How to Fade Acne Marks and Dark Spots: Realistic Timelines
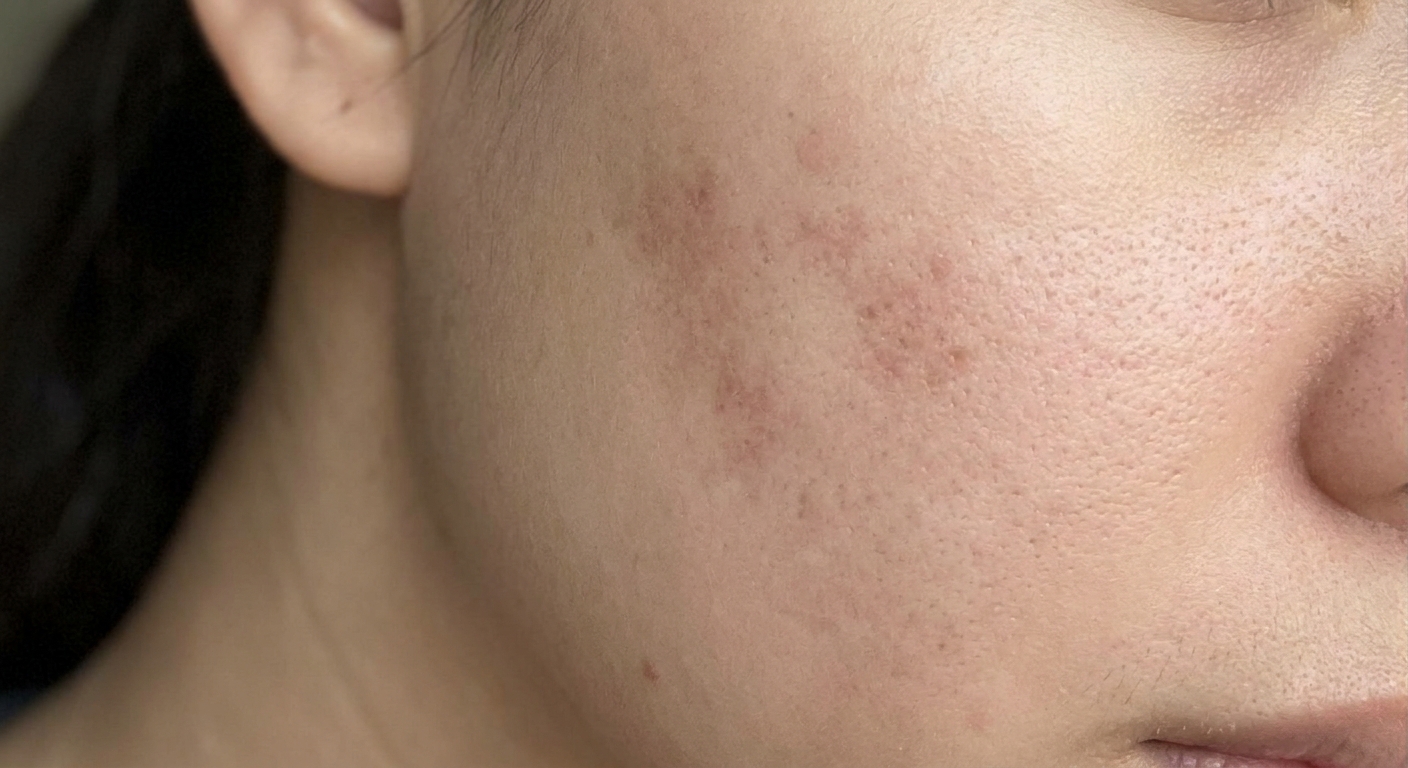
The pimple is gone but the mark it left behind might bother you more than the breakout itself did. That flat, dark or reddish spot staring back at you in the mirror every morning, sometimes for months after the actual acne has healed. I think the worst part is the uncertainty. Will this fade? When? Is this permanent?
I'm going to give you honest answers. Some of them are frustrating. The good news is that most acne marks do fade on their own. The bad news is that "on their own" means months, not days, and the products that promise fast results are mostly lying to you.
Marks vs. Scars: This Distinction Matters
Before anything else, you need to figure out what you're actually dealing with. Acne marks and acne scars are different things, and the difference determines everything about your treatment approach.
Acne marks (post-inflammatory hyperpigmentation or post-inflammatory erythema) are flat changes in skin color left behind after a breakout heals. They're discoloration, not texture changes. If you run your finger over them, the skin is smooth. These are temporary, even though "temporary" in skin terms can mean 3 to 12 months or occasionally longer.
Acne scars are actual changes in skin texture. Ice pick scars (narrow, deep pits), boxcar scars (wider depressions with defined edges), rolling scars (shallow, wavy indentations), and hypertrophic or keloid scars (raised bumps of scar tissue). These are structural damage to the dermis, and they don't fade on their own. They require professional treatment.
Most teens are dealing with marks, not scars. That's good. But if you have textural changes, skip to the section at the end about seeing a dermatologist, because no over-the-counter product is going to fix a true scar.
PIH vs. PIE: Two Types of Marks
Dermatologists distinguish between two types of flat acne marks, and knowing which one you have changes what treatments will help.
Post-inflammatory hyperpigmentation (PIH) appears as brown, dark brown, or grayish patches. It's caused by excess melanin production triggered by the inflammation from a breakout. PIH is more common and more severe in darker skin tones (Fitzpatrick types III through VI) because there's more melanin in the skin to begin with. A study in the Journal of Clinical and Aesthetic Dermatology found that PIH was the primary reason for dermatology visits among people of color, more so than the acne itself (Davis & Callender, 2010).
Post-inflammatory erythema (PIE) appears as flat pink, red, or purple spots. It's caused by damaged or dilated blood vessels under the skin surface. PIE is more visible on lighter skin tones. An easy way to distinguish PIE from PIH: press a clear glass against the mark. If it fades or disappears when you press, it's PIE (vascular). If it stays dark, it's PIH (pigment).
This matters because the treatments that target excess melanin (PIH) don't necessarily work on damaged blood vessels (PIE), and vice versa.
Realistic Timelines
I want to set expectations clearly because the internet is full of "fade dark spots in 7 days" content that sets people up for disappointment.
PIE (red/pink marks):
- Mild cases: 3 to 6 months to fade significantly
- Moderate cases: 6 to 12 months
- Stubborn cases: up to 18 months
- With treatment: you can potentially cut these timelines by 30-40%
PIH (brown/dark marks):
- On lighter skin: 3 to 6 months
- On medium skin tones: 6 to 12 months
- On darker skin tones: 6 to 24 months
- With treatment: again, roughly 30-40% faster, but not overnight
These numbers come from clinical experience and published literature on post-inflammatory pigmentation (Callender et al., 2011). I know they're not what you want to hear. But I'd rather give you real timelines than false hope, because false hope leads to product-hopping and wasted money.
Sunscreen Is the Number One Tool
This is not hyperbole. If you do nothing else on this list, wear sunscreen on your face every single day. SPF 30 minimum, applied to all areas with marks, rain or shine.
UV exposure directly stimulates melanocytes to produce more melanin. If you have PIH and you're walking around without sunscreen, every minute of sun exposure is actively making your dark marks darker and prolonging the time they take to fade. A study published in Pigment Cell and Melanoma Research demonstrated that UV radiation significantly worsened post-inflammatory hyperpigmentation even at sub-erythemal doses, meaning doses that don't cause a visible sunburn (Mahmoud et al., 2010).
For PIE, sunscreen is slightly less directly relevant but still helps prevent additional inflammation and damage to healing skin.
Specific sunscreen advice for acne-prone skin:
- Look for "non-comedogenic" on the label. Oil-free formulas are generally safer for acne-prone skin.
- Mineral sunscreens (zinc oxide, titanium dioxide) are less likely to irritate sensitive post-acne skin than chemical sunscreens. The downside is white cast, especially on darker skin tones.
- Newer tinted mineral sunscreens contain iron oxides that also block visible light, which can trigger pigmentation in darker skin tones. EltaMD UV Clear, La Roche-Posay Anthelios, and Australian Gold Botanical are all reasonable options.
- Reapply every 2 hours if you're outdoors. Most people apply sunscreen once and forget about it.

Treatments That Actually Work for PIH (Dark Marks)
Niacinamide (vitamin B3) at 4-5% concentration is one of my favorite recommendations for teens. It inhibits melanosome transfer from melanocytes to keratinocytes, which in plain language means it slows down the process that makes dark marks darker. A randomized controlled trial showed that 4% niacinamide significantly reduced hyperpigmentation after 8 weeks of use (Hakozaki et al., 2002). It's also anti-inflammatory, well-tolerated, and cheap. The Ordinary Niacinamide 10% + Zinc 1% is probably the most popular option, though I think 10% is more than necessary. CeraVe PM Moisturizing Lotion contains 4% niacinamide built into a moisturizer, which simplifies your routine.
Vitamin C (L-ascorbic acid) at 10-20% concentration is an antioxidant that also inhibits tyrosinase, the enzyme responsible for melanin production. The evidence for vitamin C in treating PIH is solid (Al-Niaimi & Chiang, 2017). The catch is that L-ascorbic acid is notoriously unstable. It oxidizes when exposed to air and light, turning the product brown and useless. If your vitamin C serum is dark brown or orange, it's gone bad. Look for products in opaque, airtight packaging. Skinceuticals CE Ferulic is the gold standard but costs $180. Timeless Vitamin C + E Ferulic is a more affordable alternative with a similar formulation.
Azelaic acid at 10-20% is an underrated option. It's available over the counter at 10% (The Ordinary Azelaic Acid Suspension 10%) and by prescription at 15-20%. It works on PIH by inhibiting tyrosinase and has additional anti-inflammatory and antibacterial properties. A study found that 20% azelaic acid was comparable to 4% hydroquinone for treating melasma, with fewer side effects (Balina & Graupe, 1991). I particularly like azelaic acid because it treats active acne and dark marks simultaneously.
Retinoids (adapalene, tretinoin, retinol) speed up cell turnover, which means the pigmented skin cells are shed and replaced faster. Adapalene 0.1% (Differin) is available over the counter and has shown efficacy in reducing PIH in clinical studies (Jacyk et al., 2011). Prescription-strength tretinoin is more effective but also more irritating. Start slow with retinoids: every other night for the first few weeks, building up to nightly use. And always use sunscreen when using retinoids because they make your skin photosensitive.
Alpha hydroxy acids (AHAs) like glycolic acid and lactic acid exfoliate the surface of the skin, helping to remove pigmented cells. Products containing 5-10% glycolic acid used 2-3 times a week can help fade PIH. Don't go overboard with chemical exfoliants. More is not better, and over-exfoliation can actually trigger more inflammation and more PIH, especially in darker skin tones.
Treatments for PIE (Red/Pink Marks)
PIE is harder to treat topically because the problem isn't pigment but rather damaged capillaries under the skin. Options are more limited:
Niacinamide helps here too by reducing inflammation and strengthening the skin barrier. It's probably the single best over-the-counter ingredient for PIE.
Azelaic acid also has some benefit for PIE through its anti-inflammatory properties.
Centella asiatica (cica) extracts have some evidence for supporting skin healing and reducing redness. They won't dramatically accelerate PIE fading, but they're gentle and won't make anything worse.
What actually works well for PIE is professional treatments: pulsed dye laser (PDL) and vascular lasers can target the dilated blood vessels directly. If you have stubborn PIE that hasn't faded after 6 months of good skincare and sunscreen, a dermatologist consultation for laser treatment is reasonable.
What Doesn't Work
"Scar removal" creams. Products marketed as scar removers (Mederma, Bio-Oil, various "scar gels") have weak to no evidence for treating either acne marks or acne scars. A Cochrane review found insufficient evidence to support the use of silicone gel sheeting for hypertrophic scars, and the evidence for scar creams on flat marks is even thinner (O'Brien & Jones, 2013). Save your money.
Lemon juice. The internet loves recommending lemon juice for dark spots. It's acidic enough to irritate your skin and potentially cause chemical burns, and the psoralen compounds in citrus can cause severe photosensitive reactions. This is a terrible idea. Please don't put lemon juice on your face.
Toothpaste, baking soda, apple cider vinegar. None of these have any evidence for treating PIH or PIE. They can all irritate your skin and potentially make marks worse.
Dermabrasion kits and aggressive scrubbing. Physical exfoliation with harsh scrubs or at-home dermabrasion tools can trigger more inflammation, which leads to more PIH. Gentle chemical exfoliation is better than physical scrubbing for post-acne marks.
Why Darker Skin Tones Get Worse PIH
This needs to be addressed directly because most acne articles are written as if everyone has the same skin, and that's not the case.
Melanocytes in darker skin are more reactive to inflammation. When a pimple heals, the inflammatory response triggers melanocytes to overproduce melanin as a protective response, and this reaction is more pronounced in skin with more baseline melanin. The result is that a breakout that might leave a faint pink mark on lighter skin can leave a dark brown mark that persists for a year or more on darker skin.
This also means that some treatments need to be used more carefully. High-concentration chemical peels, aggressive retinoid use, and certain laser treatments carry a risk of making PIH worse in darker skin tones if they cause irritation or inflammation. The approach should be more gradual: lower concentrations, slower introduction of actives, and close monitoring for irritation.
Azelaic acid and niacinamide are particularly good choices for darker skin because they're effective without being irritating. Hydroquinone at 2% (available over the counter in the US) is the gold standard prescription ingredient for PIH and works across all skin tones, but I'd recommend using it under dermatologist supervision, especially for teens, because long-term unsupervised use can cause a condition called ochronosis (paradoxical darkening).
When to See a Dermatologist
Book an appointment if:
- Your marks haven't improved at all after 6 months of consistent treatment with sunscreen plus one or two active ingredients
- You have actual textural scars (indentations, raised bumps), not just discoloration
- You have dark skin and your PIH is getting worse despite treatment
- You're considering professional treatments like chemical peels or laser therapy
- Your acne is still active, meaning you're getting new breakouts that create new marks faster than old ones fade
A dermatologist can offer prescription-strength retinoids, higher-concentration azelaic acid, hydroquinone, professional chemical peels (glycolic, salicylic, TCA), microneedling, and laser treatments. For true acne scars, procedures like subcision, fractional laser resurfacing, and filler injections are options, but these are typically reserved for people over 18 whose acne is fully under control.
Key Takeaways
- Most acne "marks" are flat discoloration (PIH or PIE), not scars. They will fade, but it takes months. Set your expectations at 3-12 months, not days.
- Sunscreen every day is the most impactful single thing you can do. UV exposure actively darkens PIH and slows healing. SPF 30+, rain or shine.
- Niacinamide and azelaic acid are the best starting ingredients for most teens: effective, affordable, gentle, and they work on both active acne and marks.
- "Scar removal" products are mostly marketing. Mederma, Bio-Oil, and similar products don't have strong evidence behind them for acne marks.
- Darker skin tones need a more careful, gradual approach because aggressive treatments can trigger more PIH. Stick with gentle actives and see a dermatologist sooner rather than later.
The Bottom Line
Fading acne marks is a patience game, and that's genuinely hard to accept when you're 15 and the mark from a breakout two months ago is still clearly visible. The most effective approach is boring and slow: daily sunscreen, one or two well-chosen active ingredients used consistently, and time. Products that promise fast results are either lying or using ingredients harsh enough to potentially backfire. Protect your skin from the sun, use niacinamide or azelaic acid, keep treating any active acne so you stop creating new marks, and give it a few months. If that's not working, a dermatologist has tools that over-the-counter products can't match.
Sources
- Davis, E.C. & Callender, V.D. (2010). Postinflammatory hyperpigmentation: A review of the epidemiology, clinical features, and treatment options in skin of color. Journal of Clinical and Aesthetic Dermatology, 3(7), 20-31.
- Callender, V.D., et al. (2011). Postinflammatory hyperpigmentation. American Journal of Clinical Dermatology, 12(2), 87-99.
- Mahmoud, B.H., et al. (2010). Effects of visible light on the skin. Photochemistry and Photobiology, 86(3), 748-753.
- Hakozaki, T., et al. (2002). The effect of niacinamide on reducing skin pigmentation and suppression of melanosome transfer. British Journal of Dermatology, 147(1), 20-31.
- Al-Niaimi, F. & Chiang, N.Y.Z. (2017). Topical vitamin C and the skin: Mechanisms of action and clinical applications. Journal of Clinical and Aesthetic Dermatology, 10(7), 14-17.
- Balina, L.M. & Graupe, K. (1991). The treatment of melasma: 20% azelaic acid versus 4% hydroquinone cream. International Journal of Dermatology, 30(12), 893-895.
- Jacyk, W.K., et al. (2011). Adapalene gel 0.1% for the treatment of post-inflammatory hyperpigmentation. Journal of the European Academy of Dermatology and Venereology, 25(10), 1208-1213.
- O'Brien, L. & Jones, D.J. (2013). Silicone gel sheeting for preventing and treating hypertrophic and keloid scars. Cochrane Database of Systematic Reviews, 9, CD003826.
- American Academy of Dermatology. (2024). How to fade dark spots in skin of color. Retrieved from https://www.aad.org/public/everyday-care/skin-care-basics/care/fade-dark-spots
- Zaenglein, A.L., et al. (2016). Guidelines of care for the management of acne vulgaris. Journal of the American Academy of Dermatology, 74(5), 945-973.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
Read This Next

The Acne Glossary: Every Term You'll Encounter, Explained Simply
From adapalene to zinc, every acne and skincare term you'll run into, defined in plain language without the medical jargon.
Read More →
Micellar Water for Acne-Prone Skin: Gentle Cleanser or Lazy Shortcut?
Micellar water is fine for light cleansing days but won't remove sunscreen properly. Here's when to use it, when to skip it, and whether you need to rinse.
Read More →
How Seasonal Changes Affect Your Acne (And When to Switch Products)

Going to College with Acne: Preparing Your Skincare for Dorm Life
