Nodular Acne: Understanding Deep, Painful Acne Bumps and Why They Need Professional Treatment
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated March 13, 2026
Key takeaways
- Nodular acne forms deep within the skin — these are hard, painful lumps larger than 5mm that don't have a visible head
- Over-the-counter products cannot effectively treat nodular acne because they can't penetrate deep enough
- Attempting to squeeze or pop nodules causes significantly more damage and almost always leads to scarring
- Prescription treatments like oral antibiotics, hormonal therapy, or isotretinoin are typically necessary
- Early treatment is critical — untreated nodular acne has the highest risk of permanent scarring
If you have ever felt a deep, hard lump forming under your skin — one that throbs with pain but never comes to a head — you already know that nodular acne feels fundamentally different from a regular pimple. That is because it is fundamentally different. Nodular acne is one of the most severe forms of acne, and it develops deep within the dermis where no face wash, scrub, or spot treatment can reach. It is also one of the most emotionally and physically painful skin conditions a teenager can experience.
The hard truth is that nodular acne cannot be managed with over-the-counter products alone. It requires professional medical treatment, and the sooner you see a dermatologist, the better your chances of avoiding permanent scarring. This article will walk you through exactly what nodular acne is, why it happens, what makes it so stubborn, and what treatments dermatologists use to get it under control.
What Is Nodular Acne
Nodular acne is classified as severe acne — the most serious category on the clinical acne grading scale. While a typical pimple develops near the surface of the skin, a nodule forms deep within the dermal layer, well below where topical products can penetrate. The result is a hard, painful lump under the skin that can persist for weeks or even months without proper treatment.
Here is what distinguishes a nodule from other types of acne lesions:
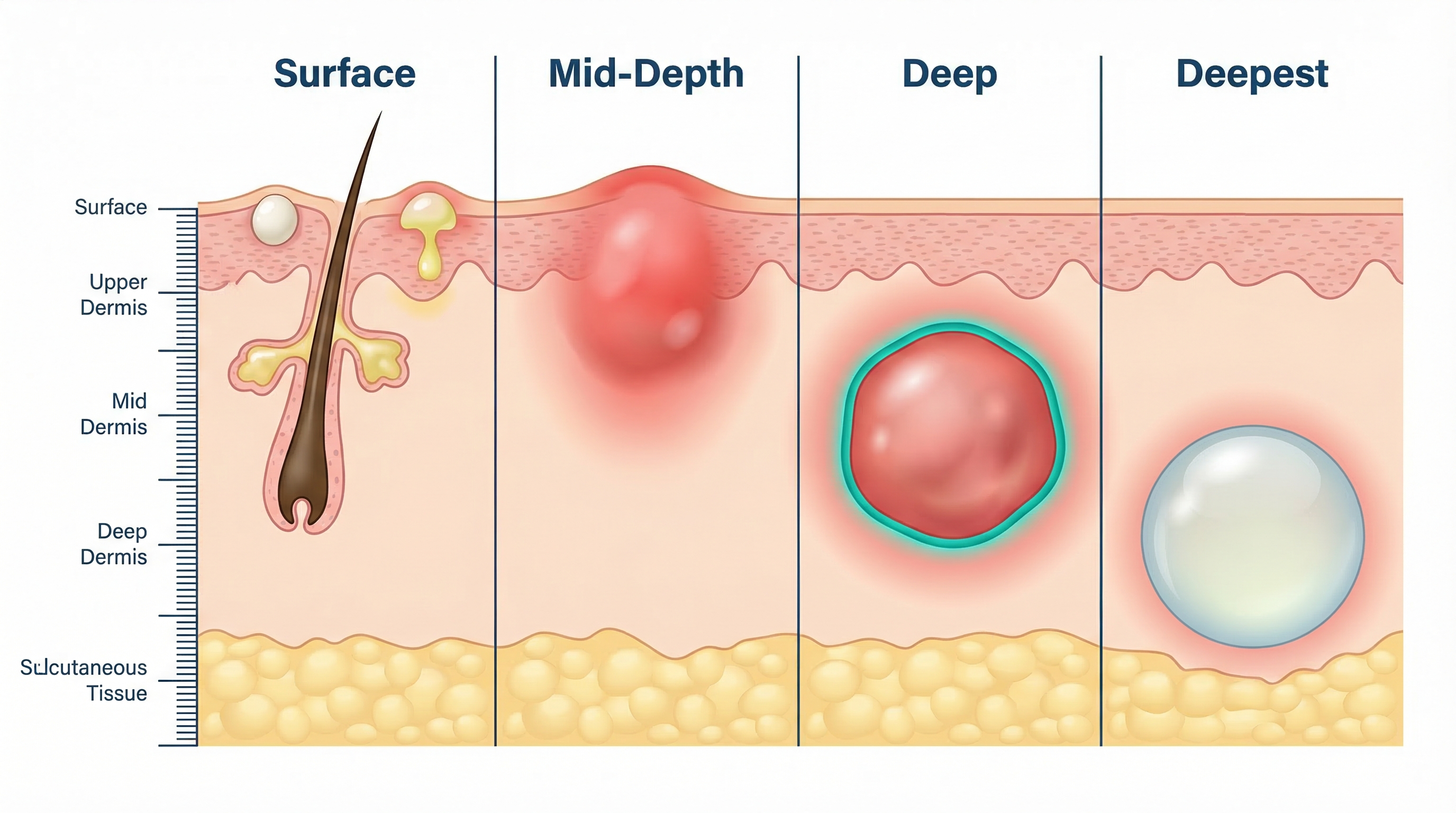
- Size: Nodules are larger than 5mm in diameter — roughly the size of a pencil eraser or bigger. Some can grow significantly larger.
- Depth: They originate deep in the dermis, far below the skin's surface. A typical whitehead or blackhead sits in the upper layers of the skin; a nodule sits much deeper.
- Texture: Nodules feel firm and hard to the touch. Unlike a pustule (which has a soft, fluid-filled center), a nodule feels solid.
- No visible head: There is no whitehead, no pus visible at the surface. The inflammation is entirely below the skin.
- Pain: Nodules are often intensely painful, even without touching them. The deep inflammation puts pressure on surrounding nerve endings.
- Duration: Without treatment, individual nodules can last for weeks to months. They do not resolve on their own timeline the way a surface pimple might.
Dermatologists classify acne severity into four grades. Grade I is mild comedonal acne (blackheads and whiteheads). Grade II is moderate inflammatory acne (papules and pustules). Grade III is severe inflammatory acne with nodules. Grade IV — the most severe — is nodulocystic acne, where both nodules and cysts are present. If you are dealing with hard, painful deep acne bumps, you are in Grade III or IV territory, and that means medical intervention is not optional — it is necessary.
Nodular Acne vs. Cystic Acne: What Is the Difference?
People often use "nodular acne" and "cystic acne" interchangeably, but they are clinically distinct lesions:
- Nodules are solid, hard lumps deep in the skin. They are firm to the touch and do not contain fluid or pus in a central cavity.
- Cysts are also deep, but they contain a semi-liquid or liquid core — a mixture of pus, dead cells, and bacteria enclosed in a sac-like membrane. Cysts tend to feel slightly softer than nodules.
In practice, many teens with severe acne have both nodules and cysts, which is why dermatologists often refer to the condition as nodulocystic acne. Both types carry a high risk of scarring, and both require professional treatment. The distinction matters mainly because it helps your dermatologist tailor the treatment approach.
How Is Nodular Acne Different from Regular Pimples?
A regular papule or pustule — what most people call a "pimple" — develops when a clogged pore becomes mildly to moderately inflamed. The inflammation stays relatively contained near the skin's surface, the lesion runs its course in a few days to a couple of weeks, and it usually resolves without permanent damage.
Nodular acne is a completely different process. The inflammation is deep, intense, and destructive. The body's immune response is so aggressive that it damages the surrounding collagen and tissue, which is why nodules carry such a high risk of leaving permanent scars — even when they are left completely alone and never touched.
How Nodules Form
Understanding the pathophysiology of nodular acne helps explain why it is so resistant to simple treatments and why it behaves so differently from surface-level breakouts.
The Deep Follicular Rupture
All acne begins the same way: a hair follicle becomes clogged with excess sebum (oil) and dead skin cells, creating a microcomedone. In mild acne, this plug stays near the surface and might become a blackhead or whitehead. In moderate acne, bacteria (Cutibacterium acnes) colonize the clogged follicle and trigger a localized inflammatory response, producing a red, swollen papule or pus-filled pustule.
In nodular acne, something more dramatic happens. The wall of the hair follicle ruptures deep within the dermis. When this deep break occurs, the entire contents of the follicle — sebum, dead cells, bacteria, and inflammatory byproducts — spill into the surrounding dermal tissue. This is not a small leak near the surface. It is a deep structural failure that triggers a massive immune response.
The Intense Inflammatory Cascade
When follicular contents breach the dermis, the immune system responds aggressively. Here is what happens at the cellular level:
- Neutrophils flood the area — these are the first-responder immune cells. They rush to the site of the rupture and begin releasing enzymes and reactive oxygen species to fight the bacteria. In the process, they also damage healthy surrounding tissue.
- Macrophages arrive next — these larger immune cells engulf bacteria and debris, but they also release pro-inflammatory cytokines (signaling molecules) that intensify and sustain the inflammation.
- The inflammatory response becomes self-sustaining — cytokines like IL-1, TNF-alpha, and IL-8 recruit even more immune cells. The area becomes a war zone of immune activity, which is why nodules feel so painful and swollen.
- Collagen and tissue damage occurs — the prolonged, intense inflammation damages the collagen matrix and surrounding dermal structures. This tissue destruction is what leads to scarring — and it is happening regardless of whether you touch the nodule or not.
This entire process is driven by the depth of the rupture. Because it occurs in the dermis rather than near the skin's surface, the inflammation is more severe, more sustained, and more destructive. The body essentially walls off the area with inflammatory tissue, creating that characteristic hard, painful lump that you can feel deep beneath your skin.
Why Some Teens Get Nodular Acne and Others Don't
Not every teenager who gets acne will develop nodules. Several factors increase the risk:
- Genetics play the largest role. If one or both parents had severe or nodular acne, you are significantly more likely to develop it. Genetics influence sebum production, pore size, inflammatory response intensity, and how your follicles are structured.
- Androgen levels — higher levels of androgens (particularly DHT) drive greater sebum production, which increases the likelihood of deep follicular clogging and rupture.
- Individual inflammatory response — some people's immune systems mount a more aggressive response to C. acnes bacteria. Research has shown that the intensity of the inflammatory reaction, not just the amount of bacteria, determines acne severity.
- Delayed or inadequate treatment of moderate acne can allow it to progress to the nodular stage. What starts as papules and pustules can evolve into deeper inflammation over time.
Why OTC Products Don't Work
This is one of the most important things to understand about nodular acne, and it is the reason many teens and parents spend months — sometimes years — frustrated with products that do nothing.
The Depth Problem
Over-the-counter acne treatments like benzoyl peroxide, salicylic acid, and adapalene are designed to work in the upper layers of the skin — the epidermis and the very top of the dermis. They are effective for comedonal acne (blackheads and whiteheads) and mild-to-moderate inflammatory acne (papules and small pustules) because those lesions are relatively superficial.
Nodular acne sits far below where these products can penetrate. A 2% salicylic acid wash or a 2.5% benzoyl peroxide gel simply cannot reach the deep dermal inflammation that defines a nodule. It would be like trying to treat a deep tissue infection with a band-aid — the intervention is happening at the wrong level entirely.
What Happens When You Keep Trying OTC
Many teens go through a discouraging cycle:
- A painful deep lump appears.
- They apply a spot treatment — benzoyl peroxide, salicylic acid, tea tree oil, or whatever product they have.
- Nothing happens. The nodule persists.
- They try a different product, or apply more of the same one, sometimes irritating the overlying skin.
- The nodule eventually resolves on its own after weeks — but leaves a mark or scar.
- They assume the product worked slowly, when in reality, it did nothing.
This cycle is not just ineffective — it is actively harmful because it delays proper treatment. Every week that a nodule goes without appropriate medical care is another week of deep tissue inflammation and collagen destruction. Time is tissue when it comes to nodular acne.
What About Prescription Topicals?
Even prescription-strength topical treatments like tretinoin (Retin-A) or topical clindamycin have limited effectiveness against active nodules. These medications are valuable for preventing new comedones from forming and for treating mild-to-moderate acne, and your dermatologist may include them as part of a comprehensive treatment plan. But they cannot resolve an existing deep nodule on their own. Nodular acne requires systemic (whole-body) treatment, direct injection, or both.
Why Squeezing or Popping Is Catastrophic
When you have a hard, painful lump on your face that has been there for days, the temptation to squeeze it can feel overwhelming. We need to be very clear about this: attempting to squeeze, pop, or extract a nodule is one of the worst things you can do to your skin.
Here is why:
There Is Nothing to Pop
A nodule does not have a head. There is no pus-filled pocket near the surface waiting to be released. The inflammation is solid tissue deep in the dermis. When you squeeze a nodule, you are not releasing anything — you are compressing inflamed tissue against itself.
You Drive Infection Deeper
The pressure from squeezing forces inflammatory contents — bacteria, dead cells, and immune debris — even deeper into the dermis and potentially into the subcutaneous tissue below. This expands the area of inflammation, makes the nodule larger, and can cause it to spread laterally under the skin.
Scarring Becomes Almost Guaranteed
A nodule left untreated may scar. A nodule that has been squeezed will almost certainly scar, and the scar will be worse than it would have been otherwise. The mechanical trauma from squeezing damages the collagen framework in the dermis, and the deeper you drive the infection, the more tissue destruction occurs. This leads to deeper, more visible scars — including ice pick scars and rolling scars that are extremely difficult to treat later.
You Can Create Secondary Infection
Breaking the skin while trying to squeeze a nodule introduces additional bacteria from your fingers and nails into an already compromised area. This can cause a secondary bacterial infection on top of the existing acne inflammation, making everything significantly worse.
The bottom line: No matter how tempting it is, do not squeeze nodular acne. The short-term frustration of leaving it alone is nothing compared to the permanent scarring that results from attempting to pop it. If you need immediate relief, a cortisone injection from a dermatologist can flatten a nodule within 24-48 hours — and that is the only safe shortcut.
Professional Treatment Options
Nodular acne requires medical treatment. There is no shame in that — it simply means the condition has progressed beyond what consumer products can manage. Here are the treatments dermatologists use, ranging from first-line options to the most powerful tools available.
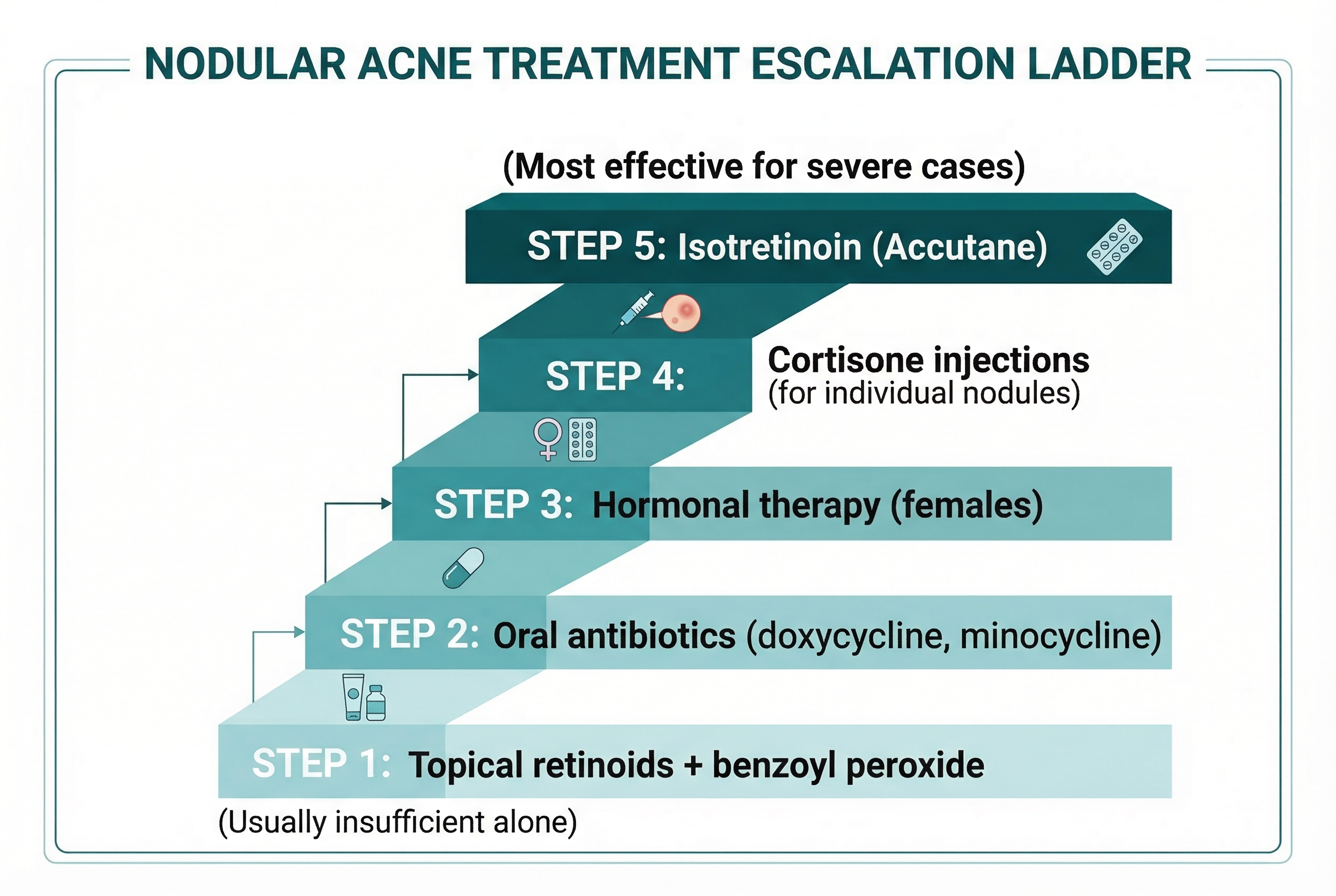
Oral Antibiotics
For many teens with nodular acne, oral antibiotics are one of the first prescription treatments a dermatologist will try. The most commonly prescribed are:
- Doxycycline — the most frequently used oral antibiotic for acne. It works by reducing C. acnes bacteria and, importantly, by suppressing the inflammatory response. The anti-inflammatory effect is actually more relevant for nodular acne than the antibacterial effect.
- Minocycline — similar to doxycycline but with slightly different absorption characteristics.
Oral antibiotics are typically prescribed for 3 to 6 months alongside topical retinoids and/or benzoyl peroxide. They are not intended as a long-term solution due to concerns about antibiotic resistance. Your dermatologist will plan a transition strategy — either tapering off the antibiotics while maintaining topical therapy, or moving to a different treatment if the response is insufficient.
For moderate nodular acne, oral antibiotics combined with topical therapy can produce meaningful improvement. However, for severe or widespread nodular acne, antibiotics alone may not be enough, and your dermatologist may recommend escalating to more powerful options.
Hormonal Therapy (for Girls and Women)
For teenage girls and young women whose nodular acne is significantly driven by hormonal factors, hormonal treatments can be highly effective:
- Combined oral contraceptives containing estrogen and progestin can reduce androgen levels and decrease sebum production. Several formulations are FDA-approved specifically for acne treatment.
- Spironolactone is an anti-androgen medication that blocks the effects of androgens on the oil glands. It is used off-label for acne in females and can be very effective for hormonally driven nodular acne.
Hormonal therapy is typically used in combination with other treatments, not as a standalone approach. It takes 2-3 months to see initial improvement and up to 6 months for full effect.
Isotretinoin (Accutane)
Isotretinoin is the single most effective treatment for severe nodular acne. It is the only medication that addresses all four causes of acne simultaneously: it dramatically reduces sebum production, normalizes follicular keratinization (preventing clogged pores), reduces C. acnes bacteria, and has anti-inflammatory effects.
For many teens with nodular acne, isotretinoin is not just an option — it is the recommended treatment. The American Academy of Dermatology guidelines state that isotretinoin should be considered as a first-line treatment for severe nodular acne, not merely as a last resort after other treatments have failed.
A typical course of isotretinoin:
- Lasts 5 to 7 months (sometimes longer)
- Requires monthly blood tests and monitoring
- Requires enrollment in a risk management program (iPLEDGE in the US) due to the risk of severe birth defects if taken during pregnancy
- Produces significant dryness of the skin, lips, and eyes as the most common side effect
- Achieves long-term remission in approximately 60-80% of patients after a single course
Isotretinoin has a long list of potential side effects that your dermatologist will discuss thoroughly. The decision to start it should involve a detailed conversation between the teen, their parents, and the dermatologist. But for severe nodular acne — especially when scarring is already occurring — the benefits almost always outweigh the risks.
When to push for isotretinoin: If your teen has been on oral antibiotics for 3-6 months with inadequate improvement, if nodules keep recurring despite treatment, or if scarring is developing, it is reasonable to have a direct conversation with your dermatologist about whether isotretinoin is appropriate. Do not wait until the acne has caused extensive scarring — by then, the damage is permanent.
Cortisone Injections
Cortisone (corticosteroid) injections deserve their own section because they serve a unique role in nodular acne treatment: they can provide rapid relief for individual, painful nodules.
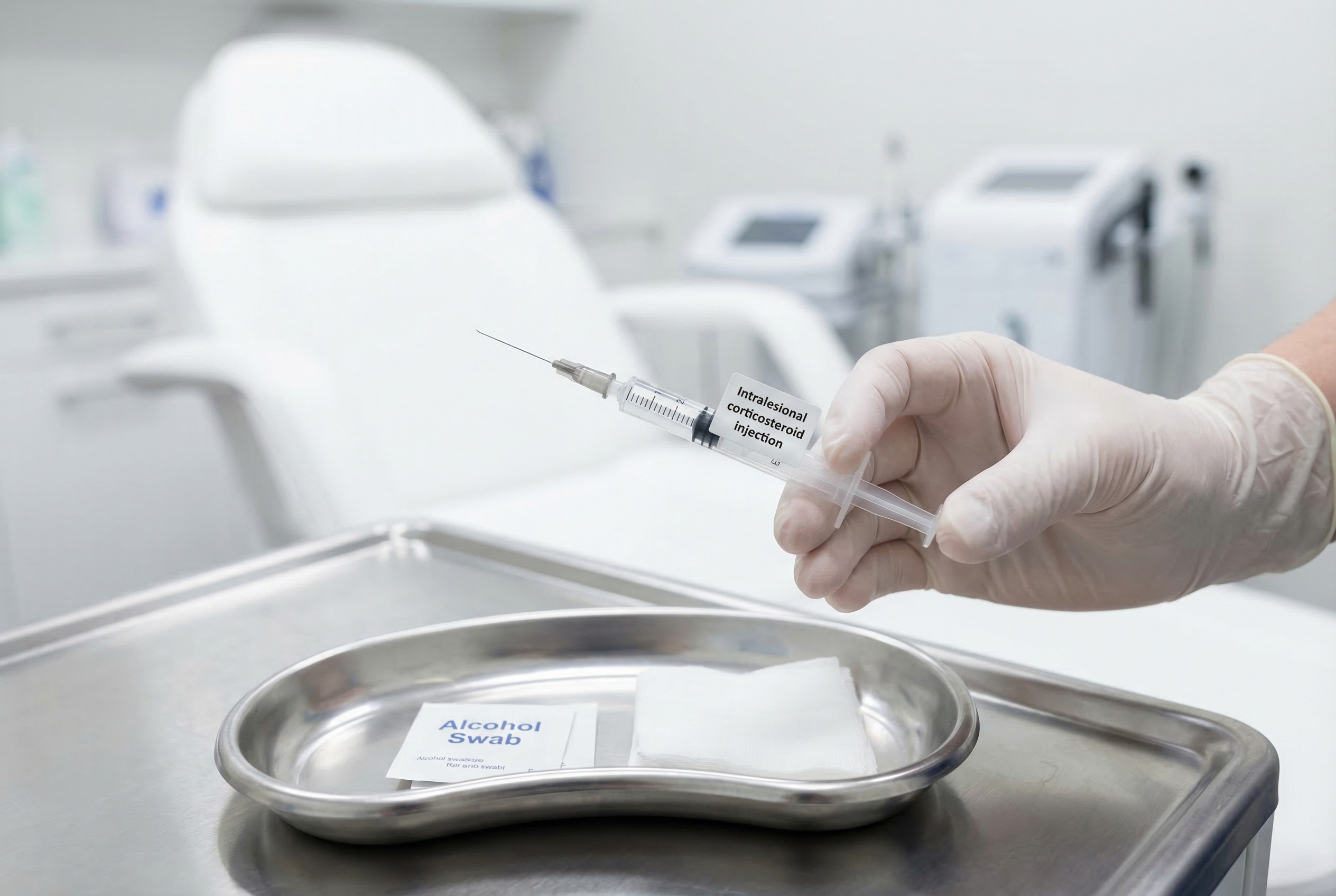
What Is a Cortisone Injection?
A cortisone injection — also called an intralesional corticosteroid injection — involves injecting a small amount of dilute corticosteroid (typically triamcinolone acetonide) directly into a nodule. The steroid suppresses the inflammatory response at the site, causing the nodule to flatten and the pain to subside.
What to Expect During the Procedure
If you are seeing a dermatologist for a cortisone injection, here is what the process looks like:
- The dermatologist cleans the area with alcohol or an antiseptic wipe.
- A very fine needle is inserted directly into the center of the nodule. The needle is small — most patients describe it as a brief sting.
- A small amount of corticosteroid solution is injected — usually just 0.05 to 0.1 mL per lesion.
- The entire procedure takes less than a minute per nodule. No anesthesia is typically required.
- You can resume normal activities immediately. There is no downtime.
Results and Timeline
- Within 24-48 hours, most nodules flatten significantly. Pain relief often begins within hours.
- Within 3-5 days, the nodule is usually fully resolved or nearly so.
- The injection treats the individual nodule, not the underlying condition. New nodules can still form. That is why cortisone injections are used alongside systemic treatment, not as a replacement for it.
Potential Side Effects
The most common side effect is skin atrophy — a small indentation or thinning of the skin at the injection site. This usually occurs if the concentration of the steroid is too high or if too much is injected. An experienced dermatologist minimizes this risk by using appropriately diluted solutions. In most cases, any mild atrophy resolves on its own within a few months.
Cortisone injections are particularly valuable for:
- A large, painful nodule before a significant event (school photos, prom, presentation)
- Nodules in highly visible areas causing significant distress
- Nodules that are not responding to systemic treatment as quickly as hoped
Scarring Prevention
Nodular acne has the highest scarring risk of any acne type. Understanding why — and what you can do about it — is critical.
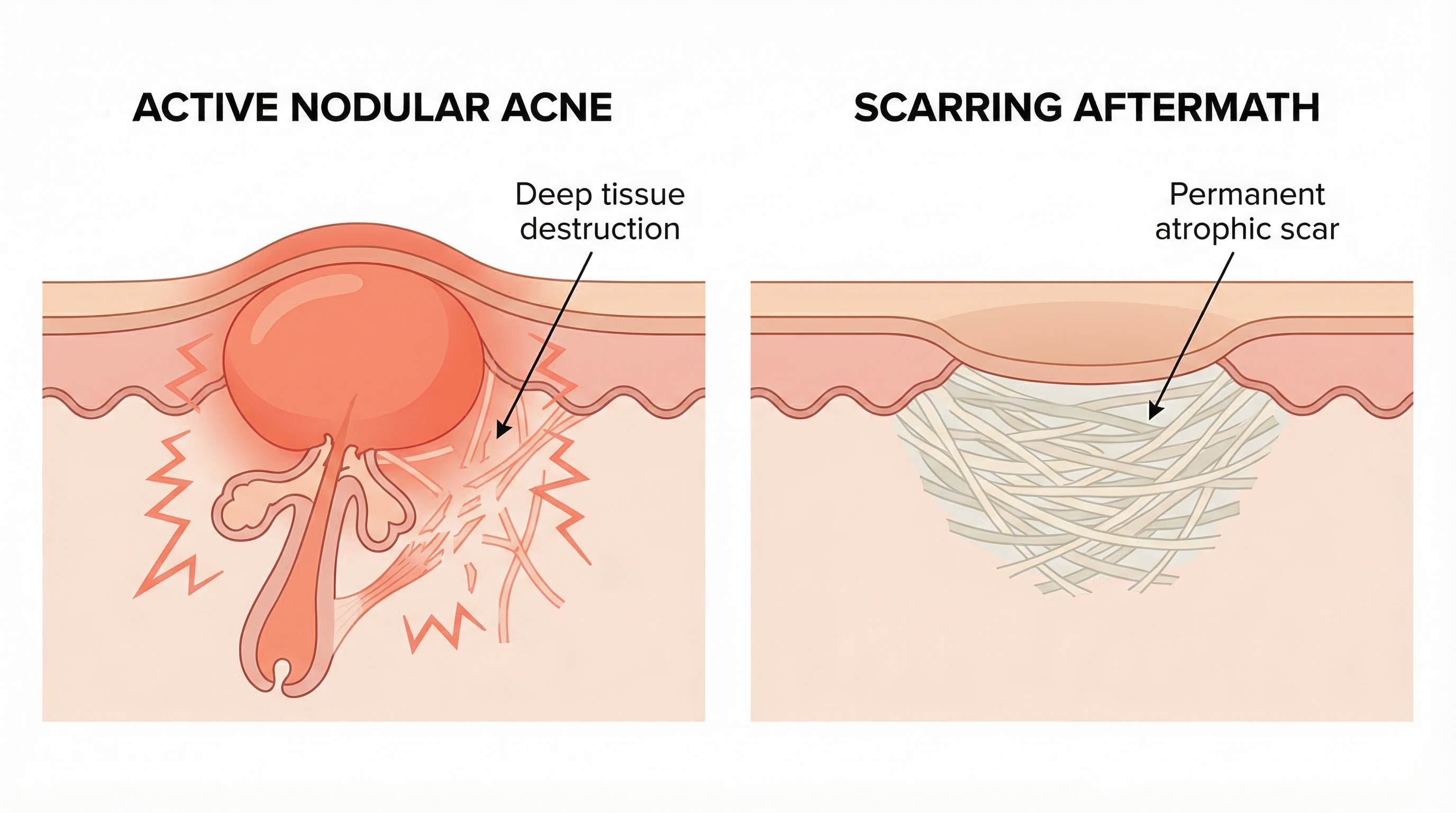
Why Nodular Acne Scars So Easily
The deep, prolonged inflammation of nodular acne directly destroys collagen in the dermis. Even without any squeezing or picking, a nodule can damage enough structural tissue to leave a permanent scar. The body attempts to repair the damage, but the repair process often produces either:
- Atrophic scars (depressions in the skin) — including ice pick scars, boxcar scars, and rolling scars. These form when the body cannot produce enough new collagen to replace what was destroyed.
- Hypertrophic or keloid scars (raised scars) — these form when the body overproduces collagen during the repair process. They are more common on the chest, back, and jawline.
The Most Effective Scar Prevention Strategy
There is really only one reliable way to prevent nodular acne scars: treat the acne aggressively and early. Every day that a nodule is actively inflamed is another day of tissue destruction. The strategies are straightforward:
- See a dermatologist as soon as nodular acne develops. Do not wait weeks or months hoping it will resolve.
- Follow the treatment plan consistently. Take prescribed medications as directed.
- Get cortisone injections for persistent, painful nodules to reduce the duration of inflammation.
- Do not pick, squeeze, or manipulate nodules. This is the single most controllable factor in scar prevention.
- Use sun protection diligently. UV exposure worsens post-inflammatory hyperpigmentation (the dark marks left after acne lesions heal) and can make scars more visible.
If scarring has already occurred, there are treatments available — including laser therapy, microneedling, chemical peels, and dermal fillers — but these are far more expensive, time-consuming, and less predictable than preventing the scars in the first place.
Living with Nodular Acne
Nodular acne is not just a skin condition. It is a daily experience that affects how you feel, how you interact with others, and how you see yourself. Acknowledging this is not being dramatic — research consistently shows that severe acne has a psychological impact comparable to chronic conditions like asthma, epilepsy, and diabetes.
The Emotional Weight
Teens with nodular acne often deal with:
- Physical pain — nodules genuinely hurt. Sleeping on the affected side, resting your chin on your hand, or even the pressure of a phone against your face can cause sharp pain.
- Self-consciousness — deep, inflamed bumps are often visible even under makeup or concealer, and teens are acutely aware of others' perceptions.
- Frustration with treatment timelines — unlike a surface pimple that might resolve in a week, nodular acne treatment takes months. Isotretinoin courses last 5-7 months. Oral antibiotics take weeks to show improvement. This requires patience that is difficult for anyone, let alone a teenager.
- Feeling misunderstood — well-meaning advice to "just wash your face more" or "stop eating junk food" is not only unhelpful but reinforces the false idea that nodular acne is caused by poor hygiene or lifestyle choices. It is not. It is a medical condition driven by genetics, hormones, and inflammatory biology.
Managing Day-to-Day Life During Treatment
While you are waiting for treatment to work, here are practical strategies:
- Use a gentle, non-irritating skincare routine. Harsh scrubs and astringents will not help nodules and will irritate already inflamed skin. A mild cleanser, appropriate moisturizer, and sunscreen are sufficient.
- Apply ice for pain relief. Wrapping an ice cube in a thin cloth and holding it against a painful nodule for 5-10 minutes can reduce inflammation and numb the pain temporarily.
- Talk to someone about how you feel. Whether it is a parent, school counselor, therapist, or trusted friend — the emotional burden of severe acne is real and valid. You do not have to pretend it does not affect you.
- Keep perspective on the timeline. Treatment works, but it takes time. Most teens with nodular acne see significant improvement within 3-6 months of starting appropriate medical therapy. Isotretinoin, in particular, produces dramatic results for the majority of patients.
Tip for parents: If your teen has nodular acne, take it seriously. Do not dismiss it as a normal part of adolescence that they will "grow out of." Advocate for a dermatology appointment — and if the first treatment plan is not working after a reasonable time, advocate for escalation. Your teen's skin, confidence, and emotional wellbeing are worth it.
Diet and Lifestyle Factors
Let's be honest about the role of diet and lifestyle in nodular acne: they are secondary factors, not primary causes. No amount of dietary change will cure nodular acne that requires isotretinoin. However, certain factors may influence acne severity on the margins, and they are worth being aware of.
What the Research Actually Shows
- High-glycemic foods — foods that cause rapid spikes in blood sugar (white bread, sugary drinks, processed snacks) have been associated with increased acne severity in some studies. The mechanism involves insulin and insulin-like growth factor (IGF-1), which can stimulate sebum production and promote inflammation.
- Dairy — some studies have found a weak association between dairy consumption (particularly skim milk) and acne. The evidence is not strong enough to make blanket recommendations, but if your teen notices a clear pattern, it may be worth discussing with their dermatologist.
- Stress — psychological stress can worsen acne through cortisol-mediated increases in sebum production and inflammatory responses. For teens already dealing with severe acne, this creates an unfortunate cycle: the acne causes stress, and the stress worsens the acne.
What This Means Practically
- Dietary changes alone will not resolve nodular acne. Do not delay seeking medical treatment in favor of trying elimination diets.
- Eating a balanced diet with lower glycemic load is good general health advice and may modestly support acne treatment.
- Stress management — through sleep, exercise, social support, and if needed, professional counseling — is genuinely helpful both for acne and for overall wellbeing.
- Exercise is beneficial for stress reduction and overall health. Shower promptly after sweating to prevent further irritation, but do not avoid physical activity because of acne.
When to See a Dermatologist
If you are reading this article, you probably already need to see a dermatologist. But to be specific, you should seek professional care if:
- You have hard, painful lumps under the skin that do not come to a head
- Deep acne bumps persist for more than 2-3 weeks without improvement
- Over-the-counter treatments have not worked after 8-12 weeks of consistent use
- You are developing scars — even small ones — from your acne
- Acne is causing significant emotional distress, affecting school attendance, social activities, or self-esteem
- You have a family history of severe acne and are beginning to develop deep lesions
Do not wait for nodular acne to become "bad enough" to justify seeing a doctor. It is already bad enough. Early intervention is the single most effective strategy for preventing permanent scarring and minimizing the emotional toll.
Bottom Line
Nodular acne is a severe medical condition, not a cosmetic inconvenience. These hard, painful lumps deep under your skin are the result of intense inflammation in the dermis — a process that no face wash, spot treatment, or home remedy can reach. Over-the-counter products are not going to fix this, and attempting to squeeze or pop nodules will make everything worse.
What does work is professional medical treatment. Oral antibiotics, hormonal therapy, isotretinoin, and cortisone injections are real, proven tools that dermatologists use every day to bring nodular acne under control. The earlier treatment begins, the less scarring occurs.
If you or your teen is dealing with nodular acne, please take it seriously and seek dermatological care. You deserve a treatment plan that matches the severity of what you are dealing with — and the right treatment can genuinely transform your skin and how you feel about it.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. (2016). Guidelines of care for the management of acne vulgaris. JAAD.https://pubmed.ncbi.nlm.nih.gov/26897386/
- Kraft J, Freiman A. (2011). Management of acne. CMAJ.https://pubmed.ncbi.nlm.nih.gov/21398228/
- Gollnick H, et al. (2003). Management of acne. JAAD.https://pubmed.ncbi.nlm.nih.gov/12734496/
- Thiboutot DM, et al. (2009). New insights into acne management. JAAD.https://pubmed.ncbi.nlm.nih.gov/19467365/
- Tanghetti EA. (2013). The role of inflammation in acne pathology. JCAD.https://pubmed.ncbi.nlm.nih.gov/24062871/
- Strauss JS, et al. (2007). Guidelines of care for acne vulgaris management. JAAD.https://pubmed.ncbi.nlm.nih.gov/17276540/
- Layton AM, et al. (1993). A review on the treatment of acne vulgaris. Journal of Clinical Pharmacy and Therapeutics.https://pubmed.ncbi.nlm.nih.gov/8126048/
- American Academy of Dermatology. Severe acne: Types and treatments.https://www.aad.org/public/diseases/acne/really-acne/severe
- Dréno B, et al. (2015). Understanding innate immunity and inflammation in acne. JEADV.https://pubmed.ncbi.nlm.nih.gov/25382740/
- Webster GF. (2005). The pathophysiology of acne. Cutis.https://pubmed.ncbi.nlm.nih.gov/15916220/
Read This Next

Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →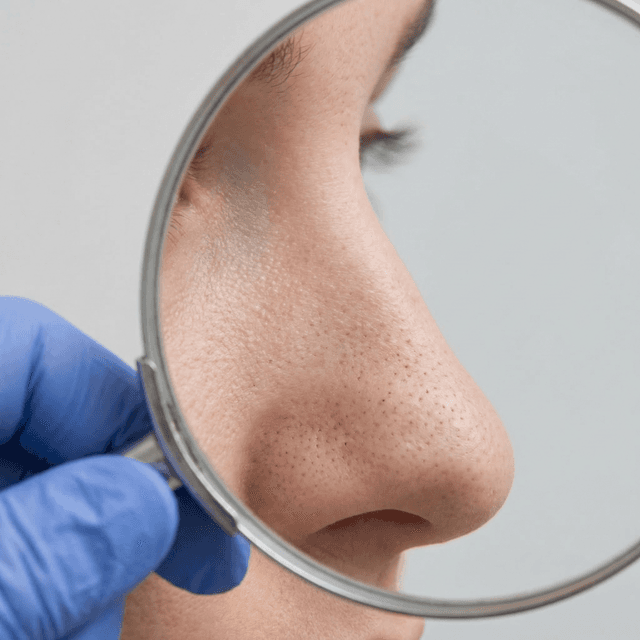
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →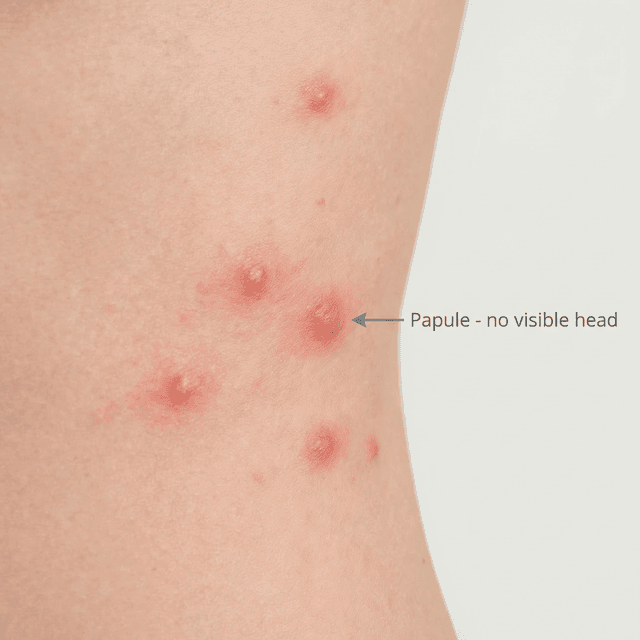
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →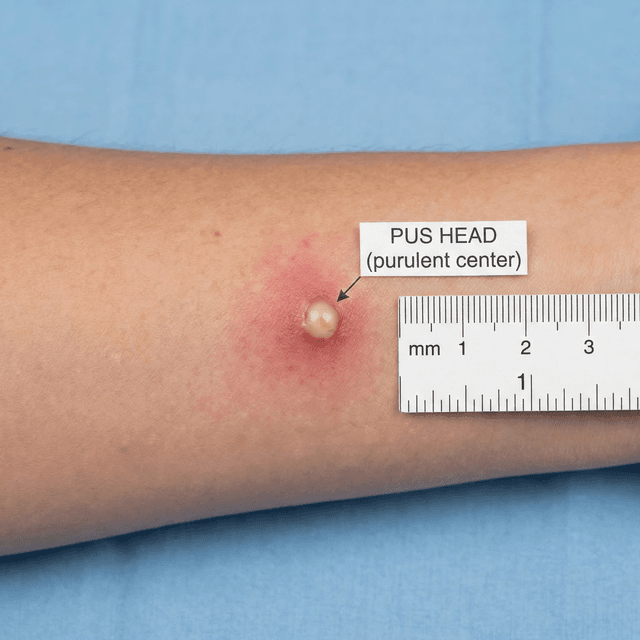
Pustules: The Classic Pimple — What's Inside, Should You Pop It, and How to Treat It
Pustules are what most people picture when they think 'pimple' — red bumps with a white or yellow center. Here's what's actually inside them, whether popping is ever okay, and what dermatologists recommend.
Read More →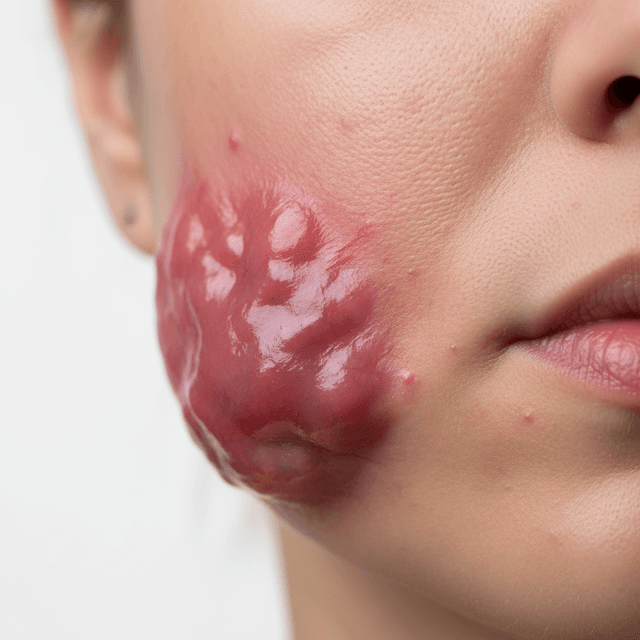
Cystic Acne: The Most Severe Form of Acne — Causes, Treatment, and What to Expect
Cystic acne is the most severe form of acne — large, painful, fluid-filled lesions deep under the skin. Here's what causes it, why it's so hard to treat, and what actually works.
Read More →