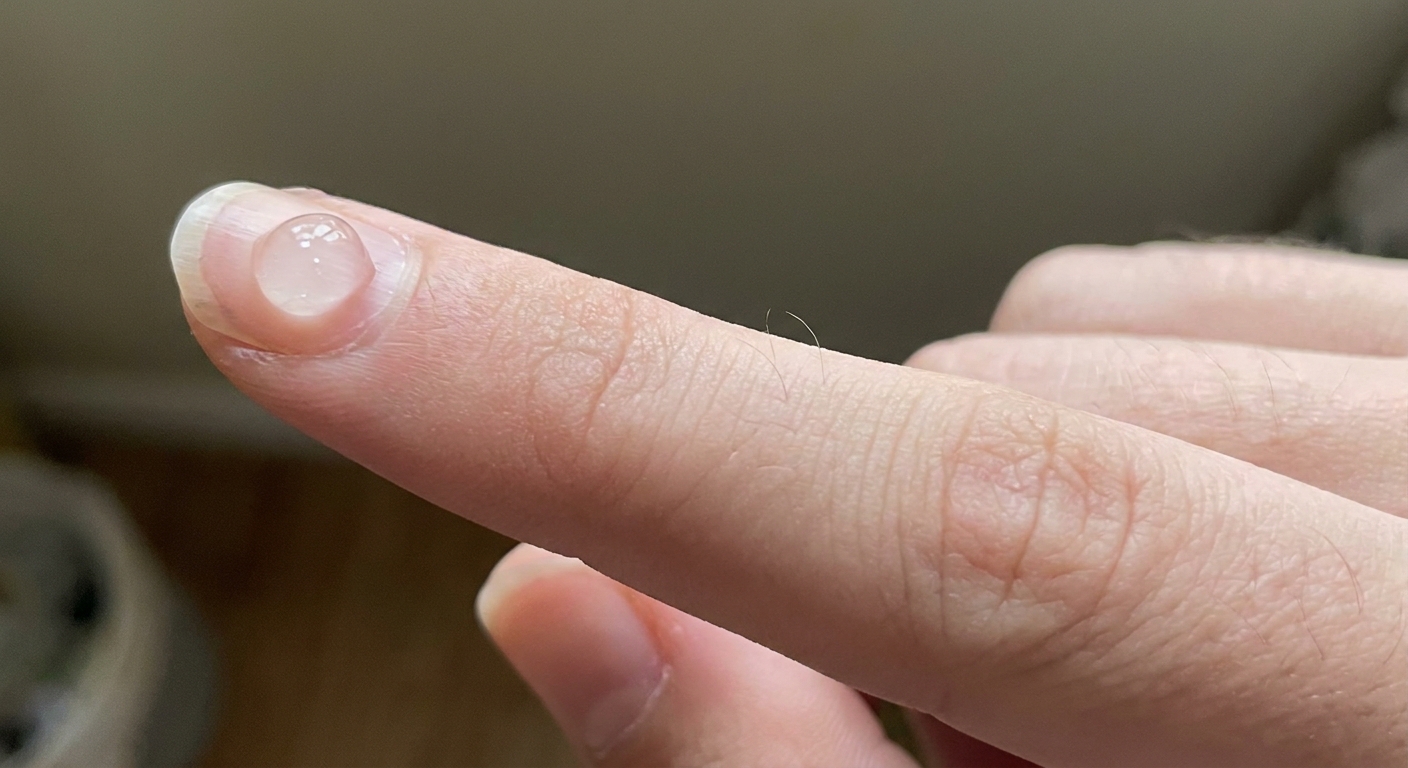
More adapalene does not mean faster results. It means more irritation, more peeling, more redness, and probably the same timeline for improvement. A thin, even layer is what you're going for. Dot it on your forehead, each cheek, nose, and chin, then blend outward. It takes about 30 seconds.
Using too much is probably the second most common reason teens have a bad experience with adapalene, right after quitting during the purge.
The Buffering Technique
If adapalene irritates your skin even with the slow introduction, try buffering. This means applying your moisturizer first, waiting 5-10 minutes for it to absorb, and then applying adapalene on top.
The moisturizer creates a thin barrier that slightly slows the absorption of adapalene into your skin. You still get the benefits, but the irritation is reduced. A study in Cutis found that applying adapalene over moisturizer did not significantly reduce its efficacy while improving tolerability in patients with sensitive skin [5].
This isn't cheating or diluting the product. Dermatologists recommend it regularly, especially for their younger patients who haven't used actives before. Once your skin acclimates over a few weeks, you can try switching to applying adapalene first and moisturizer second (the standard order), and see if your skin handles it.
Sun Sensitivity: Not Optional to Address
Adapalene makes your skin more sensitive to UV radiation. This is a real effect, not an exaggerated warning. The increased cell turnover means your newer, thinner skin cells are closer to the surface and more vulnerable to sun damage.
You need to wear sunscreen every morning while using adapalene. SPF 30 minimum, broad-spectrum. Every single morning. Even on cloudy days, even in winter, even if you're just walking to school.
I know this sounds annoying. It is annoying. But getting a sunburn on retinoid-thinned skin is genuinely painful, and sun exposure can worsen the exact hyperpigmentation you might be using adapalene to treat. Pick a sunscreen you'll actually use. Something lightweight that doesn't leave a white cast and won't break you out. CeraVe, La Roche-Posay, and EltaMD all make options specifically formulated for acne-prone skin.
If you skip the sunscreen, you're undermining half the work the adapalene is doing.
The 12-Week Commitment
I want to be blunt about the timeline because I think unrealistic expectations ruin more acne treatments than the treatments themselves.
Week 1-2: You might notice some dryness and flaking. Your skin is adjusting.
Week 2-4: Purging begins. New breakouts appear. Frustration peaks.
Week 4-6: Purging starts to slow down for most people. Existing breakouts begin healing.
Week 6-8: Things start looking noticeably better. Fewer new breakouts. Skin texture improves.
Week 8-12: Significant improvement. Skin is clearer, smoother, and more even-toned.
Week 12+: Full effects visible. Maintenance mode.
A 2004 meta-analysis of adapalene trials published in the Journal of the European Academy of Dermatology and Venereology found that adapalene 0.1% gel produced a median 63% reduction in total acne lesions at 12 weeks [6]. That's strong. But none of that shows up at week three.
Commit to 12 weeks minimum. Put a reminder on your phone. Mark it on a calendar. Whatever it takes to get past the rough patch.
Using Adapalene for Body Acne
Acne on your back, chest, or shoulders follows the same basic biology as facial acne, and adapalene works on those areas too. But you need to adjust your approach.
The skin on your body is thicker than your face, so it can typically handle adapalene with less irritation. You can usually start with nightly application on body areas. Apply after showering when your skin is clean and dry.
The pea-sized rule doesn't apply here because you're covering a much larger surface area. Use enough to create a thin, even layer over the affected area. For a full back, you might need a nickel-to-quarter-sized amount.
One practical issue: reaching your own back is difficult. If you have someone who can help you apply it, great. If not, there are applicator tools designed for this (lotion applicators with long handles) that work reasonably well. You can also look into adapalene-containing body washes and sprays that are easier to apply, though contact time with a wash-off product is shorter and may be less effective than a leave-on gel.
What to Pair with Adapalene
Adapalene works well as part of a routine, not necessarily alone. Here's what combines well and what to avoid:
Good combinations:
- A gentle, non-foaming cleanser (CeraVe Hydrating, Vanicream Gentle, La Roche-Posay Toleriane)
- A basic moisturizer (CeraVe Moisturizing Cream, Vanicream Daily Facial Moisturizer)
- Benzoyl peroxide in the morning (adapalene at night). This combination is so effective that there's literally an FDA-approved product (Epiduo) that combines them. A randomized controlled trial showed the combination outperformed either ingredient alone [7]
- Niacinamide, which helps with irritation and oil control
Avoid combining with:
- Other retinoids (tretinoin, tazarotene). You don't need two retinoids.
- AHA/BHA exfoliants (glycolic acid, lactic acid, salicylic acid at high concentrations) in the same routine. Using these on different nights or different times of day is fine once your skin has adjusted to adapalene, but layering them together, especially early on, is a recipe for irritation.
- Physical scrubs. Your skin is already experiencing accelerated turnover. Scrubbing on top of that strips your barrier.
Common Mistakes to Avoid
Applying to wet skin. Always apply adapalene to completely dry skin. Wet skin absorbs it faster and deeper, which sounds like a good thing but actually just increases irritation. After washing your face, wait a full 5-10 minutes before applying.
Using it around the eyes, corners of the nose, and lips. These areas have thinner skin and will get irritated fast. Keep the adapalene away from them. Applying a thin layer of Vaseline or Aquaphor around your eyes and lips before using adapalene can act as a protective barrier if you tend to accidentally spread product to those areas.
Stopping during purging. I've said it before, but it bears repeating. The purge is the treatment working. Stopping means you went through the worst part for nothing.
Using multiple new products at once. If you start adapalene, a new cleanser, a new moisturizer, and a new sunscreen all in the same week, you'll have no idea what's causing any irritation you experience. Introduce adapalene into an otherwise stable routine.
Key Takeaways
- Adapalene is now OTC and costs about $13 for a generic tube. You don't need a dermatologist visit to start, though consulting one is still smart.
- Purging is normal and expected. Weeks 2-6 will likely bring more breakouts. This is the treatment accelerating what was already forming under your skin.
- Start slow. Every other night for the first few weeks, pea-sized amount, and consider buffering with moisturizer first.
- Wear sunscreen every day. Non-negotiable while using any retinoid. SPF 30+, broad-spectrum.
- Commit to 12 weeks. The data is clear that adapalene works, but it takes time. Most of the benefit shows up between weeks 8 and 12.
The Bottom Line
Adapalene going OTC was one of the biggest developments in teen acne treatment in decades. For about the price of a fast food meal, you can access a medication class that dermatologists consider the gold standard for acne. But it demands patience. The purging phase is real, the dryness is real, and the temptation to quit early is real.
If you stick with it through 12 weeks while being smart about how you introduce it (slow start, buffer if needed, moisturize well, sunscreen always), you're giving your skin access to a genuinely powerful treatment that works on a level most drugstore products simply cannot match. The teens who get the best results aren't the ones with the most products. They're the ones who picked the right product and refused to give up on it.
Sources
- Zaenglein AL, et al. "Guidelines of care for the management of acne vulgaris." Journal of the American Academy of Dermatology. 2016;74(5):945-973. doi:10.1016/j.jaad.2015.12.037
- Shroot B, Michel S. "Pharmacology and chemistry of adapalene." Journal of the American Academy of Dermatology. 1997;36(6 Pt 2):S96-S103. doi:10.1016/s0190-9622(97)70050-x
- Tenaud I, et al. "In vitro modulation of TLR-2, CD1d and IL-10 by adapalene on normal human skin and acne inflammatory lesions." British Journal of Dermatology. 2008;159(Suppl 1):12-17.
- Thiboutot DM, et al. "Adapalene gel 0.3% for the treatment of acne vulgaris: a multicenter, randomized, double-blind, controlled, phase III trial." Journal of the American Academy of Dermatology. 2007;57(5):791-799. doi:10.1016/j.jaad.2007.06.006
- Dréno B, et al. "The influence of exposome on acne." Journal of the European Academy of Dermatology and Venereology. 2018;32(5):812-819. doi:10.1111/jdv.14820
- Waugh J, Noble S, Scott LJ. "Adapalene: a review of its use in the treatment of acne vulgaris." Drugs. 2004;64(13):1465-1478. doi:10.2165/00003495-200464130-00005
- Gold LS, et al. "A randomized, controlled trial of adapalene-benzoyl peroxide gel vs. vehicle gel for the treatment of acne vulgaris." Journal of the American Academy of Dermatology. 2009;60(6):934-943. doi:10.1016/j.jaad.2008.12.038
- Czernielewski J, et al. "Adapalene biochemistry and the evolution of a new topical retinoid for treatment of acne." Journal of the European Academy of Dermatology and Venereology. 2001;15(Suppl 3):5-12.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
Read This Next

Niacinamide for Acne: The Gentle Ingredient That Does Everything

Azelaic Acid for Acne: The Underrated Treatment Teens Should Know About

Natural vs. Medicated Acne Treatments: What the Evidence Actually Shows
Tea tree oil has real data behind it, but most 'natural' acne products are marketing hype. Here's what the research says about natural vs. medicated treatments — and why the best approach might combine both.
Read More →
Drugstore vs. Prescription Acne Products: When to Upgrade
Most teens don't need a prescription to clear their skin. Here's how to tell if drugstore products are enough -- and when it's time to see a dermatologist.
Read More →
Acne Patches and Spot Treatments Ranked: Which Ones Actually Work
We tested the most popular acne patches and spot treatments to figure out which ones are worth your money — and which are just cute packaging with a markup.
Read More →