Comedonal Acne: Why Your Skin Is Bumpy But Not Red (And How to Fix It)
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Team — Updated May 9, 2026
Key takeaways
- Comedonal acne is a clogging problem, not a bacteria problem. The bumps are plugged pores without significant inflammation, which is why antibacterial treatments like benzoyl peroxide don't do much for them.
- Adapalene (Differin) is the most effective OTC option because it normalizes how skin cells shed inside the pore, preventing the plugs from forming in the first place.
- Results take 8-12 weeks minimum. Comedones are slow to form and slow to clear. If you bail after three weeks because nothing's happening, you never gave the treatment a fair shot.
- Maintenance matters. The tendency to form comedones doesn't go away. Most people need to continue some form of retinoid or exfoliant use long-term, even after their skin looks clear.
If your forehead looks like sandpaper but nobody else can see why, you probably have comedonal acne. It's the type that doesn't photograph well. You can feel it with your fingers, the skin is rough and bumpy, but in pictures it just looks... fine. Which makes it harder to explain to people why it's bothering you.
I think comedonal acne is one of the more frustrating types because the usual advice doesn't apply. Slapping on benzoyl peroxide, washing your face more, spot-treating individual bumps. None of that really works here. The problem is fundamentally different from the red, angry pimples most people think of when they hear "acne," and the treatment needs to be different too.

What comedonal acne actually is
A comedone is a clogged pore. That's it. Dead skin cells that should have shed normally instead got stuck together inside the pore, mixed with sebum (your skin's natural oil), and formed a plug. The pore is blocked, but there's no real infection happening and your immune system hasn't gotten involved yet. So you get a bump without redness, without pus, without pain.
This distinction matters because it determines what treatment will work. Inflammatory acne (the red, painful kind) involves bacteria multiplying in the clogged pore and your immune system reacting to that. Comedonal acne is purely mechanical. It's a plumbing problem. The pipe is blocked, but nothing's infected.
Dermatologists classify comedones as either "open" (blackheads) or "closed" (whiteheads), and most people with comedonal acne have a mix of both, often concentrated in the same area.
Blackheads vs whiteheads (they're not what you think)
The difference between a blackhead and a whitehead is whether the pore opening is stretched wide or still covered by a thin layer of skin.
A blackhead (open comedone) has a wide opening at the surface. The plug of dead skin and oil is exposed to air, and it oxidizes. That's what makes it dark. It's not dirt. You could wash your face fifty times and the blackhead would still be dark because the color comes from a chemical reaction between the contents of the pore and oxygen. I mention this because the "dirt" myth leads people to over-wash, which irritates the skin and can actually make things worse.
A whitehead (closed comedone) is covered by a thin layer of skin. The plug is trapped underneath and doesn't oxidize, so it stays flesh-colored or slightly white. These are the small bumps you can feel but barely see, the ones that make your forehead feel textured. Closed comedones are generally harder to treat than blackheads because the pore opening is sealed and topical products have a harder time reaching the plug.
There's a misconception that whiteheads are the same as pustules (pimples with a white tip). They're not. A pustule is inflamed and filled with pus. A whitehead is not inflamed. It's just a small, firm bump under the skin.
Why your forehead gets it worst
If you have comedonal acne, there's a good chance your forehead is the main problem area. Maybe your nose too. Possibly your chin. But the forehead tends to be ground zero, and there's a reason for that.

The forehead is part of what dermatologists call the T-zone, the area with the highest concentration of sebaceous (oil) glands on the face. More oil glands means more sebum production, which means more raw material for those plugs to form.
But oil alone doesn't cause comedones. The other half of the equation is something called follicular hyperkeratinization, which is a clinical way of saying the skin cells lining the inside of your pores are behaving abnormally. Instead of shedding one at a time and flowing out with the oil, they're sticking together and building up. Androgens (hormones that increase during puberty) drive both processes: they stimulate oil production AND they seem to affect how cells behave inside the follicle.
Hair products can contribute too. Pomades, oils, gels, and heavy conditioners that get on your forehead create a specific variant called pomade acne, which is almost entirely comedonal. If your forehead acne started around the time you changed hair products, that's worth investigating.
Why benzoyl peroxide won't fix this
Here's where a lot of people waste months on the wrong approach.
Benzoyl peroxide is a great acne treatment. It kills Cutibacterium acnes (the bacteria involved in inflammatory acne) by releasing oxygen into the pore, and it's one of the few topical antibacterials that bacteria don't develop resistance to. For red, inflamed pimples, it's excellent.
But comedonal acne isn't primarily a bacterial problem. The bacteria are there, sure, but they're not the main issue. The main issue is that cells aren't shedding properly inside the pore. BP doesn't address that. It won't unclog an existing comedone or prevent new ones from forming through any meaningful mechanism.
The 2016 American Academy of Dermatology guidelines for acne management are pretty clear on this. For predominantly comedonal acne, the first-line recommendation is a topical retinoid, not benzoyl peroxide. BP is recommended as an add-on for inflammatory acne or to prevent antibiotic resistance when antibiotics are used. For comedones specifically, it's a secondary player at best.
This doesn't mean BP is useless if you have comedonal acne. Many people have a mix of comedonal and inflammatory acne, and BP handles the inflammatory component. But if your acne is mostly those non-red bumps, BP alone will disappoint you.
Retinoids: the one thing that consistently works
Retinoids are vitamin A derivatives that work by changing how skin cells grow, divide, and shed. When you apply a retinoid to your skin, it binds to receptors in the skin cells and alters their behavior. Specifically, it normalizes the desquamation process inside the follicle, meaning those sticky cells that were clumping together and forming plugs start shedding the way they're supposed to.
This is why retinoids are the gold standard for comedonal acne. They address the root cause rather than a symptom.
The most accessible option is adapalene 0.1% (Differin), which has been available over the counter in the US since 2016. Before that, you needed a prescription for any retinoid, which was a real barrier. Adapalene is a third-generation retinoid that's more stable and less irritating than older ones like tretinoin, while being roughly comparable in effectiveness for mild to moderate acne.
A few things to know about using adapalene:
Start slow. Every other night for the first two weeks, then build up to nightly. Your skin will probably get worse before it gets better, a phenomenon sometimes called "purging." What's happening is that the retinoid is speeding up the turnover of cells that were already forming plugs deep in the pore, so those comedones surface faster. This is temporary and usually lasts 4-6 weeks.
Use it at night. Retinoids break down in UV light and they make your skin more sensitive to the sun. Sunscreen during the day is non-negotiable while using any retinoid.
Moisturize. Dryness and peeling are the most common side effects. A simple, non-comedogenic moisturizer applied after the retinoid has absorbed (wait about 15 minutes) makes a big difference in tolerability.
Don't combine with too many other actives. Using a retinoid alongside benzoyl peroxide, salicylic acid, and glycolic acid all at once is a recipe for a destroyed skin barrier. Pick one active and let the retinoid do its work. If you want to add BP, apply it in the morning and the retinoid at night.
For more stubborn cases, prescription-strength retinoids like tretinoin (0.025% to 0.1%) or tazarotene are options your dermatologist might suggest. Tazarotene is the most potent but also the most irritating, so it's usually reserved for people who haven't responded to adapalene or tretinoin.
Chemical exfoliants as backup
If retinoids aren't tolerable (some people's skin just can't handle them, even with careful introduction), chemical exfoliants are the next best option for comedonal acne.
Salicylic acid (0.5-2%) is oil-soluble, which means it can penetrate into the pore and help dissolve the plug from the inside. Most over-the-counter acne washes and toners contain salicylic acid. It's gentler than retinoids for most people, but it's also less effective. I think of salicylic acid as a maintenance ingredient rather than a heavy lifter. It can keep things from getting worse, but it often can't clear established comedones on its own.
Glycolic acid (5-10%) is a water-soluble alpha hydroxy acid that works on the skin's surface. It dissolves the bonds between dead cells on the outer layer of skin, which can help prevent pore openings from getting blocked. It won't penetrate into the pore the way salicylic acid does, but it's useful for overall texture improvement.
Some people use both, alternating nights or using salicylic acid as a wash and glycolic acid as a leave-on treatment. Just be careful about overdoing it. Combining multiple exfoliants with a retinoid is a fast track to irritation, redness, and a compromised skin barrier, which ironically can make acne worse.
The patience problem
This is the part that nobody wants to hear, but I'm going to say it anyway because I think managing expectations is more useful than empty encouragement.
Comedonal acne is slow. Slow to develop, slow to respond to treatment, slow to clear. A comedone can take weeks to form deep in the pore before it's even visible on the surface. And because retinoids work by normalizing cell behavior over time rather than killing bacteria quickly, the treatment timeline is measured in months, not days.
The AAD and most dermatological guidelines say to give a retinoid at least 12 weeks before evaluating whether it's working. Twelve weeks. That's three months of applying something every night, possibly dealing with dryness and purging, before you can fairly judge the results.

Most people bail way before that. They try adapalene for three weeks, don't see a difference (or see things get worse during the purge), and conclude it doesn't work. Then they switch to something else, restart the clock, and never give anything enough time.
I get it. Three months is a long time when you're staring at bumpy skin every morning. But the biology doesn't care about your impatience. The cells inside your pores take time to normalize their behavior, and there's no way to rush that process.
One thing that can help mentally: take photos in the same lighting every two weeks. Day-to-day changes are invisible, but comparing week 1 to week 8 often reveals progress you couldn't see in the mirror.
Why it comes back when you stop
Here's the other part nobody wants to hear.
The tendency to form comedones is largely genetic and hormonal. Retinoids don't cure the underlying predisposition. They manage it. While you're using adapalene, your skin cells are shedding normally inside the pore. When you stop, they gradually revert to their old behavior.
This doesn't mean you're doomed to apply retinoid every night forever. Many people can step down to a maintenance schedule of 2-3 times per week and keep their skin clear. Some can switch to salicylic acid for maintenance after clearing with a retinoid. But completely stopping all treatment usually means the comedones come back within a few months.
A 2008 review in the American Journal of Clinical Dermatology looked at relapse rates after retinoid discontinuation and found that most patients experienced some return of comedonal lesions within 12 weeks of stopping treatment. The ones who continued a reduced-frequency retinoid maintained their improvement.
I know that's annoying. Nobody wants to be told they need to keep using a product indefinitely. But I think it's better to know this upfront than to be surprised and demoralized when the bumps return after you thought you'd beaten them.
Think of it like wearing a retainer after braces. The braces did the heavy lifting, but the retainer keeps things in place. The retinoid cleared your comedones, and a maintenance routine keeps them clear.
Bottom line
Comedonal acne is clogged pores without inflammation. It makes your skin bumpy and textured but not red. Benzoyl peroxide and antibacterials don't work well on it because the problem is abnormal cell shedding, not bacteria. Adapalene (available OTC as Differin) is the most effective treatment, but it takes a genuine 8-12 weeks to show results. Chemical exfoliants like salicylic acid and glycolic acid can help as alternatives or supplements. And because the tendency to form comedones is built into your skin, some form of ongoing maintenance treatment is usually needed to keep them from coming back.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973https://pubmed.ncbi.nlm.nih.gov/26897386/
- Leyden JJ. A review of the use of combination therapies for the treatment of acne vulgaris. J Am Acad Dermatol. 2003;49(3 Suppl):S200-210https://pubmed.ncbi.nlm.nih.gov/12963896/
- Thiboutot DM, et al. Adapalene-benzoyl peroxide, a fixed-dose combination for the treatment of acne vulgaris. Am J Clin Dermatol. 2007;8(4):237-243https://pubmed.ncbi.nlm.nih.gov/17645378/
- Thielitz A, Gollnick H. Topical retinoids in acne vulgaris: update on efficacy and safety. Am J Clin Dermatol. 2008;9(6):369-381https://pubmed.ncbi.nlm.nih.gov/18973403/
- American Academy of Dermatology. Acne: Diagnosis and treatment. AAD. 2024https://www.aad.org/public/diseases/acne/treatment/treatment
- Dreno B, et al. Understanding innate immunity and inflammation in acne. J Eur Acad Dermatol Venereol. 2015;29(Suppl 4):3-11https://pubmed.ncbi.nlm.nih.gov/26059728/
- Kircik LH. Tretinoin microsphere gel pump 0.04% vs tretinoin microsphere gel 0.1% for the treatment of acne vulgaris. J Clin Aesthet Dermatol. 2009;2(5):28-34https://pubmed.ncbi.nlm.nih.gov/20729946/
Read This Next

Inflammatory Acne: Papules, Pustules, and Why Your Skin Hurts
Inflammatory acne is the red, painful kind that actually hurts. Understanding the immune response behind it changes how you treat it and helps you stop making it worse.
Read More →
Acne Scars vs. Acne Marks: The Difference Matters for Treatment
Most teens say 'scars' when they mean 'marks,' and the treatments are completely different. Marks are flat and fade on their own. Scars change the texture of your skin and usually need professional help. Here's how to tell which you have.
Read More →
Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →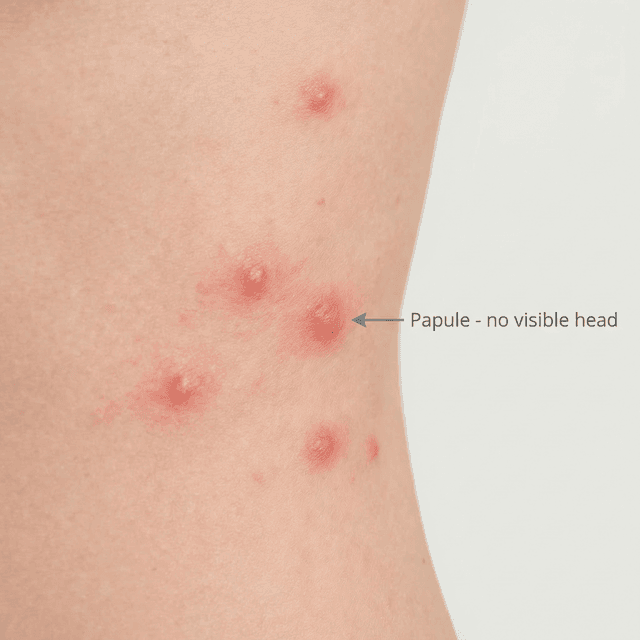
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →