Inflammatory Acne: Papules, Pustules, and Why Your Skin Hurts
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Team — Updated May 9, 2026
Key takeaways
- Inflammatory acne is a two-part problem. Bacteria multiply in a clogged pore AND your immune system overreacts to them, causing the redness and pain.
- Benzoyl peroxide kills the bacteria, retinoids prevent new clogged pores. Using both together attacks inflammatory acne from two directions, which is why dermatologists almost always recommend the combination.
- Squeezing an inflamed pimple pushes bacteria and inflammation deeper into the skin, increasing the risk of scarring and prolonging healing. Hands off.
- Niacinamide and azelaic acid can reduce inflammation without harsh side effects, making them good additions to a BP/retinoid routine.
- If your inflammatory acne isn't responding to topicals after 3 months, oral treatment may be needed. This isn't a failure. Some acne just needs more than what you can put on your face.
You know the difference between a bump you can ignore and a pimple that makes you wince when you accidentally touch it. That second one is inflammatory acne, and it's a different animal from the blackheads and whiteheads that just sit there looking textured. Inflammatory acne is red. It's swollen. It hurts. And it tends to leave marks behind in a way that non-inflammatory acne usually doesn't.
I think understanding why it hurts and why it's red actually changes how you approach treatment. Once you see what's happening below the surface, some common advice (like squeezing pimples, or using only one product) stops making sense, and other approaches suddenly click.

How a clogged pore becomes an inflamed one
Every inflammatory pimple starts as a comedone. A clogged pore. Dead skin cells mix with oil, form a plug, and block the follicle. Up to this point, it's just comedonal acne, bumpy but not painful.
The transition to inflammation happens when Cutibacterium acnes (C. acnes) gets involved. These bacteria live naturally on everyone's skin and inside every pore. They're part of the normal skin microbiome. But when a pore gets plugged, the environment inside changes. Oxygen levels drop. Sebum accumulates. And C. acnes, which feeds on sebum, starts multiplying rapidly in that oxygen-poor, oil-rich environment.
Here's where it gets interesting. The bacteria themselves don't actually cause much direct damage. What happens instead is that as C. acnes multiplies, it produces enzymes (lipases) that break down sebum into free fatty acids, and it releases proteins that your immune system recognizes as a threat. Your body sends white blood cells (neutrophils, primarily) to the site, and those immune cells release inflammatory chemicals as they try to contain the bacteria.
The redness, swelling, and pain you see on the surface is mostly your own immune system's response to the bacteria, not the bacteria themselves. This is a key distinction because it means effective treatment needs to address both the bacterial overgrowth AND the inflammatory response.
A 2013 review in the Journal of Clinical and Aesthetic Dermatology by Tanghetti made the case that inflammation in acne actually begins earlier than we used to think. Even comedones that look non-inflammatory under a microscope show elevated levels of inflammatory markers like IL-1 and TNF-alpha. So inflammation may be simmering from the very beginning, and what we call "inflammatory acne" is when it becomes visible and symptomatic.
Papules vs pustules
Both are inflamed, but they look different and represent slightly different stages of the process.
A papule is a small, raised, red bump without a visible white center. It's solid to the touch and tender. Under the skin, the pore wall has started to break down from the pressure of the inflammatory response, and immune cells are flooding the area. But there's no collection of pus at the surface yet.
A pustule is what most people picture when they think "pimple." It's red at the base with a white or yellowish center. That center is pus, which is a collection of dead neutrophils, bacteria, and cellular debris. The immune system has been fighting the infection for a while, and the casualties are visible.
Papules sometimes resolve on their own as the immune system gets the bacteria under control. They can also progress to pustules. Pustules can drain spontaneously (the white head opens) or they can go deeper and become nodules if the pore wall ruptures underneath the skin. That deeper rupture is what leads to nodular or cystic acne, which is a whole different conversation.
For treatment purposes, papules and pustules respond to the same approach. The distinction is mostly useful for communicating with your dermatologist and tracking the severity of your acne over time.
Why inflammatory acne hurts
The pain isn't random. There are specific nerves in the dermis (the deeper layer of skin) surrounded by pressure-sensitive receptors, and inflammation activates them in two ways.
First, the swelling itself creates physical pressure. As immune cells and fluid accumulate around the infected pore, the tissue expands, pressing on nerve endings. Bigger pimples hurt more because there's more swelling.
Second, the inflammatory chemicals released by your immune system (prostaglandins, histamines, bradykinin) directly sensitize nerve endings, lowering their threshold for firing. This is why even a light touch on an inflamed pimple can feel disproportionately painful. The nerves in that area are essentially turned up to maximum sensitivity.

Icing a painful pimple actually makes biological sense here. Cold constricts blood vessels (reducing the flow of inflammatory cells to the area) and numbs the nerve endings temporarily. It won't treat the pimple, but it can take the edge off the pain. Wrap an ice cube in a thin cloth and hold it on the spot for 5-10 minutes. Don't put ice directly on skin.
The inflammation cascade (simplified)
I'm going to simplify this because the full immunology is genuinely complicated, but the general sequence matters for understanding why certain treatments work.
Step 1: Clogged pore fills with sebum. C. acnes multiplies in the low-oxygen, oil-rich environment.
Step 2: C. acnes produces lipases and releases toll-like receptor ligands. Your skin's innate immune system detects these.
Step 3: Keratinocytes (skin cells) and sebocytes (oil gland cells) release pro-inflammatory cytokines, including IL-1alpha, IL-8, and TNF-alpha. These are chemical alarm signals.
Step 4: Neutrophils (a type of white blood cell) are recruited to the site. They arrive through dilated blood vessels, which is why the area turns red. The blood vessels become leaky, which is why the area swells.
Step 5: Neutrophils try to engulf the bacteria and release enzymes in the process. These enzymes damage surrounding tissue, including the pore wall. If the pore wall breaks, the contents spill into the surrounding dermis, which triggers even more inflammation.
Step 6: The body eventually contains the infection and starts repairing the damage. This repair process can leave behind post-inflammatory hyperpigmentation (dark marks) or scarring if the tissue damage was severe enough.
The whole sequence, from initial bacterial overgrowth to visible pimple, can take days to weeks. And the resolution, from active pimple to healed skin, takes another 1-4 weeks for a typical pustule, longer if scarring occurs.
Treatment: benzoyl peroxide and retinoids together
This combination is the standard of care for mild to moderate inflammatory acne, and it works because it attacks the problem from two angles.

Benzoyl peroxide (2.5-5%) kills C. acnes through oxidation. It releases free oxygen radicals inside the pore, which the anaerobic (oxygen-hating) bacteria can't survive. Unlike topical antibiotics, C. acnes doesn't develop resistance to benzoyl peroxide, even with long-term use. This is important because antibiotic resistance in acne bacteria is a growing problem worldwide.
The 2.5% concentration works about as well as 10% for most people but causes less irritation. A 2009 study in the Journal of the American Academy of Dermatology confirmed this. Going higher on the concentration mainly gets you more dryness and redness without proportional improvement in bacterial kill.
Adapalene (0.1%) is a retinoid that normalizes how skin cells shed inside the pore, preventing the comedone formation that starts the whole cascade. It also has direct anti-inflammatory properties, which is something earlier retinoids like tretinoin didn't have as strongly.
Using both: apply benzoyl peroxide in the morning and adapalene at night. Or use a combination product like Epiduo, which contains both in one tube. The AAD's 2016 guidelines recommend combination therapy as first-line for inflammatory acne specifically because using only one product leaves half the problem unaddressed.
A note about the adjustment period: when you start both products at once, your skin is going to protest. Dryness, peeling, some stinging. This is normal and it fades over 2-4 weeks as your skin adapts. If it's unbearable, start with one product (I'd choose adapalene first since it takes longer to work) and add BP after a few weeks.
Anti-inflammatory ingredients worth trying
Beyond the standard BP/retinoid combo, there are ingredients that specifically target the inflammation component. These aren't replacements for BP or retinoids, but they can reduce redness and speed healing alongside the main treatment.
Niacinamide (vitamin B3, 4-5%) is one I think deserves more attention than it gets. It inhibits the transfer of melanosomes to keratinocytes (reducing post-inflammatory dark marks), strengthens the skin barrier, and has demonstrated anti-inflammatory effects in multiple studies. It's well-tolerated by almost everyone and doesn't interact badly with other actives. You can layer it with retinoids and BP without issues.
Azelaic acid (10-15% OTC, 15-20% prescription) has both anti-inflammatory and antibacterial properties, and it also inhibits melanin production. It's particularly useful if you're dealing with both active inflammation and dark marks left behind by old pimples. It's gentler than BP for many people and works well as a morning treatment alongside an evening retinoid.
Sulfur (2-10%) is an older ingredient that still works. It's mildly antibacterial and helps absorb excess oil. Some spot treatments and masks contain sulfur as the active ingredient. The main downside is the smell, which is exactly what you'd expect from sulfur.
What I'd skip: tea tree oil. There's some evidence it has mild antibacterial properties, but the effective concentration is irritating for a lot of people, and the studies comparing it to BP show it works more slowly and less completely. It's not terrible, but when you have proven options available, I'm not sure why you'd go with the weaker one.
Why squeezing makes inflammatory acne so much worse
I know you've heard "don't pop your pimples" a thousand times. But I think the reason matters more than the rule, because understanding the mechanism might actually stop you from doing it.
When you squeeze an inflamed papule or pustule, you're applying pressure to an already-fragile pore wall. Remember, the inflammation has been breaking down that wall from the inside. External pressure can rupture it completely, pushing bacteria, pus, and inflammatory chemicals deeper into the dermis instead of out through the surface.
This is worse than it sounds. When that contaminated material spreads into surrounding tissue, your immune system launches a much larger response. What was one pimple can become a cluster. What was a superficial pustule can become a deep, painful nodule. And the tissue damage from this deeper inflammation is what causes permanent scarring.
A 2010 review in Dermatology Research and Practice on acne scar pathogenesis found that mechanical manipulation of lesions (i.e., picking and squeezing) was a consistent risk factor for scar formation. The inflammatory damage goes deeper when you intervene physically, and deeper damage means more collagen destruction and a harder repair job for your skin.
Even when you successfully extract the contents of a pustule, you've still created an open wound. That wound can get reinfected (your fingers are covered in bacteria), and the healing process often leaves a more visible mark than if you'd left the pimple alone.
The hardest part of this advice is that sometimes pimples do drain on their own, and the relief is immediate. But there's a difference between a pimple that has naturally come to a head and drains with almost no pressure versus one that you're digging at with your fingernails. If you absolutely can't resist, at least wait until there's a visible white head at the surface, wash your hands, and use gentle pressure with tissue-covered fingers. But honestly, a hydrocolloid pimple patch applied overnight will do the same job without the tissue damage.
When topicals aren't enough
There's a point where topical treatments hit their ceiling. If you've been using a proper BP/retinoid combination for 3 months and you're still getting frequent inflammatory breakouts, especially if they're deep or painful, it's time to talk to a dermatologist about oral options.
This isn't a failure of your routine or your skin. Some people's acne is driven more heavily by hormonal factors, or their particular strain of C. acnes is more virulent, or the inflammatory response is just more aggressive than what topicals can contain. The biology isn't your fault, and recognizing when you need stronger tools is smart, not giving up.
Oral options include:
Antibiotics (usually doxycycline or minocycline) reduce both bacterial load and inflammation. They're typically prescribed for 3-6 months alongside topicals and then discontinued to avoid resistance issues. They're not a long-term solution, but they can break the cycle and bring things under control while topicals take effect.
Hormonal treatments (for girls/women) like combined oral contraceptives or spironolactone can address the androgen-driven oil production that fuels inflammatory acne. These are particularly worth considering if breakouts consistently track with your menstrual cycle or concentrate along the jawline and chin.
Isotretinoin (Accutane) is the nuclear option. It shrinks oil glands, reduces sebum production, and can produce long-term or permanent remission. It has real side effects and requires close monitoring, but for severe inflammatory acne that doesn't respond to other treatments, it can be genuinely transformative.
The point is: there's always a next step. If what you're doing isn't working after a fair trial, you don't have to just live with it.
Bottom line
Inflammatory acne is your immune system overreacting to bacteria trapped in clogged pores. The redness, swelling, and pain are all signs of that immune response, not just "bad skin." Treatment works best when it hits both sides of the equation: benzoyl peroxide to kill bacteria and a retinoid like adapalene to stop new pores from clogging. Anti-inflammatories like niacinamide and azelaic acid can help with the redness and marks left behind. Don't squeeze inflamed pimples because you'll push the infection deeper and increase your scarring risk. And if topicals alone aren't cutting it after 3 months of consistent use, oral treatment exists and works. Talk to a dermatologist.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973https://pubmed.ncbi.nlm.nih.gov/26897386/
- Dreno B, et al. Understanding innate immunity and inflammation in acne. J Eur Acad Dermatol Venereol. 2015;29(Suppl 4):3-11https://pubmed.ncbi.nlm.nih.gov/26059728/
- Tanghetti EA. The role of inflammation in the pathology of acne. J Clin Aesthet Dermatol. 2013;6(9):27-35https://pubmed.ncbi.nlm.nih.gov/24062871/
- Kraft J, Freiman A. Management of acne. CMAJ. 2011;183(7):E430-435https://pubmed.ncbi.nlm.nih.gov/21398228/
- Fabbrocini G, et al. Acne scars: pathogenesis, classification and treatment. Dermatol Res Pract. 2010;2010:893080https://pubmed.ncbi.nlm.nih.gov/20981308/
- Draelos ZD, et al. Niacinamide-containing facial moisturizer improves skin barrier and benefits subjects with rosacea. Cutis. 2005;76(2):135-141https://pubmed.ncbi.nlm.nih.gov/16209160/
- Thiboutot D, et al. New insights into the management of acne: an update from the Global Alliance to Improve Outcomes in Acne group. J Am Acad Dermatol. 2009;60(5 Suppl):S1-50https://pubmed.ncbi.nlm.nih.gov/19376456/
- Simonart T. Newer approaches to the treatment of acne vulgaris. Am J Clin Dermatol. 2012;13(6):357-364https://pubmed.ncbi.nlm.nih.gov/22920095/
Read This Next

Comedonal Acne: Why Your Skin Is Bumpy But Not Red (And How to Fix It)
Comedonal acne gives you textured, bumpy skin without the redness of typical pimples. It's frustrating because it doesn't respond to the usual treatments. Here's what actually works.
Read More →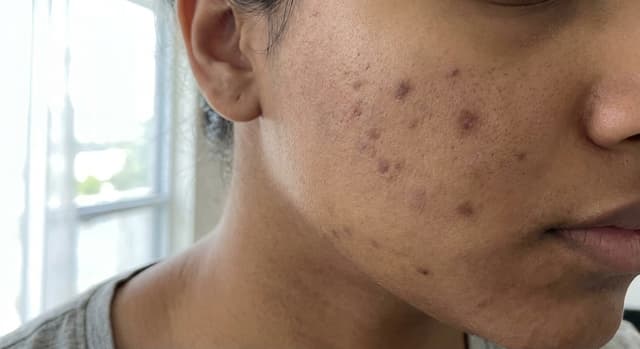
Acne Scars vs. Acne Marks: The Difference Matters for Treatment
Most teens say 'scars' when they mean 'marks,' and the treatments are completely different. Marks are flat and fade on their own. Scars change the texture of your skin and usually need professional help. Here's how to tell which you have.
Read More →
Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →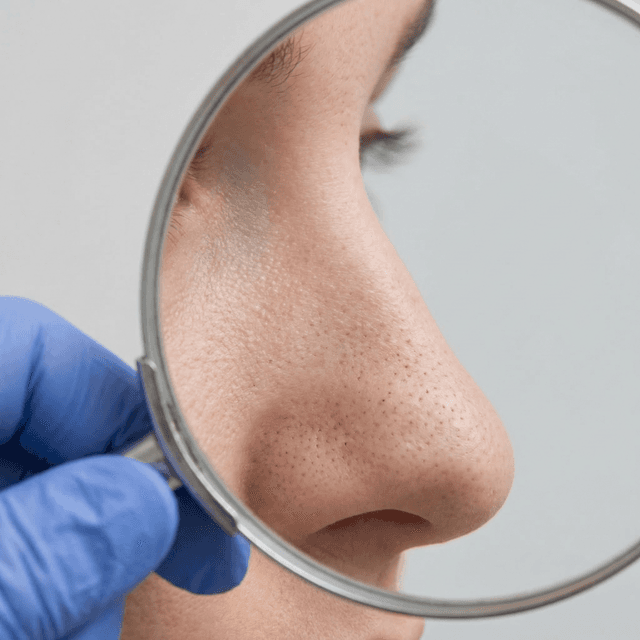
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →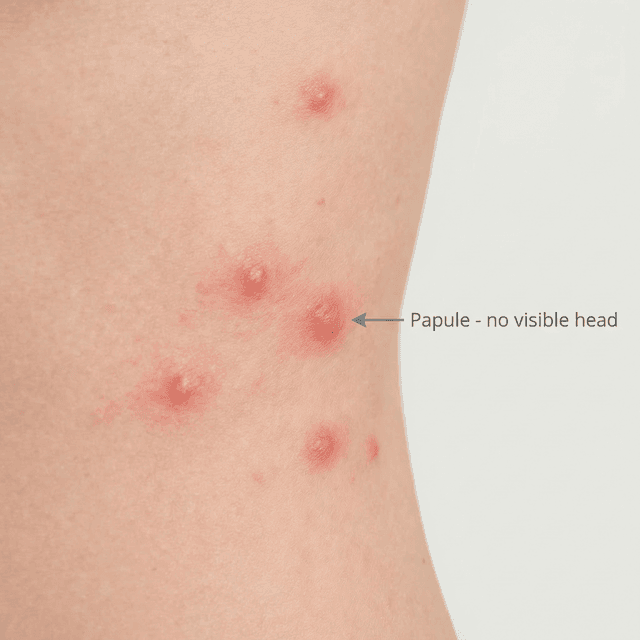
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →