Salicylic Acid for Acne: Clinical Evidence and Realistic Outcomes
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Team — Updated March 17, 2026
Key takeaways
- Salicylic acid works primarily on blackheads and whiteheads with minimal impact on inflammatory acne (papules, pustules, cysts), limiting its usefulness for most teen acne.
- Studies show only 20-35% improvement in total lesion count after 12 weeks, significantly lower than prescription alternatives like retinoids.
- Skin barrier disruption occurs in 25-40% of users causing increased sensitivity, redness, and potential worsening of acne through barrier impairment.

Salicylic acid appears in countless over-the-counter acne products marketed to teenagers, often positioned as a "gentler alternative" to harsher treatments. As a dermatologist reviewing the clinical evidence, I find this characterization misleading. While salicylic acid has specific applications where it performs adequately, the gap between marketing claims and published efficacy data is substantial.
Mechanism of Action
Salicylic acid is a beta-hydroxy acid (BHA) that works through two primary mechanisms:
Keratolytic effect: Dissolves the intercellular cement holding dead skin cells together, promoting exfoliation. This occurs at concentrations of 0.5-2% in most over-the-counter formulations.
Lipophilic penetration: Unlike water-soluble alpha-hydroxy acids, salicylic acid can penetrate oil-filled pores due to its fat-soluble properties.
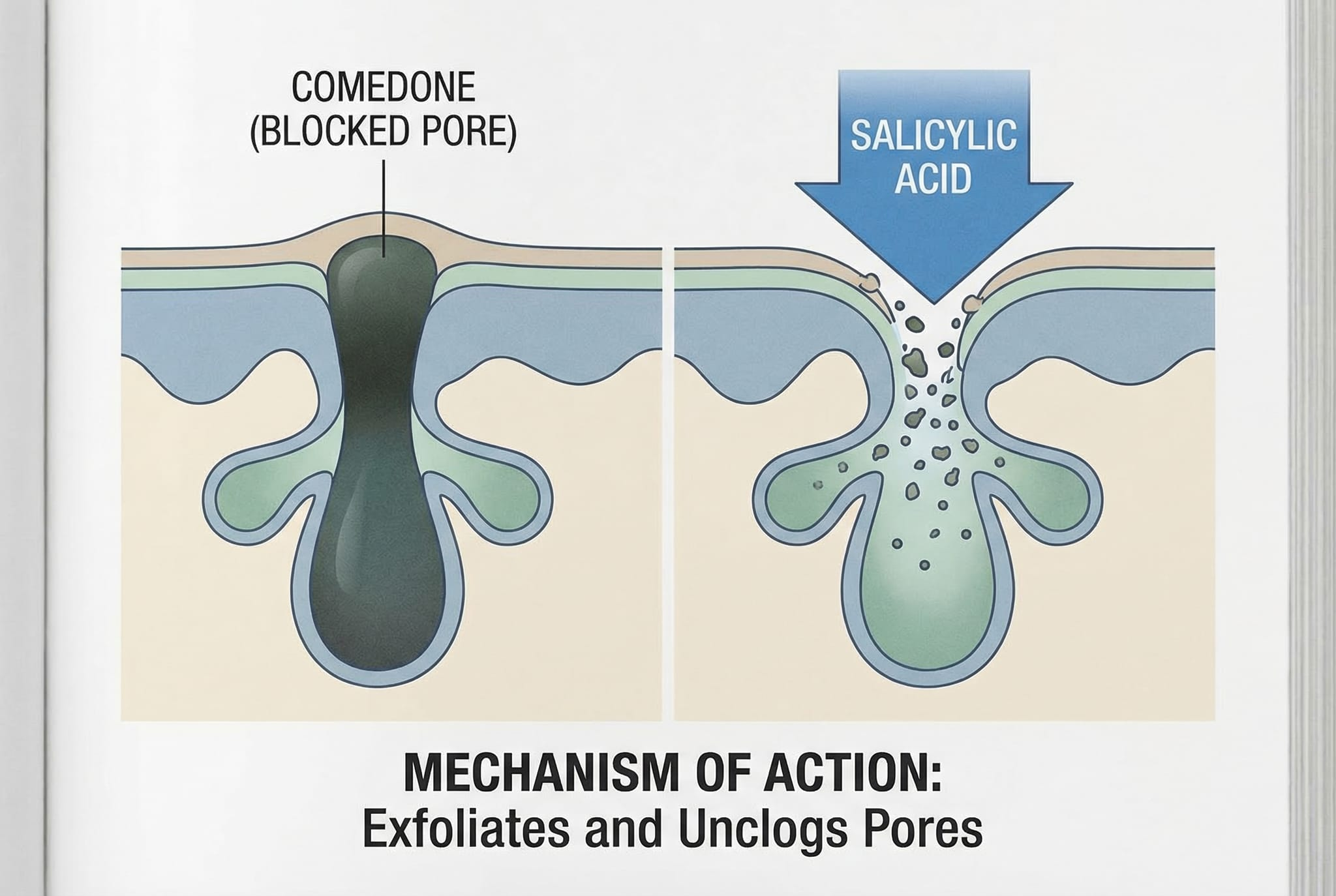
What this means clinically: Salicylic acid is theoretically effective at unclogging pores containing dead skin cells and oil. However, acne pathophysiology involves multiple factors beyond simple pore clogging—including inflammation, bacterial proliferation, and hormonal influences—none of which salicylic acid addresses effectively.
Clinical Efficacy Data
The published literature on salicylic acid for acne reveals significantly more modest results than product labeling suggests. A 2015 comprehensive review in Clinical, Cosmetic and Investigational Dermatology analyzed randomized controlled trials:
Efficacy by acne lesion type:
Comedonal acne (blackheads/whiteheads):
- 30-45% reduction in comedone count at 12 weeks
- "Moderate improvement" in 40-50% of patients
- Best results seen with 2% concentration
Inflammatory acne (papules/pustules):
- Only 15-25% reduction in inflammatory lesion count
- "Minimal to no improvement" in 50-60% of patients
- Significantly underperforms compared to benzoyl peroxide or topical antibiotics
Important context: The majority of teenage acne is inflammatory, not purely comedonal. This means salicylic acid targets the less problematic component of most patients' acne while leaving the more visible, painful lesions largely untouched.
Comparative trials show:
- Less effective than topical retinoids (adapalene, tretinoin) for all acne types
- Less effective than benzoyl peroxide for inflammatory acne
- Similar efficacy to glycolic acid but with more irritation potential
Side Effects and Skin Reactions
The perception of salicylic acid as "gentle" doesn't align with dermatological evidence. Clinical trials document notable side effect rates that often surprise patients:
Skin Barrier Disruption (25-40% of users)
Salicylic acid works by disrupting the skin's outermost layer. This mechanism inherently compromises barrier function:
Common symptoms:
- Increased transepidermal water loss (clinically measured)
- Tightness and dehydration
- Increased sensitivity to other products
- Paradoxical increase in oil production (rebound effect)
Medical significance: A compromised skin barrier can actually worsen acne by allowing bacterial penetration and triggering inflammatory cascades. In clinical practice, I've observed patients whose acne improved after stopping salicylic acid, not starting it.
Contact Irritation (20-35% of users)
Irritant contact dermatitis from salicylic acid presents as:
- Redness and inflammation
- Burning or stinging (especially around eyes and mouth)
- Dry patches and flaking
- Increased sun sensitivity
Duration: Unlike benzoyl peroxide where irritation sometimes subsides after 4-6 weeks, salicylic acid irritation often persists throughout use because barrier damage is cumulative.
Salicylate Sensitivity (Rare but Serious)
Approximately 1-2% of the population has aspirin/salicylate sensitivity. Using salicylic acid topically can trigger:
- Widespread facial redness
- Hives or rash beyond application area
- Respiratory symptoms in severe cases
Medical alert: If you have aspirin allergy or asthma, consult a physician before using salicylic acid products.
Systemic Absorption Concerns
While uncommon with facial use, salicylic acid can be absorbed systemically, particularly with:
- Large application areas (full back/chest)
- Higher concentrations (professional peels at 20-30%)
- Damaged or inflamed skin
Documented effects of systemic absorption:
- Salicylism (ringing in ears, nausea, dizziness)
- Pregnancy concerns (FDA Category C)
Clinical recommendation: Pregnant or nursing women should avoid salicylic acid products unless specifically approved by their obstetrician.
When Salicylic Acid Falls Short
Based on clinical evidence and treatment outcomes, salicylic acid has limited utility for:
Inflammatory Acne
If your acne consists primarily of red, inflamed pimples rather than blackheads:
- Published data shows only 15-25% improvement
- Prescription options (retinoids, benzoyl peroxide combinations) show 40-60% improvement
- The difference in efficacy is clinically and cosmetically significant
Moderate to Severe Acne
For acne involving:
- More than 20-30 active lesions
- Nodules or cysts
- Scarring or post-inflammatory hyperpigmentation
Medical perspective: Salicylic acid is inadequately powered for these conditions. Using it as first-line treatment delays more effective intervention and risks permanent scarring.
Hormonal Acne
Teenage acne is largely hormonally driven. Salicylic acid has no mechanism to address:
- Androgen-stimulated sebum production
- Hormone-responsive inflammatory pathways
- Cyclical breakout patterns
Dark Skin Tones
For patients with Fitzpatrick skin types IV-VI:
- Post-inflammatory hyperpigmentation (dark marks after pimples) is often the primary concern
- Salicylic acid irritation can worsen hyperpigmentation
- Prescription retinoids or targeted hyperpigmentation treatments often yield better outcomes
Realistic Timeline and Usage
If salicylic acid is appropriate for your acne type (primarily comedonal), clinical data suggests:
Week 1-3: Expect dryness and potential increased breakouts as pores purge. No visible improvement.
Week 4-6: Early responders see reduction in blackheads. Non-responders see no change.
Week 8-12: Maximum benefit achieved for comedones. If inflammatory acne persists unchanged, continued use won't help.
Beyond 12 weeks: Maintenance phase. Salicylic acid won't provide additional improvement, only sustain existing results.
Proper Use to Minimize Side Effects
If proceeding despite these limitations:
Concentration: Start with 0.5-1%, not 2%
Frequency: Every other day for first month
Application: To dry skin only, avoiding eye and mouth areas
Moisturizer: Non-comedogenic moisturizer essential to offset barrier disruption
Sun protection: Daily SPF 30+ required due to increased photosensitivity
Product Formulation Matters
Salicylic acid efficacy depends heavily on formulation factors rarely disclosed on labels:
pH dependency: Salicylic acid requires pH 3-4 to remain active. Many drugstore products have pH 5-6, rendering the ingredient largely ineffective.
Concentration versus availability: A 2% salicylic acid product at pH 5 delivers less active ingredient than a 0.5% product at pH 3.5.
Clinical implication: Patients often use ineffective formulations, see no results, then blame themselves for "not using it long enough" when the product itself was poorly formulated.
Combination Product Concerns
Salicylic acid frequently appears in products alongside:
Benzoyl peroxide: Additive irritation without synergistic benefit
Retinoids: Can inactivate tretinoin if applied simultaneously
Other acids (glycolic, lactic): Increases pH instability and irritation
Medical recommendation: Single-ingredient products allow better assessment of efficacy and side effect attribution.
Cost-Benefit Analysis
From a medical economics perspective:
Salicylic acid products: $8-25 per bottle, lasting 1-2 months Generic tretinoin (prescription): $15-40 with insurance for 3 months supply Generic adapalene (now OTC): $12-20 for 3 months
Efficacy comparison:
- Salicylic acid: 20-35% lesion reduction (primarily blackheads)
- Adapalene: 40-60% lesion reduction (all lesion types)
- Tretinoin: 50-70% lesion reduction (all lesion types)
Analysis: Prescription retinoids cost similar or less while providing significantly superior outcomes for most acne types.
Bottom Line
Salicylic acid has documented but limited efficacy in acne treatment, working primarily on non-inflammatory blackheads and whiteheads while showing minimal effect on the inflammatory lesions that constitute most teenage acne. Clinical trials demonstrate only 20-35% improvement in total lesion counts after 12 weeks of consistent use, with 50-60% of patients seeing minimal to no improvement. Side effects including skin barrier disruption, irritation, and increased sensitivity occur in 25-40% of users. The characterization of salicylic acid as a "gentle" alternative is not supported by side effect data. For patients with predominantly comedonal acne and resilient skin, a careful trial may be reasonable. However, for inflammatory acne, darker skin tones, or sensitive skin, alternative treatments—particularly OTC adapalene or prescription retinoids—offer superior efficacy with manageable side effects when used correctly. If you try salicylic acid, use the lowest effective concentration (0.5-1%), expect a 12-week trial period, and discuss prescription alternatives with your dermatologist if results are unsatisfactory.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Arif T. Salicylic acid as a peeling agent: a comprehensive review. Clin Cosmet Investig Dermatol. 2015https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4554394/
- Kornhauser A, et al. Applications of hydroxy acids: classification, mechanisms, and photoactivity. Clin Cosmet Investig Dermatol. 2010
Read This Next

Niacinamide for Acne: The Gentle Ingredient That Does Everything

Azelaic Acid for Acne: The Underrated Treatment Teens Should Know About

Adapalene (Differin) for Teens: The Complete Starter Guide

Natural vs. Medicated Acne Treatments: What the Evidence Actually Shows
Tea tree oil has real data behind it, but most 'natural' acne products are marketing hype. Here's what the research says about natural vs. medicated treatments — and why the best approach might combine both.
Read More →
Drugstore vs. Prescription Acne Products: When to Upgrade
Most teens don't need a prescription to clear their skin. Here's how to tell if drugstore products are enough -- and when it's time to see a dermatologist.
Read More →