How to Prevent and Treat Acne Scars: A Complete Guide for Teens
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated March 15, 2026
Key takeaways
- Prevention is everything — treating active acne early and avoiding picking are the two most effective ways to prevent scarring.
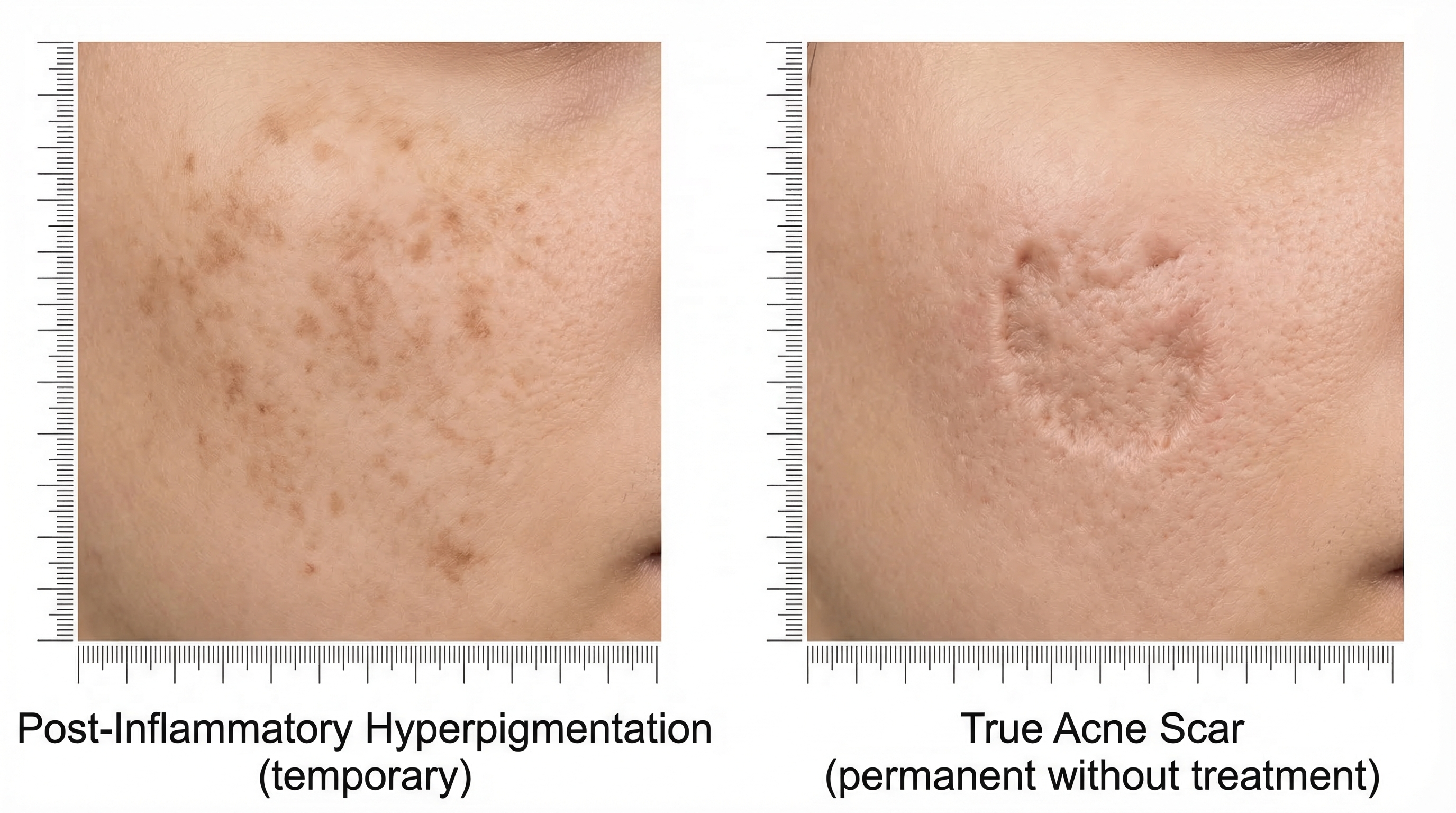
- Dark marks aren't true scars — post-inflammatory hyperpigmentation (PIH) fades on its own over months, while actual scars change the texture of your skin.
- Teen skin heals faster — your age is actually an advantage, since younger skin has more collagen and better healing capacity than adult skin.
- Over-the-counter options exist — retinoids, vitamin C serums, and AHAs can meaningfully improve mild scarring and dark marks at home.
- Professional treatments have limits — procedures like microneedling and laser can improve scars by 30-70%, but rarely eliminate them completely.
If you're a teenager dealing with acne scars — or worried about getting them — you're not alone. Studies estimate that up to 95% of people with acne develop some degree of scarring, and for teens who are already navigating so much socially and emotionally, those marks on your skin can feel like they define you.
They don't. And here's the good news: your age is actually on your side. Teen skin heals faster, produces more collagen, and responds better to treatment than adult skin. Some marks that look permanent right now will fade significantly on their own. Others can be improved with the right approach.
This guide breaks down what acne scars actually are, how to prevent them, and what treatments are realistic when you're young. No hype, no miracle cures — just honest, evidence-based information.
Dark Marks vs. True Scars: What's Actually on Your Skin
Before you panic about "scarring," you need to know an important distinction that most people miss: the dark or reddish spots left behind after a pimple heals are usually not scars at all.
Post-Inflammatory Hyperpigmentation (PIH)
Those flat, dark, or reddish-brown spots that linger after a breakout are called post-inflammatory hyperpigmentation, or PIH. They're caused by your skin's inflammatory response to acne, which triggers excess melanin production. PIH is extremely common in teens and is especially visible on darker skin tones.
The key thing about PIH: it's flat. If you close your eyes and run your finger over the spot, you won't feel any change in texture. That's how you know it's hyperpigmentation and not a true scar.
The even better news? PIH fades on its own. Without any treatment, most dark marks resolve within 3 to 12 months. With the right products (sunscreen, retinoids, vitamin C), you can speed that timeline up significantly.
Post-Inflammatory Erythema (PIE)
If your marks are pink or red rather than brown, you're likely dealing with post-inflammatory erythema (PIE). This is caused by damaged or dilated blood vessels under the skin after inflammation. PIE is more common in lighter skin tones and can be stubborn, sometimes taking 6 to 18 months to fully resolve. It also fades on its own, though vascular lasers can speed the process.
True Acne Scars
True acne scars involve actual changes to the structure and texture of your skin. When you run your finger over them, you can feel depressions or raised areas. These form when severe inflammation damages the collagen in your deeper skin layers, and your body's repair process produces too much or too little tissue.
True scars don't fully resolve on their own, though they do soften and improve over time — especially in young skin that's still producing collagen at a high rate.
Types of Acne Scars
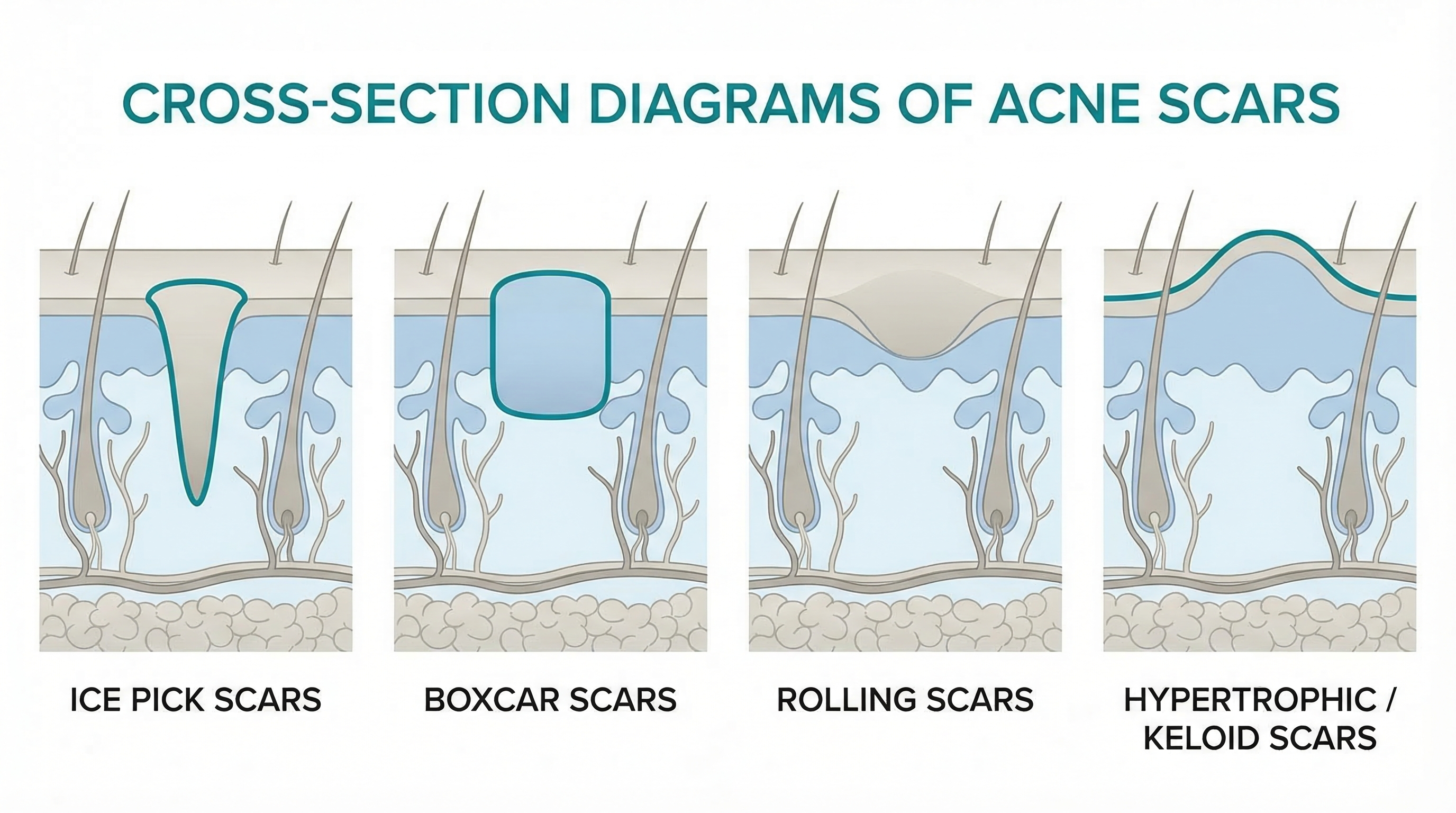
Not all acne scars are the same, and understanding what type you have matters because different scars respond to different treatments. Dermatologists generally classify acne scars into two broad categories: atrophic (depressed) and hypertrophic (raised).
Atrophic (Depressed) Scars
These are by far the most common type of acne scar. They form when inflammation destroys collagen and your skin can't fully rebuild the tissue, leaving a depression or indentation. There are three subtypes:
Ice pick scars are narrow, deep, V-shaped pits that extend into the deeper layers of skin. They look like someone poked your skin with a sharp instrument. Ice pick scars are the most common atrophic scar type and are also the hardest to treat because of their depth. They most often result from inflamed cysts or deep papules.
Boxcar scars are wider, round or oval depressions with sharply defined vertical edges — almost like a shallow crater. Think of them as wider versions of ice pick scars but with a flat bottom instead of a pointed one. They're caused by widespread inflammation that destroys collagen over a broader area.
Rolling scars create a wave-like, uneven texture on the skin. They have sloping, soft edges rather than sharp borders, which gives the skin a rolling or undulating appearance. These form when fibrous bands of scar tissue develop between the skin and the tissue beneath it, pulling the surface down.
Hypertrophic and Keloid Scars
These are raised scars that form when your body produces too much collagen during the healing process.
Hypertrophic scars are raised, firm scars that stay within the boundaries of the original wound. They're more common on the chest, back, and jawline.
Keloid scars are similar but grow beyond the borders of the original breakout, sometimes becoming quite large. Keloids are more common in people with darker skin tones, and they have a genetic component — if your parents get keloids, you're more likely to as well.
Both types can be itchy or tender, and keloids in particular can be challenging to treat.
Why Prevention Beats Treatment Every Time
Here's something every dermatologist will tell you: it's far easier to prevent an acne scar than to treat one. Even the best professional treatments can only improve scarring by an estimated 30 to 70 percent — they rarely eliminate scars completely. That's why prevention is where your effort should go first.
Stop Picking, Squeezing, and Popping
This one is hard. Really hard. When you have a painful, visible pimple, the urge to squeeze it can feel almost impossible to resist. But picking at acne is the single biggest controllable risk factor for scarring.
When you squeeze a pimple, you can rupture the follicle wall beneath the skin's surface, pushing bacteria and debris deeper into the dermis. This causes more inflammation, more tissue damage, and more scarring. A blemish that might have healed cleanly in a week can turn into a scar that lasts years.
Some strategies that help:
- Pimple patches (hydrocolloid bandages) give you something to "do" about a pimple without picking. They absorb fluid and create a barrier that prevents touching.
- Keep your hands busy — this sounds silly, but many people pick at their skin absentmindedly while studying, scrolling, or watching TV.
- Cover your mirrors if you find yourself getting into long picking sessions in the bathroom.
- Talk to someone if picking feels compulsive or out of your control. Skin picking disorder (excoriation disorder) is a recognized condition, and there's no shame in getting help.
Treat Active Acne Early and Consistently
The longer acne goes untreated, the more inflammation builds up, and the greater the risk of scarring. This is especially true for inflammatory acne — red, swollen papules, pustules, nodules, and cysts — rather than blackheads and whiteheads.
If over-the-counter benzoyl peroxide or adapalene isn't getting your acne under control within 2 to 3 months, see a dermatologist. Prescription treatments like topical retinoids, antibiotics, or in severe cases, isotretinoin (Accutane), can prevent the deep inflammation that leads to permanent scarring.
The American Academy of Dermatology specifically recommends early, aggressive treatment for teens with moderate-to-severe acne to minimize scarring risk.
Wear Sunscreen Every Day
UV exposure doesn't cause acne scars, but it makes existing dark marks and scars significantly more visible. Sun exposure stimulates melanin production, which darkens PIH spots and slows the fading process. It also breaks down collagen, which impairs your skin's ability to heal and remodel scar tissue.
Use a broad-spectrum SPF 30 or higher sunscreen daily — even on cloudy days, even in winter. Look for lightweight, non-comedogenic formulas that won't clog pores or feel greasy.

At-Home Treatments That Actually Help
If you already have dark marks or mild scarring, several over-the-counter ingredients have solid evidence behind them. These won't perform miracles, but with consistent use over months, they can make a meaningful difference.
Retinoids (Adapalene / Differin)
Adapalene 0.1% gel is available over the counter and is one of the most well-studied ingredients for both acne treatment and scar improvement. Retinoids work by:
- Accelerating skin cell turnover, which helps fade dark marks faster
- Stimulating collagen production, which can gradually improve the depth of shallow atrophic scars
- Preventing new breakouts, which prevents new scars from forming
Start slowly — every other night — because retinoids can cause dryness and irritation, especially in the first few weeks. Always use sunscreen during the day when using a retinoid, as they increase sun sensitivity.
Vitamin C Serums
Vitamin C (L-ascorbic acid) is an antioxidant that inhibits melanin production and supports collagen synthesis. A 10-15% vitamin C serum applied in the morning can:
- Visibly fade dark marks and PIH over 8 to 12 weeks
- Provide some UV protection (though it's not a substitute for sunscreen)
- Support overall skin healing
Look for serums in opaque, airtight bottles, as vitamin C degrades quickly when exposed to light and air.
Alpha Hydroxy Acids (AHAs)
Glycolic acid and lactic acid are AHAs that gently exfoliate the skin's surface, promoting cell turnover and fading hyperpigmentation. Products containing 5 to 10% glycolic acid can be used a few times per week.
Start with a low concentration and use it at night. AHAs also increase sun sensitivity, so sunscreen is non-negotiable.
Niacinamide
Niacinamide (vitamin B3) at 4-5% concentrations has been shown to reduce hyperpigmentation and strengthen the skin barrier. It's gentle, well-tolerated by most skin types, and plays well with other active ingredients. It's a good option if retinoids or AHAs feel too irritating for your skin.
Silicone Sheets and Gels
For raised scars (hypertrophic or keloid), medical-grade silicone sheets or gels are one of the best-studied at-home treatments. They work by hydrating the scar tissue and creating a protective barrier that helps flatten and soften raised scars over time. You'll need to use them consistently for at least 2 to 3 months to see improvement.
A Realistic At-Home Routine for Scar Fading
Here's what a practical routine might look like:
Morning:
- Gentle cleanser
- Vitamin C serum (optional)
- Lightweight moisturizer with SPF 30+
Night:
- Gentle cleanser
- Adapalene gel (start every other night)
- Moisturizer
Add an AHA exfoliant 1-2 nights per week on the nights you skip adapalene. Don't layer too many actives at once — irritated skin heals more slowly, which defeats the purpose.
Professional Treatments: What's Available
When at-home products aren't enough, dermatologists have a range of procedures that can improve acne scars more significantly. However, there are important things teens need to know before pursuing these options.
Chemical Peels
In-office chemical peels use higher concentrations of acids (glycolic, salicylic, TCA) than what's available over the counter. They remove the outer layers of damaged skin, stimulating new skin growth and collagen production.
- Superficial peels have minimal downtime and can help with PIH and very shallow scars. A series of 4 to 6 peels is usually needed.
- Medium-depth peels (TCA peels) penetrate deeper and can improve moderate scarring, but involve several days of peeling and redness.
Chemical peels are generally considered safe for teens and are one of the more affordable professional options.
Microneedling
Microneedling uses a device with tiny needles to create controlled micro-injuries in the skin, triggering your body's wound-healing response and boosting collagen production. It's effective for rolling and boxcar scars and is generally well-tolerated.
Most people need 3 to 6 sessions spaced 4 to 6 weeks apart. Results develop gradually over months as new collagen forms. Studies show an average improvement of 30 to 50% in scar depth after a full course of treatment.
Important: At-home dermarollers are not the same as professional microneedling. Consumer devices use shorter needles and can actually cause damage or infection if used improperly. Stick to professional treatments.
Laser Treatments
Laser treatments come in two main categories:
Fractional non-ablative lasers (like Fraxel) create microscopic columns of heat in the deeper skin layers without damaging the surface. They stimulate collagen remodeling with less downtime than ablative lasers. Multiple sessions are needed.
Fractional ablative lasers (like CO2 or erbium lasers) remove thin layers of skin and stimulate deeper collagen remodeling. They're more effective but involve more downtime — typically 5 to 7 days of redness and peeling.
Laser treatments can improve scars by 40 to 70% over a series of sessions, depending on scar type and severity. However, they carry risks including hyperpigmentation (especially in darker skin tones), prolonged redness, and in rare cases, worsening of scars. A qualified, experienced dermatologist is essential.
Dermal Fillers
For deep, individual atrophic scars, dermal fillers (like hyaluronic acid) can be injected beneath the scar to lift the depressed area and create a smoother surface. Results are immediate but temporary — most fillers last 6 to 18 months before the body absorbs them.
Fillers are best suited for a small number of well-defined rolling or boxcar scars rather than widespread scarring.
Subcision
Subcision is a minor surgical procedure where a needle is inserted under the skin to break up the fibrous bands that tether rolling scars to deeper tissue. Once these bands are released, the skin can spring back up to a more even level. Subcision is often combined with fillers or microneedling for better results.
TCA Cross
For deep ice pick scars specifically, TCA (trichloroacetic acid) cross involves applying a high concentration of TCA directly into individual scars using a toothpick or small applicator. This triggers collagen production from the bottom of the scar up, gradually raising the depressed area. Multiple sessions are usually needed, spaced 4 to 6 weeks apart.
What's Realistic for Teens
Let's be honest about expectations — because unrealistic expectations lead to frustration and wasted money.
The Good News
- Your skin is on your side. Teen skin produces collagen at a much higher rate than adult skin, which means your scars are actively remodeling and improving on their own. Many shallow scars and most dark marks will improve significantly within 1 to 2 years even without aggressive treatment.
- Early intervention works. Treating acne now, before scarring gets worse, is the most impactful thing you can do.
- Technology keeps improving. Scar treatments are better than they were even 5 years ago, and they'll continue to improve.
The Honest Truth
- No treatment eliminates scars completely. Even the best procedures improve scars — they don't erase them. Anyone promising "complete scar removal" is overpromising.
- Most professional treatments work best after acne is controlled. There's limited benefit to treating scars while you're still actively breaking out, since new breakouts create new scars. Get the acne under control first.
- Many dermatologists recommend waiting. Because teen skin is still healing and changing, some dermatologists prefer to wait until acne has been clear for 6 to 12 months and scars have had time to mature before recommending aggressive procedures like laser treatments.
- Results take time. Whether you're using retinoids at home or getting microneedling in an office, meaningful improvement happens over months, not days.
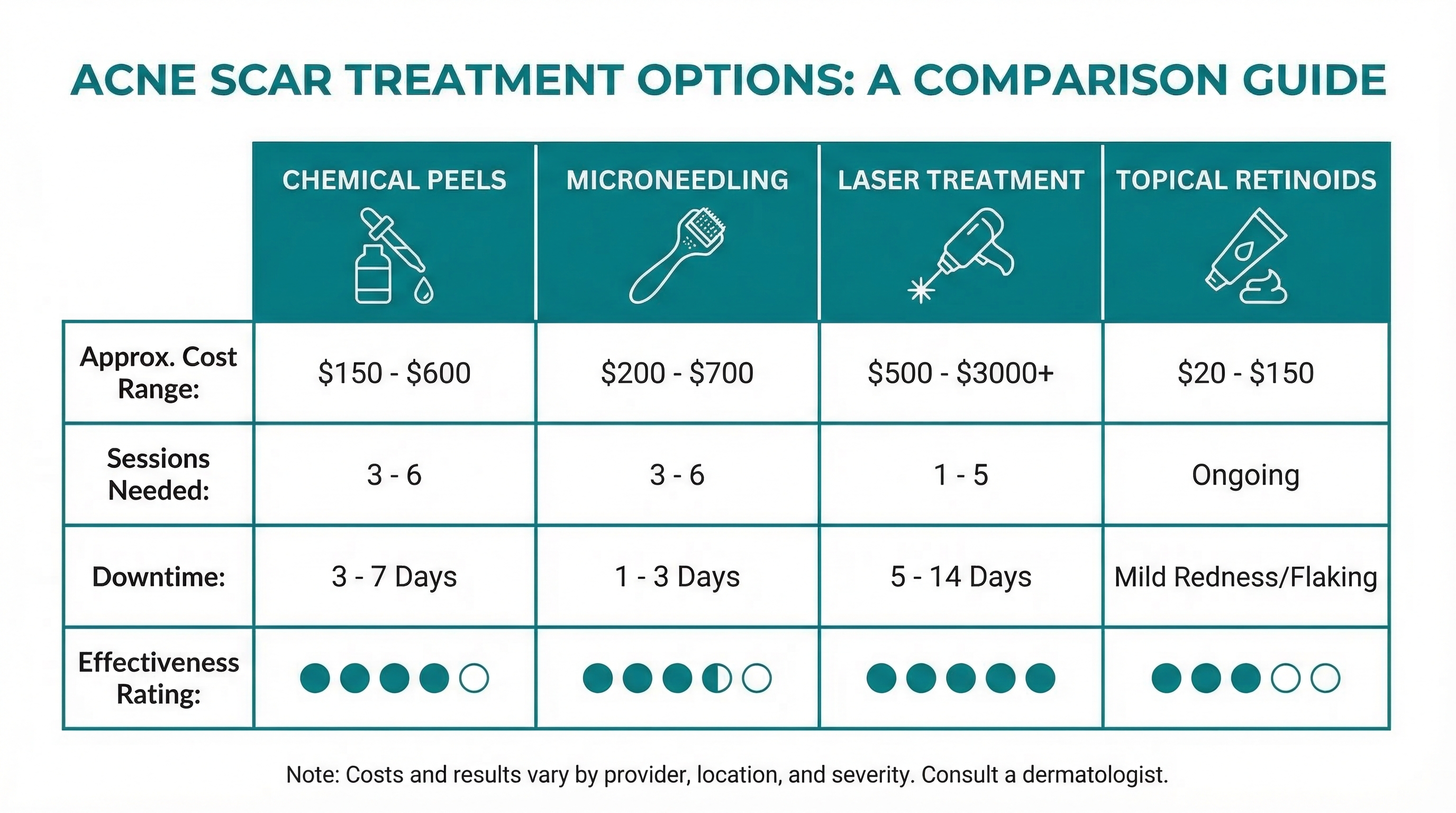
Cost Considerations
Professional scar treatments can be expensive, and most are considered cosmetic, meaning insurance typically won't cover them.
- Chemical peels: $100-$300 per session (4-6 sessions typical)
- Microneedling: $200-$700 per session (3-6 sessions typical)
- Laser treatments: $500-$3,000+ per session (2-5 sessions typical)
- Fillers: $500-$1,500 per session (repeat every 6-18 months)
These costs add up quickly. For most teens, the smartest approach is to focus on prevention, use effective at-home products, and consider professional treatments later if needed — once acne is fully controlled and you've given your skin time to heal naturally.
The Emotional Side of Acne Scars
We'd be doing you a disservice if we only talked about the physical side of acne scars. The emotional impact is real, and it matters.
Research consistently shows that acne scarring is associated with lower self-esteem, increased anxiety, social withdrawal, and even depression — particularly in adolescents. If you're feeling self-conscious about your scars, if you're avoiding social situations, or if your scars are affecting your mental health, that's completely valid. You're not being vain or overdramatic.
A few things worth knowing:
- Other people notice your scars far less than you do. This isn't just a feel-good platitude — it's well-documented in psychology. We fixate on our own perceived flaws far more intensely than anyone else does.
- Scars fade with time. What feels overwhelming at 15 often looks very different at 20 or 25, as your skin continues to heal and remodel.
- It's okay to want treatment. Wanting clear skin isn't shallow. Taking care of your appearance is a normal, healthy part of self-care.
- It's also okay to not pursue treatment. Some people reach a point of acceptance with their scars, and that's equally valid.
- Talk to someone if you're struggling. A parent, school counselor, therapist, or your dermatologist can help if acne scars are significantly affecting your daily life or mental health.
Tip for parents: If your teen is distressed about acne scars, take it seriously. Dismissing their concerns with "it's just acne" or "you'll grow out of it" can feel invalidating. Helping them see a dermatologist isn't indulging vanity — it's supporting their wellbeing.
Bottom Line
Acne scars can feel overwhelming when you're a teenager, but there's a lot you can do — and the most important steps are the simplest ones.
Prevent new scars by treating active acne early, resisting the urge to pick, and wearing sunscreen daily. Fade dark marks with over-the-counter retinoids, vitamin C, and patience — most hyperpigmentation resolves on its own within months. Give your skin time before pursuing expensive professional treatments; teen skin heals remarkably well, and many scars that seem permanent at 15 are far less noticeable by your early 20s.
If your scars are deep, widespread, or causing significant emotional distress, a board-certified dermatologist can create a treatment plan tailored to your specific scar types and skin tone. But even in those cases, improvement is a gradual process — not an overnight fix.
You're dealing with something hard, and it's okay to feel frustrated by it. But your skin is healing, even when it doesn't feel like it.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Fabbrocini G, et al. Acne scars: pathogenesis, classification and treatment. Dermatol Res Pract. 2010;2010:893080https://pubmed.ncbi.nlm.nih.gov/21188228/
- American Academy of Dermatology. Acne scars: Diagnosis and treatment. 2024https://www.aad.org/public/diseases/acne/derm-treat/scars
- Connolly D, et al. Acne Scarring — Pathogenesis, Evaluation, and Treatment Options. J Clin Aesthet Dermatol. 2017;10(9):12-23https://pubmed.ncbi.nlm.nih.gov/29344322/
- Zaenglein AL, et al. Guidelines of care for the management of acne vulgaris. J Am Acad Dermatol. 2016;74(5):945-973https://pubmed.ncbi.nlm.nih.gov/26897386/
- Eichenfield LF, et al. Evidence-based recommendations for the diagnosis and treatment of pediatric acne. Pediatrics. 2013;131 Suppl 3:S163-86https://pubmed.ncbi.nlm.nih.gov/23637225/
- Oge LK, et al. Acne Vulgaris: Diagnosis and Treatment. Am Fam Physician. 2019;100(8):475-484https://pubmed.ncbi.nlm.nih.gov/31613567/
- Tan J, et al. Acne and Scarring: Epidemiology, Pathophysiology, and Prevention. J Cutan Med Surg. 2022;26(2 Suppl):3S-7Shttps://pubmed.ncbi.nlm.nih.gov/35678089/
- Abdel Hay R, et al. Interventions for acne scars. Cochrane Database Syst Rev. 2016;4(4):CD011946https://pubmed.ncbi.nlm.nih.gov/27038134/
- Boen M, Jacob C. A Review and Update of Treatment Options Using the Acne Scar Classification System. Dermatol Surg. 2019;45(3):411-422https://pubmed.ncbi.nlm.nih.gov/30608264/
- Skin Cancer Foundation. Sunscreen and Sun Protection. 2024https://www.skincancer.org/skin-cancer-prevention/sun-protection/
- Layton AM, et al. A review on the treatment of acne scarring — Where do we stand? J Cosmet Dermatol. 2021;20(4):1065-1071https://pubmed.ncbi.nlm.nih.gov/33559964/
Read This Next

How to Get Rid of Chest Acne: What Works and What Doesn't
Read More →
How to Fade Acne Marks and Dark Spots: Realistic Timelines
Read More →
How to Get Rid of Forehead Acne: Causes and Fixes

Skincare Routine for Teens with Oily Skin: Morning and Night
