Testosterone and Acne: Why Hormones Drive Most Teen Breakouts
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Team — Updated May 15, 2026
Key takeaways
- Testosterone doesn't directly cause acne. It gets converted to DHT by an enzyme called 5-alpha reductase, and DHT is what actually enlarges oil glands and increases sebum production.
- Boys produce roughly 10-20 times more testosterone than girls, which is why male adolescent acne tends to be more severe and widespread, particularly on the back and chest.
- Girls still get hormonal acne because their adrenal glands and ovaries produce androgens too. Even relatively small hormonal shifts can trigger breakouts, especially around the menstrual cycle.
- Topical retinoids reduce androgen receptor sensitivity in skin cells, which is one reason they work so well for acne beyond just unclogging pores.
- Hormone-balancing supplements have no credible evidence for treating acne. The hormonal changes of puberty are normal biology, not something that needs correcting with zinc or saw palmetto.
Most acne advice focuses on what you put on your face. Wash with this, apply that, don't touch your skin. And that stuff matters. But it kind of skirts around the actual reason most teenagers break out in the first place, which is hormonal. Specifically, it's testosterone.
Not in a vague "hormones are changing" way. In a very specific, well-mapped biochemical pathway that dermatologists have understood for decades. If you want to know why your acne started when it did, why it's as bad as it is, and why certain treatments work better than others, you need to understand what testosterone is doing to your oil glands. So let's get into it.

The testosterone-DHT-sebum pathway
Testosterone itself doesn't cause acne directly. What happens is more specific than that.
Your skin contains an enzyme called 5-alpha reductase. This enzyme converts testosterone into a more potent androgen called dihydrotestosterone, or DHT. DHT is somewhere around 5 to 10 times more potent than testosterone at binding to androgen receptors, and your sebaceous (oil) glands are loaded with these receptors.
When DHT binds to the androgen receptors on sebaceous gland cells, it triggers those glands to grow larger and produce more sebum. A 1993 study published in the Journal of Clinical Endocrinology & Metabolism demonstrated this clearly: individuals with a genetic deficiency in 5-alpha reductase (meaning they couldn't convert testosterone to DHT) had significantly less sebum production and essentially no acne. Their testosterone levels were normal. They just couldn't make DHT. And without DHT, their oil glands stayed small and quiet.
This is the core mechanism. More DHT reaching your oil glands means more oil. More oil means a better environment for Cutibacterium acnes bacteria. More bacteria means more inflammation. More inflammation means pimples.
The reason this matters beyond biology class is that it explains why acne treatments work the way they do. Retinoids don't just unclog pores. They actually reduce the sensitivity of androgen receptors in the skin, making your oil glands less responsive to DHT. That's a hormonal effect from a topical product. It also explains why some people with normal testosterone levels still get terrible acne: their skin may have more 5-alpha reductase activity, more androgen receptors, or more sensitive receptors. The amount of testosterone in your blood is only part of the story. What your skin does with it locally is the rest.
Why boys tend to get worse acne
This part is pretty straightforward. During puberty, boys start producing testosterone in much larger quantities. By the end of puberty, males have roughly 10 to 20 times the circulating testosterone of females. The adrenal glands contribute some, but the majority comes from the testes.
More circulating testosterone means more raw material for conversion to DHT. More DHT means more sebum. And because male adolescents also tend to have more androgen receptors in their trunk skin (back, chest, shoulders), boys are more likely to develop severe acne in those areas.

A 2004 review in Clinical Dermatology by Zouboulis and colleagues laid out the androgen-sebaceous gland relationship in detail, noting that androgen levels correlate with both sebum production rates and acne severity across multiple studies. The correlation isn't perfect (some high-testosterone individuals have clear skin, some low-testosterone individuals break out badly), but the overall trend is consistent.
The severity difference is real. Studies on acne prevalence consistently show that adolescent males are more likely to have moderate-to-severe acne than adolescent females, and more likely to develop the deep, cystic lesions that lead to scarring. This isn't because boys are worse at skincare. It's because they have more of the hormone that drives sebum production.
This is also why male acne tends to improve in the late teens and early twenties for many people. Not because testosterone drops (it doesn't, really), but because the rapid hormonal surge stabilizes. Your oil glands adjust. Your skin's response to androgens calms down. The "puberty spike" passes, even though testosterone levels remain high.
Why girls still get hormonal acne
If testosterone is the main driver and boys have way more of it, why do girls get acne at all? It's a fair question with a slightly complicated answer.
Girls and women produce androgens from two sources: the adrenal glands and the ovaries. The total amount is much less than what males produce, but it's not zero. And for acne, you don't need a lot. Even modest levels of androgens, if they're being efficiently converted to DHT in the skin, can produce enough sebum to trigger breakouts.
There's also the fluctuation factor. Female hormone levels don't stay constant. They cycle monthly, with shifts in estrogen, progesterone, and androgens across the menstrual cycle. The period right before menstruation is when progesterone drops and the relative androgen influence increases, which is why so many girls and women notice breakouts in the week before their period. It's not that androgen levels spike dramatically. It's that the estrogen-to-androgen ratio shifts just enough to tip the balance toward more oil production.
A 1994 study by Lucky et al. in Archives of Dermatology found that girls with acne had higher levels of the adrenal androgen DHEA-S (dehydroepiandrosterone sulfate) compared to girls without acne, even before menarche. This suggests that the adrenal contribution to androgen-driven acne starts early and may partly explain why some girls develop acne before their periods even begin.
Some girls also have conditions that increase androgen production beyond typical levels. Polycystic ovary syndrome (PCOS) is the most common, affecting an estimated 6-12% of women of reproductive age. PCOS often involves elevated androgen levels, and persistent acne (especially along the jawline and chin) is one of its clinical features. If your acne is severe, persistent, and accompanied by irregular periods, excessive hair growth, or other hormonal symptoms, it's worth asking a doctor about PCOS specifically.
The puberty surge timeline
Acne doesn't just appear one day at full blast. It follows the hormonal timeline of puberty, which itself follows a fairly predictable sequence.
For boys, adrenal androgens (mainly DHEA-S) start rising around age 7-8, well before any visible signs of puberty. This is called adrenarche. Testicular testosterone production kicks in later, usually around age 10-12, and increases steadily through mid-puberty. Peak testosterone production typically occurs between ages 15-18. Acne tends to follow this curve, appearing first in mild form around 11-13 and peaking in severity around 15-17.
For girls, the adrenal androgen rise follows a similar timeline, but the ovarian contribution adds another layer. Acne may appear as early as 9-10 (driven by adrenal androgens) and often intensifies around menarche (average age 12-13). Female acne sometimes has a second peak in the late teens to early twenties and can persist longer into adulthood than male acne, particularly when it's driven by cyclic hormonal fluctuations.
What I find interesting about this timeline is that it explains a pattern many teens notice but can't articulate: your acne gets worse even when you're doing everything "right." You might be washing your face, using the products your dermatologist recommended, eating well, sleeping enough, and still, at 15 or 16, your acne is worse than it was at 13. That's not because you're failing. That's because your testosterone levels are still climbing, and your oil glands are responding accordingly.
This is temporary. The hormonal surge doesn't last forever. But "temporary" in puberty terms can mean years, which is cold comfort when you're in the middle of it.
No, supplements won't balance your hormones
I need to be direct about this because the marketing is aggressive and teens are especially vulnerable to it.
There is an entire industry selling supplements that claim to "balance your hormones" and clear acne from the inside out. Zinc, DIM (diindolylmethane), saw palmetto, vitex (chasteberry), spearmint capsules, adaptogenic herbs. The packaging is clean, the testimonials are glowing, and the prices are high.
The evidence for most of these is thin to nonexistent for acne specifically.
Zinc has some legitimate research behind it for acne. A handful of studies have shown modest benefit from oral zinc supplementation, though the effect sizes are small compared to conventional treatments and high-dose zinc can cause nausea and copper deficiency. If you're zinc-deficient, supplementing may help. If you're not, it probably won't do much.
DIM and saw palmetto are marketed as natural anti-androgens. The mechanistic logic isn't crazy (saw palmetto does inhibit 5-alpha reductase in prostate tissue), but the clinical evidence for acne treatment in humans is essentially absent. There are no large, controlled trials showing these supplements clear acne.
The larger problem is the framing. The hormonal changes of puberty are not a disease. Your testosterone rising during adolescence is not a hormonal imbalance that needs correcting. It's normal development. When someone sells you a supplement to "balance" this process, they're treating healthy biology as a problem and offering an unproven solution.
That doesn't mean hormonal acne treatments don't exist. They do. But the ones that work are pharmaceuticals with actual clinical trials behind them, not supplements with Instagram ads.
What actually helps
Given that androgens are driving the process, what treatments actually address the hormonal component of acne?

Topical retinoids (tretinoin, adapalene, tazarotene). These are the foundation of acne treatment for good reason. A 2017 review in Dermatologic Therapy explained that retinoids work through multiple mechanisms: they normalize the shedding of cells inside the pore (preventing clogs), they reduce inflammation, and they decrease the expression of androgen receptors in sebaceous glands. That last mechanism is often overlooked. By making your oil glands less sensitive to DHT, retinoids address the hormonal driver of acne at the skin level. They don't change your blood hormone levels. They change how your skin responds to those hormones.
Benzoyl peroxide doesn't have a hormonal mechanism, but it kills the bacteria that thrive in the excess oil that androgens create. It's a practical downstream solution. You can't stop the oil production entirely, but you can control what grows in it.
Spironolactone is an anti-androgen medication that blocks androgen receptors. It's used off-label for acne in females (not typically prescribed for males because of its feminizing side effects like breast tenderness). A review in the Journal of the American Academy of Dermatology noted that spironolactone at doses of 50-200mg daily significantly reduced acne in women with hormonal breakout patterns. It's a prescription medication with real side effects, so it's not a first-line option, but for women with acne that doesn't respond to topical treatments, it directly addresses the androgen pathway.
Combined oral contraceptives (for females) contain estrogen, which increases sex hormone-binding globulin (SHBG). SHBG binds to free testosterone in the blood, reducing the amount available for conversion to DHT. Several oral contraceptives are FDA-approved specifically for acne treatment. They take 2-3 months to show results and they're not appropriate for everyone, but they work through a genuinely hormonal mechanism.
Isotretinoin (Accutane) is the closest thing to a permanent solution for severe acne. It dramatically shrinks sebaceous glands, which directly addresses the overproduction of oil that androgens cause. The gland shrinkage persists long after you stop taking the drug, which is why many people experience lasting clearance. It has serious side effects and requires close monitoring, but for severe, scarring acne that hasn't responded to other treatments, it's often the right call.
What all these treatments have in common is that they've been tested in controlled clinical trials, have well-understood mechanisms, and are prescribed or recommended by dermatologists based on evidence. They are not the same category of thing as a supplement you saw advertised on TikTok.
Bottom line
Testosterone, converted to DHT by your skin's own enzymes, is the primary driver of most teen acne. It enlarges oil glands, increases sebum production, and creates the conditions for bacterial growth and inflammation. Boys get hit harder because they produce more testosterone. Girls still get hormonal acne because adrenal and ovarian androgens do the same thing at lower levels. The puberty surge is temporary but can last years. Supplements marketed as hormone balancers don't have the evidence to back their claims. Treatments that actually work on the hormonal pathway include topical retinoids (which reduce androgen receptor sensitivity), spironolactone (which blocks androgen receptors), oral contraceptives (which reduce free testosterone), and isotretinoin (which shrinks oil glands). Talk to a dermatologist about which approach makes sense for your situation.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zouboulis CC, et al. Androgens and sebaceous gland function. Clin Dermatol. 2004;22(5):360-366https://pubmed.ncbi.nlm.nih.gov/15556719/
- Imperato-McGinley J, et al. The androgen control of sebum production. Studies of subjects with dihydrotestosterone deficiency and complete androgen insensitivity. J Clin Endocrinol Metab. 1993;76(2):524-528https://pubmed.ncbi.nlm.nih.gov/8432797/
- Thiboutot D. Acne: hormonal concepts and therapy. Clin Dermatol. 2004;22(5):419-428https://pubmed.ncbi.nlm.nih.gov/15556729/
- Lucky AW, et al. Acne vulgaris in premenarchal girls. Arch Dermatol. 1994;130(3):308-314https://pubmed.ncbi.nlm.nih.gov/8129408/
- Zaenglein AL, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973https://pubmed.ncbi.nlm.nih.gov/26897386/
- Leyden J, et al. Why topical retinoids are mainstay of therapy for acne. Dermatol Ther. 2017;30(1):e12427https://pubmed.ncbi.nlm.nih.gov/27943559/
- Shaw JC. Spironolactone in dermatologic therapy. J Am Acad Dermatol. 1991;24(2 Pt 1):236-243https://pubmed.ncbi.nlm.nih.gov/1826112/
- Lai JJ, et al. The role of androgen and androgen receptor in skin-related disorders. Arch Dermatol Res. 2012;304(7):499-510https://pubmed.ncbi.nlm.nih.gov/22829073/
- Knutson DD. Ultrastructural observations in acne vulgaris: the normal sebaceous follicle and acne lesions. J Invest Dermatol. 1974;62(3):288-307https://pubmed.ncbi.nlm.nih.gov/4273657/
Read This Next

Inflammatory Acne: Papules, Pustules, and Why Your Skin Hurts
Inflammatory acne is the red, painful kind that actually hurts. Understanding the immune response behind it changes how you treat it and helps you stop making it worse.
Read More →
Comedonal Acne: Why Your Skin Is Bumpy But Not Red (And How to Fix It)
Comedonal acne gives you textured, bumpy skin without the redness of typical pimples. It's frustrating because it doesn't respond to the usual treatments. Here's what actually works.
Read More →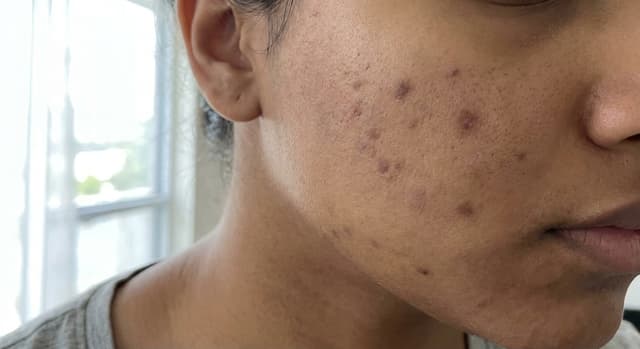
Acne Scars vs. Acne Marks: The Difference Matters for Treatment
Most teens say 'scars' when they mean 'marks,' and the treatments are completely different. Marks are flat and fade on their own. Scars change the texture of your skin and usually need professional help. Here's how to tell which you have.
Read More →
Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →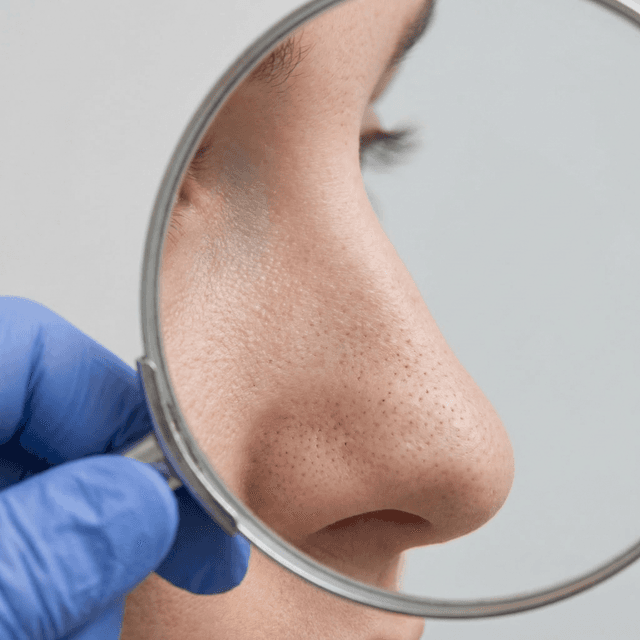
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →