Acne Scars vs. Acne Marks: The Difference Matters for Treatment
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Team — Updated May 1, 2026
Key takeaways
- Most of what teens call 'acne scars' are actually post-inflammatory marks that are flat, don't change skin texture, and fade on their own in 3-12 months.
- Dark marks (PIH) and red marks (PIE) need different treatments. Niacinamide and vitamin C help PIH. PIE is harder to treat topically and responds better to time and vascular lasers.
- True acne scars involve lost or excess collagen and don't improve without professional intervention. If you can feel an indentation or raised bump with your fingertip, that's a scar.
- Sunscreen is the single most important product for fading marks. UV exposure darkens PIH and slows the healing of both PIH and PIE. Daily SPF 30+ is non-negotiable if you're trying to fade post-acne marks.
- Most professional scar treatments are recommended for patients 18+ because the skin is still changing during adolescence. Talk to a dermatologist about timing.
Almost every teen I've talked to about their skin has used the word "scars" at some point. "I'm getting scars." "How do I get rid of my scars?" It makes sense. When acne leaves a mark behind, calling it a scar feels right.
But in most cases, what they're looking at isn't a scar. It's a mark. And the difference between those two things matters a lot, because the treatments are completely different and one of them goes away on its own while the other one doesn't.
Why this distinction matters
If you have flat, discolored spots where pimples used to be, whether they're brown, purple, or reddish, those are post-inflammatory marks. They're a normal part of the healing process. They look bad, and they can last for months, but they're temporary. The treatments that speed them up are relatively simple and affordable.
If you have actual texture changes, little indentations, pitted areas, or raised bumps where severe acne damaged the underlying skin structure, those are true scars. They don't fade with time. They don't respond to vitamin C serum. They require professional treatment, and even then, the goal is usually improvement, not complete elimination.
Using scar treatments on marks is wasting money. Using mark treatments on scars is wasting time. So let's get specific about what each one looks like and what actually works.
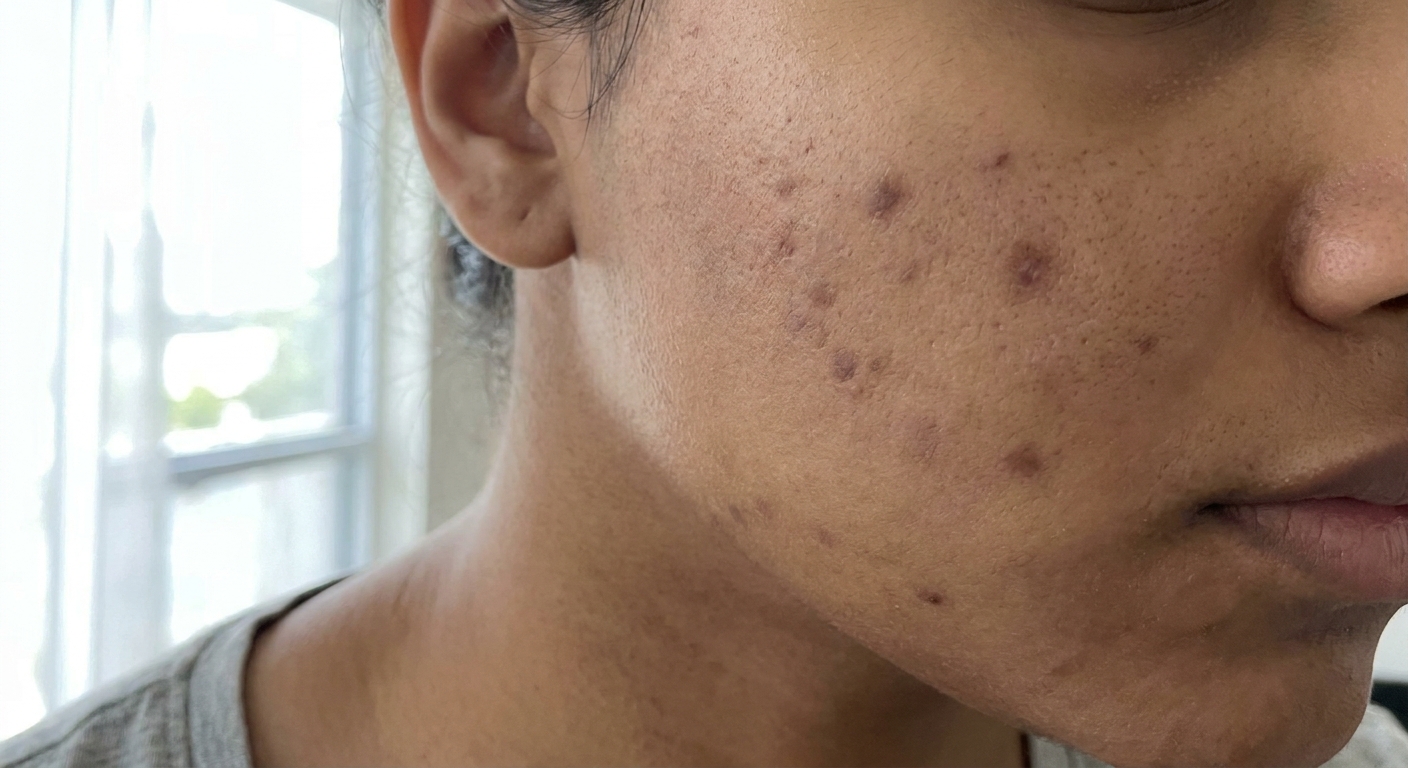
Post-inflammatory hyperpigmentation (PIH): the dark marks
PIH is the most common type of post-acne mark. It shows up as flat, darkened patches at the site of a former pimple. The color can range from light brown to deep purple-brown, depending on your skin tone. People with darker skin tones tend to develop more noticeable PIH, and it tends to last longer.
Here's what's happening underneath: when your skin is inflamed from a pimple, the inflammation triggers melanocytes (pigment-producing cells) to overproduce melanin as part of the healing response. Once the pimple heals, the excess melanin lingers in the skin, creating a dark spot. It's flat. It's smooth. If you run your finger over it, it feels exactly like the surrounding skin. There's no dip, no bump, no texture change.
How long PIH lasts: typically 3 to 12 months, sometimes longer for deeper marks or darker skin tones. It does eventually fade on its own, even without treatment.
What speeds up fading:
-
Sunscreen, every single day. I cannot overstate this. UV exposure stimulates melanocytes to produce even more melanin, which darkens existing PIH and can extend the fading timeline from months to years. SPF 30 or higher, broad spectrum, applied to your face every morning whether or not you plan to be outside. This is the most important thing you can do.
-
Niacinamide (vitamin B3). A solid body of research supports niacinamide for reducing hyperpigmentation. A concentration of 4-5% applied once or twice daily can noticeably speed up fading. It also helps regulate oil production, which is a nice bonus for acne-prone skin. You can find it in serums and moisturizers at every price point.
-
Vitamin C (L-ascorbic acid). Vitamin C inhibits tyrosinase, the enzyme involved in melanin production. It works, but it's finicky. Vitamin C serums oxidize quickly when exposed to air and light, which makes them less effective. Look for products in opaque, air-restricted packaging and use them in the morning under sunscreen.
-
Alpha hydroxy acids (AHAs). Glycolic acid and lactic acid increase cell turnover, helping the pigmented cells shed faster. Start with a low concentration (5-8%) a few times per week. Don't combine AHAs with retinoids on the same night unless you enjoy having a raw, irritated face.
-
Retinoids. Tretinoin, adapalene, and over the counter retinol all speed up cell turnover and help fade PIH. If you're already using a retinoid for acne, it's doing double duty.
What doesn't work on PIH: picking at it, exfoliating aggressively, lemon juice, toothpaste, or any other home remedy you've seen on TikTok. Harsh treatment on hyperpigmented areas can trigger more inflammation, which triggers more melanin production, which makes the dark spot darker. Leave it alone and let your treatments work.
Post-inflammatory erythema (PIE): the red marks
PIE is trickier. These are flat, red or pinkish-purple marks that appear where inflamed pimples used to be. They're most visible on lighter skin tones, where they can look almost like small bruises or wine stains.
PIE is not a pigmentation issue. It's a vascular one. During inflammation, blood vessels in the dermis dilate and sometimes get damaged. After the pimple heals, those dilated or damaged capillaries remain visible through the skin, creating the red mark. If you press on a PIE mark with a clear glass slide (this is called diascopy), it temporarily blanches or fades, because you're pushing the blood out of those superficial vessels. PIH marks don't blanch.
How long PIE lasts: this is the frustrating part. PIE can take 6 months to 2+ years to fully resolve. It fades very slowly as the damaged capillaries heal and the inflammation fully subsides.
What helps PIE:
- Sunscreen. Again. UV exposure worsens PIE and slows healing. Same rules as above.
- Azelaic acid. Has both anti-inflammatory and mild skin-brightening properties. Available over the counter at 10% or by prescription at 15-20%.
- Niacinamide. Helps with the inflammation component, though it doesn't directly target the vascular damage.
- Time. Honestly, this is the main treatment. Most PIE marks fade significantly within 12-18 months with consistent sunscreen use.
What helps PIE if you can see a dermatologist: Pulsed dye laser (PDL) and certain vascular lasers are the most effective treatments for stubborn PIE. They target the dilated blood vessels directly. These are professional treatments, not something you can replicate at home.
What doesn't help PIE: most of the ingredients that work for PIH (vitamin C, AHAs, aggressive exfoliation) don't do much for PIE specifically because it's a vascular problem, not a pigment problem. You won't make it worse by using them, but you shouldn't expect dramatic improvement.
True acne scars: texture changes that stay
This is where the word "scar" is actually accurate.
True acne scars happen when severe inflammation destroys collagen in the dermis. The skin can't fully rebuild the tissue it lost, so the surface changes permanently. Unlike marks, scars involve actual structural damage.
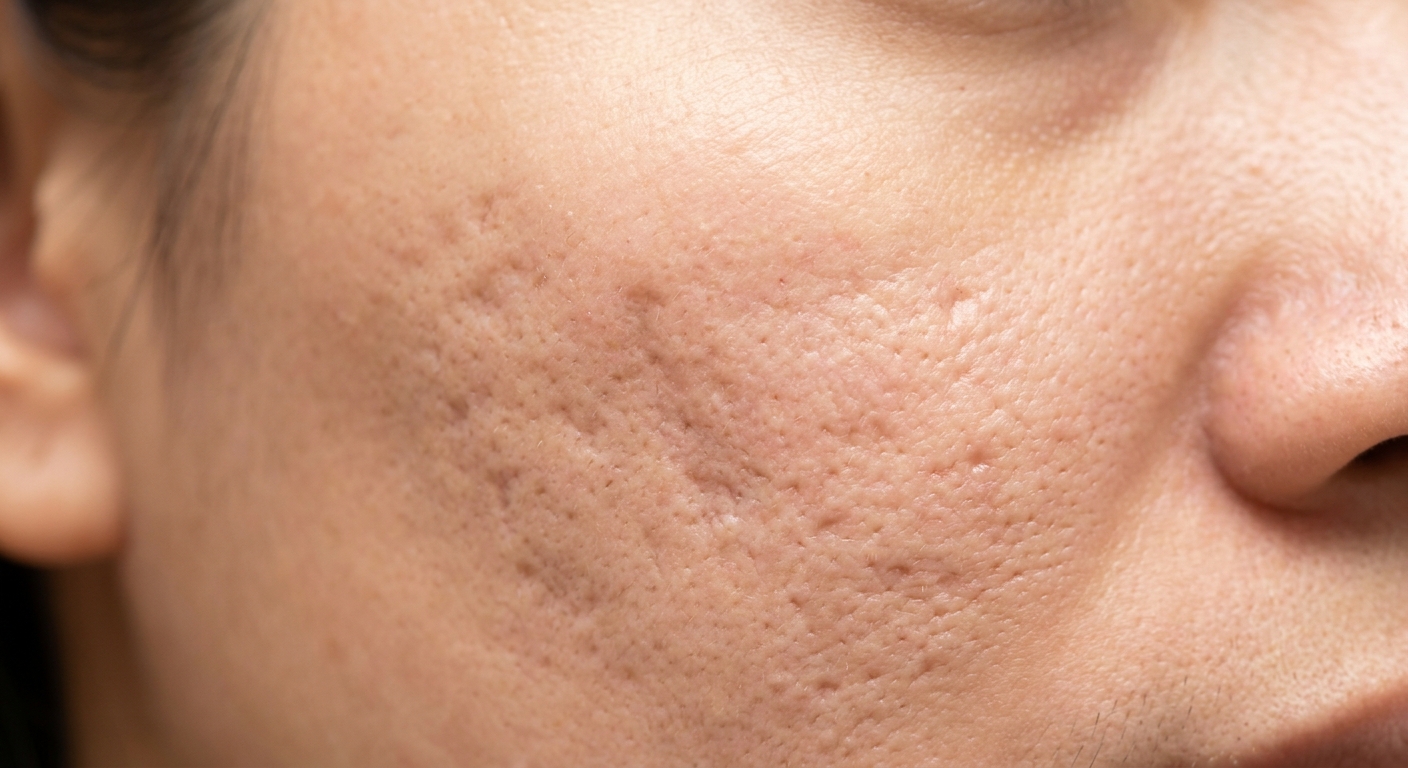
There are three main types of atrophic (indented) acne scars:
Ice pick scars are narrow, deep, V-shaped indentations. They're usually less than 2mm wide but extend deep into the dermis. They look like the skin was punctured with a sharp instrument. These are the hardest type to treat because the damage extends so far down.
Boxcar scars are wider, with well-defined vertical edges. Think of a round or oval depression with sharp borders. They can be shallow (0.1-0.5mm) or deep (0.5mm+). Shallow boxcar scars respond better to treatment than deep ones.
Rolling scars create a wave-like, undulating appearance on the skin surface. They're caused by fibrous bands that tether the epidermis to deeper structures, pulling the surface down. The borders are less defined than boxcar scars, creating more of a general unevenness.
Some people also develop hypertrophic scars or keloids, which are raised rather than indented. These happen when the body overproduces collagen during healing, creating a thick, elevated area. Hypertrophic scars stay within the boundaries of the original wound. Keloids extend beyond them. Both are more common on the chest, back, and jawline, and more prevalent in darker skin tones.
How to tell what you actually have
The simplest test:
Run your clean fingertip across the area. If the surface feels completely smooth and the only difference is color, it's a mark (PIH or PIE). If you can feel an indentation, a pit, or a raised bump, it's a scar.
Look at it in raking light. Stand next to a window so light hits your face from the side. Marks are invisible in this lighting because they're flat. Scars cast tiny shadows or create visible texture changes.
Press on it. If it's red/pink and temporarily fades when you press a clear surface against it, that's PIE. If it's dark and doesn't change with pressure, that's PIH. If there's texture change regardless of pressure, it's a scar.
Most teens have a mix. A few actual scars from the worst cystic breakouts, surrounded by PIH or PIE marks from more recent, less severe pimples. The good news is that the marks, which are usually the majority of what you're seeing, will fade.
Treating marks at home
For PIH and PIE marks, a straightforward routine handles most of it:
Morning: gentle cleanser, niacinamide serum or vitamin C serum (pick one), moisturizer, SPF 30+ sunscreen. The sunscreen is the most important product in this lineup.
Evening: gentle cleanser, retinoid (adapalene 0.1% is available over the counter in most countries), moisturizer.
That's genuinely it. You don't need ten products. You don't need expensive "dark spot correcting" kits. Consistent sunscreen, one brightening ingredient, and a retinoid will fade PIH marks about as fast as anything can without a prescription.
For PIE marks, swap the vitamin C for azelaic acid if you want something that targets the redness more directly. But honestly, time and sunscreen do most of the work.
Be patient. Marks take weeks to months to visibly fade, even with the right products. Progress is often so gradual that you don't notice it day to day. Taking a photo of your skin each month under the same lighting can help you see change you'd otherwise miss.
When to see a dermatologist
If you have actual scars (texture changes), a dermatologist is worth the visit. This is especially true if:
- You have deep ice pick or boxcar scars that bother you
- Your acne is still active, because treating scars while you're still getting new breakouts is generally not effective
- You have keloid-prone skin
- PIH or PIE marks haven't faded at all after 12+ months with consistent treatment

A dermatologist can assess what types of scars you have, determine which treatments are appropriate for your skin type and age, and set realistic expectations about results.
Professional scar treatments
Most of these are recommended for patients 18 and older, because the skin is still changing during adolescence and some treatments require multiple sessions with significant healing time between them.
Microneedling. Uses tiny needles to create controlled micro-injuries in the skin, stimulating collagen production. Effective for rolling and shallow boxcar scars. Typically requires 3-6 sessions spaced 4-6 weeks apart. Downtime is 2-3 days of redness and peeling. This is one of the more accessible professional treatments in terms of cost and recovery.
Fractional laser resurfacing. Lasers like Fraxel create microscopic columns of thermal damage in the skin, triggering collagen remodeling. Effective for moderate boxcar and rolling scars. More expensive than microneedling, with 3-7 days of downtime per session. Multiple sessions are usually needed.
Chemical peels. Medium-depth peels (like TCA at 25-35%) can improve shallow scars and PIH. Deeper peels address deeper scars but carry higher risk of complications, particularly in darker skin tones. Recovery ranges from a few days to two weeks depending on depth.
Subcision. A needle is inserted under the scar to break the fibrous bands tethering the skin down. Particularly useful for rolling scars. Often combined with microneedling or filler for better results.
Dermal fillers. Injectable fillers (hyaluronic acid) can physically lift depressed scars. Results are temporary, lasting 6-18 months, but the effect is immediate. Some dermatologists use this as a bridge while doing other treatments.
TCA CROSS. High-concentration trichloroacetic acid is applied directly into individual ice pick scars using a toothpick-like applicator. This triggers collagen production at the base of the scar, gradually filling it in from the bottom up. Usually requires 3-6 sessions.
Important caveat for teens: be wary of medspas and aestheticians offering these treatments to minors without dermatologist oversight. Lasers and deep peels carry real risks, including worsening of hyperpigmentation (especially in darker skin tones), scarring, and infection. These should be performed by or under the supervision of a board-certified dermatologist who can assess your skin type and scar type properly.
Bottom line
Most of what you see in the mirror after a breakout heals isn't scarring. It's post-inflammatory marks, either dark (PIH) or red (PIE), and they fade on their own. Sunscreen, niacinamide, and a retinoid will speed that up. True scars involve texture changes you can feel with your fingertip, and those need professional treatment to improve.
The most useful thing you can do right now is figure out which category your post-acne marks fall into. If they're flat and just a different color, take a breath. They're temporary. Protect them from the sun and give them time. If they're textured, get your acne under control first, then talk to a dermatologist about treatment options once you're old enough and your breakouts have stabilized.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973https://pubmed.ncbi.nlm.nih.gov/26897386/
- Fabbrocini G, et al. Acne scars: pathogenesis, classification and treatment. Dermatol Res Pract. 2010;2010:893080https://pubmed.ncbi.nlm.nih.gov/21188218/
- Bae-Harboe YS, Graber EM. Easy as PIE (postinflammatory erythema). J Clin Aesthet Dermatol. 2013;6(9):46-47https://pubmed.ncbi.nlm.nih.gov/24062874/
- Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol. 2010;3(7):20-31https://pubmed.ncbi.nlm.nih.gov/20725554/
- Goodman GJ, Baron JA. Postacne scarring: a qualitative global scarring grading system. Dermatol Surg. 2006;32(12):1458-1466https://pubmed.ncbi.nlm.nih.gov/17199653/
- Zeichner JA, et al. Emerging issues in adult female acne. J Clin Aesthet Dermatol. 2017;10(1):37-46https://pubmed.ncbi.nlm.nih.gov/28210380/
- American Academy of Dermatology. Acne scars: Who gets and causes. 2024https://www.aad.org/public/diseases/acne/derm-treat/scars
- Connolly D, et al. Acne scarring: Pathogenesis, evaluation, and treatment options. J Clin Aesthet Dermatol. 2017;10(9):12-23https://pubmed.ncbi.nlm.nih.gov/29344322/
Read This Next

Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →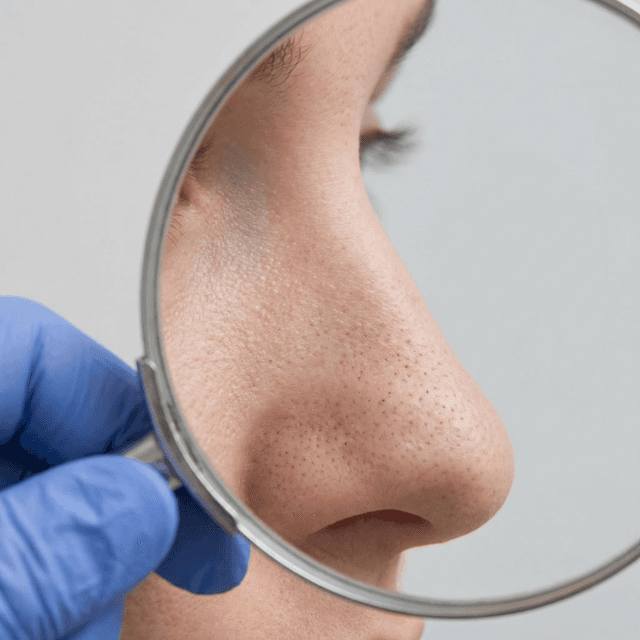
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →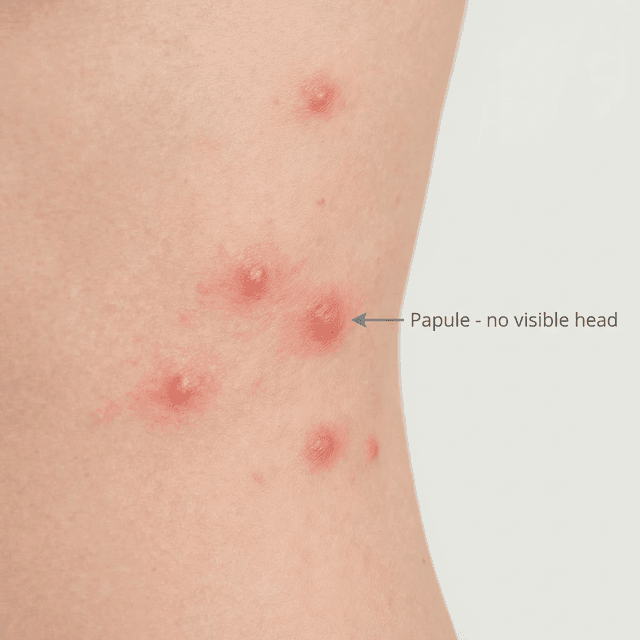
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →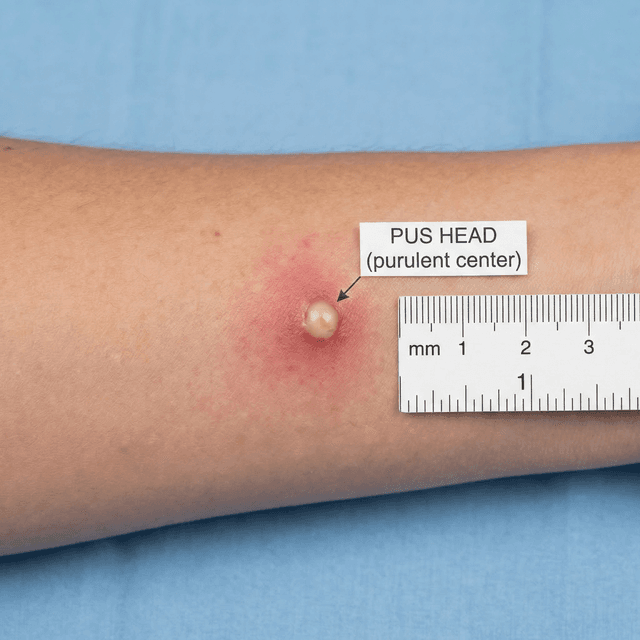
Pustules: The Classic Pimple — What's Inside, Should You Pop It, and How to Treat It
Pustules are what most people picture when they think 'pimple' — red bumps with a white or yellow center. Here's what's actually inside them, whether popping is ever okay, and what dermatologists recommend.
Read More →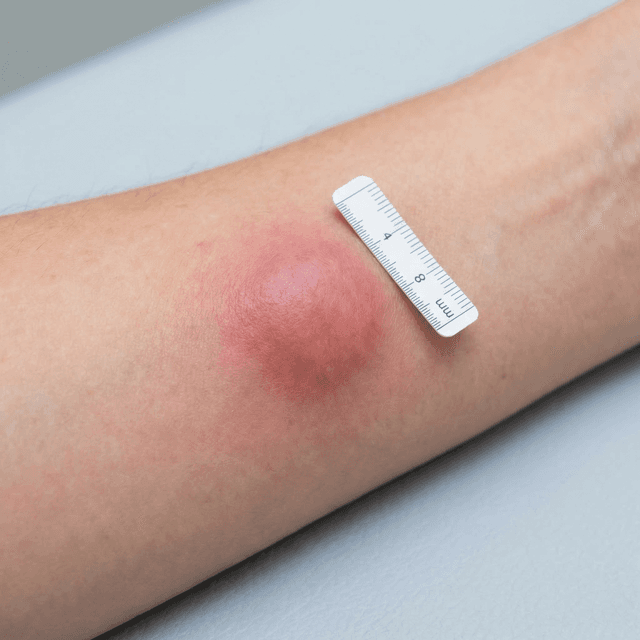
Nodular Acne: Understanding Deep, Painful Acne Bumps and Why They Need Professional Treatment
Hard, painful lumps deep under the skin that won't come to a head? That's nodular acne — a severe form that requires medical treatment. Here's what causes it and what actually works.
Read More →