Body Acne vs. Facial Acne: Key Differences in Causes, Treatment, and What Works Where
Medically reviewed by Dr. Rachel Torres, MD, Pediatric Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated March 8, 2026
Key takeaways
- Body skin is significantly thicker than facial skin, which means it can tolerate stronger treatments
- Body acne is more commonly triggered by friction, sweat, and occlusion than facial acne
- You can safely use higher concentrations of benzoyl peroxide (up to 10%) on the body but not the face
- Chest and shoulder acne in teens is strongly correlated with hormonal surges during puberty
- Body acne that doesn't respond to OTC treatment may actually be folliculitis or keratosis pilaris, not acne
If you have ever tried to treat the breakouts on your back or chest using the same face wash and spot treatment you use on your forehead, you probably noticed something: it did not work the same way. Maybe the products felt too weak, or the breakouts just kept coming back no matter what you did.
That is because body acne and facial acne are not the same condition playing out on different parts of your skin. The skin on your trunk, shoulders, and back is structurally different from the skin on your face. It has different triggers, different underlying mechanics, and it responds to different treatment strategies. Understanding these differences is the first step toward actually clearing body acne instead of just throwing your facial products at it and hoping for the best.
In this guide, we break down everything you need to know about body acne vs. facial acne — from the biology behind each to the specific treatments that work where, and what you should never cross-apply between the two.
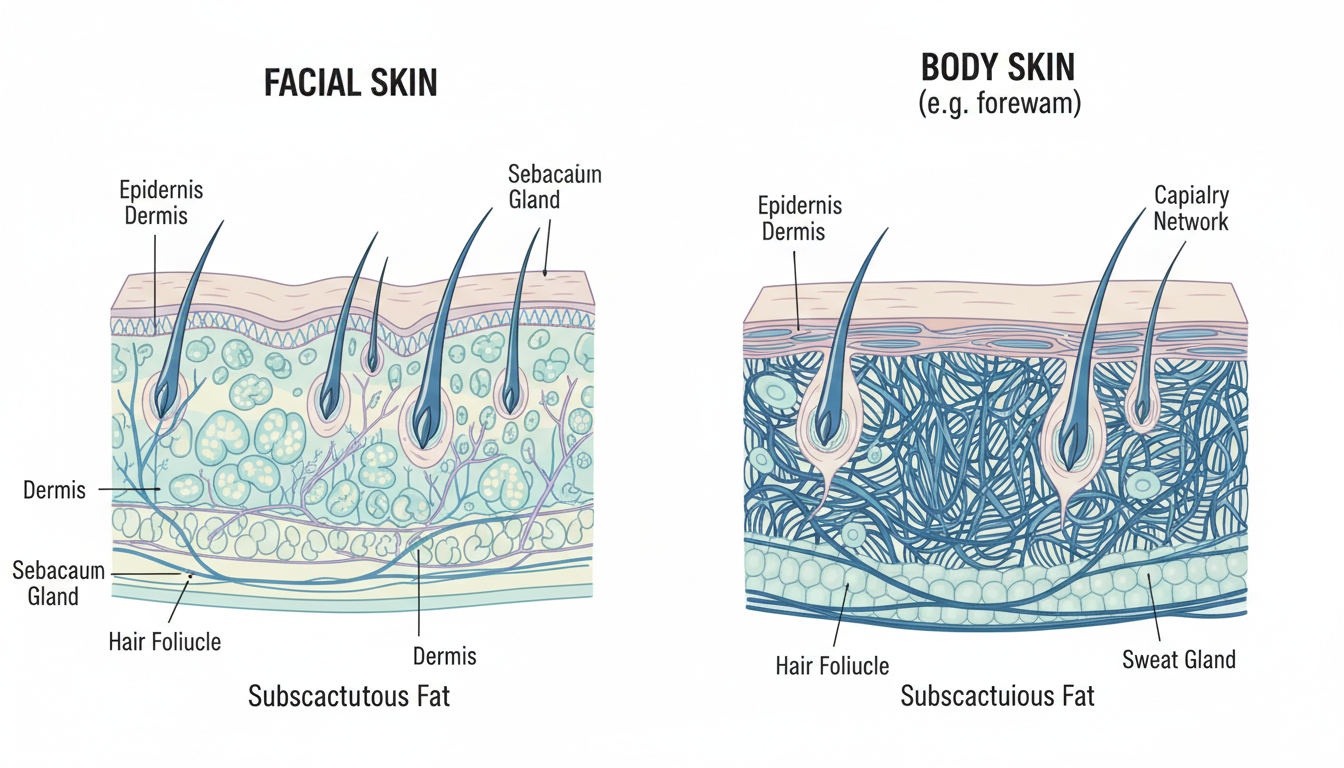
How Body Skin Differs from Facial Skin
Before we talk about acne itself, you need to understand the canvas it is forming on, because body skin and facial skin are dramatically different tissues.
Thickness and Barrier Strength
The skin on your face — particularly around the eyes and cheeks — is among the thinnest skin on your entire body, sometimes as thin as 0.5 mm. By contrast, the skin on your back, chest, and shoulders typically ranges from 2 to 4 mm thick. That is a significant structural difference.
This thickness matters for two reasons. First, thicker skin has a more robust barrier, which means it can tolerate stronger active ingredients without becoming irritated, red, or flaky. Second, that thickness also means topical treatments need to penetrate deeper to reach the follicles where acne actually forms. A gentle 2.5% benzoyl peroxide wash that works beautifully on your cheeks may barely make a dent on your upper back.
Pore Size and Sebaceous Gland Density
Your face has a high concentration of sebaceous (oil-producing) glands, especially across the T-zone. But the upper trunk — your chest, upper back, and shoulders — also has a remarkably high density of these glands. In fact, the mid-back and chest rank just behind the face in sebaceous gland concentration.
The pores on your body tend to be larger than facial pores. Larger pores can accumulate more sebum, dead skin cells, and debris before becoming visibly clogged, which is one reason body acne often presents as deeper, more inflamed lesions rather than the small comedones (blackheads and whiteheads) that are common on the face.
Microbiome Differences
The bacterial environment on your body is not the same as on your face. While Cutibacterium acnes (formerly Propionibacterium acnes) plays a central role in both facial and body acne, the relative abundance and strain diversity differ across body sites. The moist, occluded environments of the chest and back also support higher populations of Staphylococcus species and Malassezia yeast, which is why conditions that look like body acne sometimes turn out to be bacterial folliculitis or fungal folliculitis (pityrosporum folliculitis) rather than true acne vulgaris.
Sweat Gland Density and Occlusion
Your trunk has a high density of eccrine sweat glands. Sweat itself does not cause acne, but when sweat sits on the skin under clothing, it creates an occluded, humid environment. This combination of moisture, heat, and friction is a recipe for clogged pores and bacterial overgrowth — a situation that facial skin, which is almost always exposed to air, rarely faces.
Why Body Acne Happens
Body acne and facial acne share the same four fundamental mechanisms: excess sebum production, abnormal follicular keratinization (dead skin cells clogging pores), bacterial proliferation, and inflammation. But the triggers that set these mechanisms in motion differ significantly on the body.
Hormonal Drivers in Teens
If you are a teenager dealing with chest acne or shoulder acne, hormones are almost certainly a major factor. During puberty, rising levels of androgens — particularly testosterone and its derivative dihydrotestosterone (DHT) — stimulate sebaceous glands across the body to produce significantly more oil. The trunk is especially responsive to these hormonal signals.
This is why trunk acne in teenagers often appears suddenly, sometimes seeming to arrive all at once across the chest, shoulders, and upper back. It correlates directly with the hormonal surges that drive puberty, and it is especially common in teenage boys, though it affects girls as well.
Friction and Mechanical Irritation (Acne Mechanica)
One of the biggest differences between body acne and facial acne is the role of mechanical irritation. Body acne has a specific subtype — acne mechanica — that is caused or worsened by repeated friction, pressure, and heat against the skin.
Common culprits include:
- Backpack straps pressing against the shoulders and upper back for hours during the school day
- Sports equipment such as football pads, hockey gear, or tight-fitting compression shirts
- Bra straps and tight clothing that create constant friction across the chest and back
- Headbands, hats, and helmets (which can cause both facial and body acne along the hairline and forehead, bridging both zones)
If you notice that your body acne is worst exactly where your backpack straps sit or where your sports bra creates friction, acne mechanica is likely playing a significant role.
Sweat Occlusion
Sitting in sweaty workout clothes or a damp sports uniform after practice is one of the most common body acne triggers in teens. When sweat is trapped against the skin by clothing, it mixes with sebum and dead skin cells, creating an ideal environment for pore clogging and bacterial growth.
This does not happen on the face in the same way because facial skin is rarely covered by fabric for extended periods.
Products That Run Down
Here is a trigger that most people never think about: the products you use in the shower. Shampoo, conditioner, and hair styling products that rinse down your back and chest during showering can deposit pore-clogging ingredients on your body skin. Silicones, heavy oils, and sulfates in hair care products are common offenders.
This is a body-specific trigger that has no equivalent for facial acne, and it explains why some teens have acne concentrated on their upper back and shoulders (exactly where hair product runoff flows).
Laundry and Fabric Factors
Detergents, fabric softeners, and dryer sheets can leave residue on clothing and bedsheets that irritates the skin and contributes to body breakouts. Similarly, synthetic fabrics that do not breathe well can trap heat and moisture against the skin. These are meaningful triggers for body acne that have little relevance to facial acne.
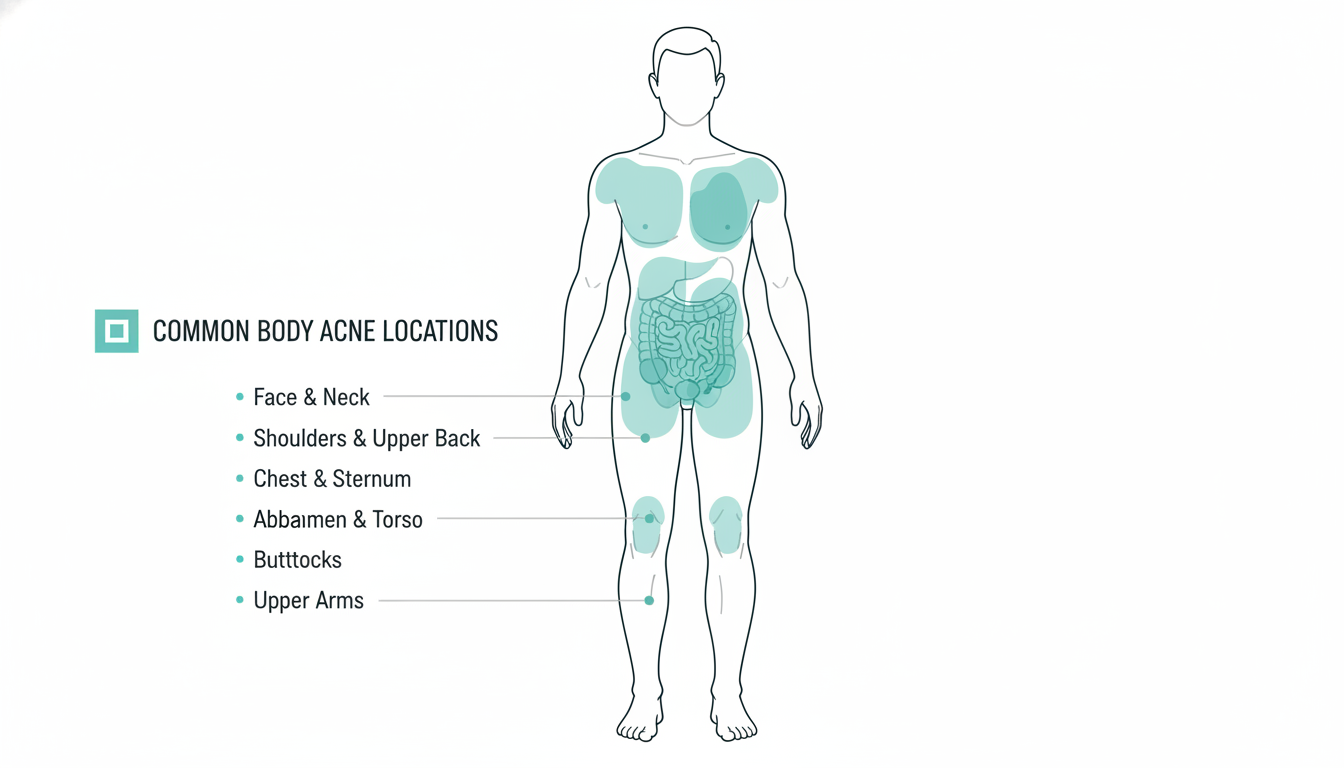
Common Body Acne Locations
Body acne does not appear randomly. It clusters in specific areas, and understanding why each location is affected can help you target treatment more effectively.
Back Acne ("Bacne")
The back, particularly the upper back between the shoulder blades, is the single most common site for body acne. This area has a high concentration of sebaceous glands, is constantly covered by clothing, experiences friction from backpacks and chair backs, and receives the runoff of hair products during showers. It is also one of the hardest areas to reach for self-treatment, which adds a practical challenge.
Back acne in teens tends to present as a mix of inflammatory papules and pustules alongside deeper nodules and cysts. Because the skin here is thick, lesions can be more severe and more likely to scar than facial acne of similar severity.
Chest Acne
Chest acne is extremely common during puberty, especially in boys. The central chest has a high density of sebaceous glands and is a site of significant androgen sensitivity. Tight-fitting shirts, sports jerseys, and the pressure of seatbelts can all contribute to chest breakouts.
Chest acne tends to be more visible and more psychologically distressing for many teens, particularly during summer or at the pool. Research published in the Journal of Clinical and Aesthetic Dermatology has found that visible body acne significantly impacts self-esteem and social participation in adolescents.
Shoulder Acne
Shoulder acne is particularly associated with acne mechanica. Backpack straps, purse straps, and athletic equipment all target this area. The shoulders also sit at the intersection of facial and trunk skin, with a transitional sebaceous gland density that makes them vulnerable to breakouts.
Upper Arms
The upper arms are a less common but still significant body acne site. However, it is important to distinguish true acne on the upper arms from keratosis pilaris (KP), a harmless condition that causes small, rough, sometimes reddish bumps on the outer upper arms. KP is caused by a buildup of keratin around hair follicles and is not acne at all — it does not respond to acne treatments and is managed with gentle exfoliation and moisturization instead.
Buttocks
Bumps on the buttocks are frequently assumed to be acne but are more often caused by folliculitis — an infection of the hair follicles, usually bacterial. True acne vulgaris on the buttocks is relatively uncommon because this area, despite experiencing significant friction and occlusion, has a lower density of the type of sebaceous glands involved in acne.
Treatment Differences
This is where the body acne vs. facial acne distinction becomes most practically important. The treatment strategies that work best for each are meaningfully different.
Benzoyl Peroxide: Different Concentrations for Different Sites
Benzoyl peroxide (BP) is the workhorse ingredient for both facial and body acne, but the appropriate concentration is very different.
For the face, most dermatologists recommend starting with 2.5% benzoyl peroxide, as research has shown that this concentration is nearly as effective as higher strengths while causing significantly less irritation on delicate facial skin. Going above 5% on the face often leads to excessive dryness, peeling, and redness without meaningful additional benefit.
For the body, however, you can safely use 5% to 10% benzoyl peroxide. The thicker skin on the trunk tolerates these higher concentrations well, and the stronger formulation is often necessary to penetrate effectively and kill acne-causing bacteria in the larger, deeper follicles of the back and chest.
Body-specific formulations also matter. For the back and hard-to-reach areas, BP body washes (used as a short-contact therapy, left on the skin for 2-3 minutes before rinsing) are far more practical than leave-on creams or gels that you would need someone else to apply. Spray formulations of benzoyl peroxide and salicylic acid are another body-specific option that allows you to treat your own back without contorting into awkward positions.
Wash-Off vs. Leave-On Treatments
On the face, leave-on treatments (serums, gels, lotions that stay on the skin) are the gold standard because they provide continuous active ingredient delivery throughout the day or night.
On the body, wash-off treatments are often more practical and equally effective. A benzoyl peroxide body wash used daily in the shower can deliver enough active ingredient to manage mild-to-moderate body acne. The key is contact time: let the wash sit on affected areas for at least two to three minutes before rinsing, rather than applying and immediately washing it off.
For more stubborn body acne, you can combine a wash-off treatment in the shower with a leave-on treatment (like a benzoyl peroxide spray or salicylic acid body lotion) applied after drying off.
Salicylic Acid on the Body
Salicylic acid at 0.5% to 2% is commonly used on the face, and these same concentrations can work on the body. However, because body skin is thicker and you are treating larger surface areas, look for body-specific formulations: salicylic acid body washes, exfoliating body sprays, and treatment pads designed for use on the trunk.
Salicylic acid is particularly useful for body acne because it is oil-soluble, meaning it can penetrate into oily pores and dissolve the sebum and dead skin cell mixture that clogs them. It is also anti-inflammatory, which helps with the often-inflamed lesions seen on the trunk.
Retinoids: Use with Caution on the Body
Topical retinoids (adapalene, tretinoin) are foundational treatments for facial acne, but they are less commonly used on the body for practical reasons. Applying retinoid cream across the entire back and chest requires a large amount of product, can be difficult to apply evenly, and the increased sun sensitivity across such a large area is harder to manage.
That said, adapalene gel (available over the counter as Differin) can be used on specific, focused areas of body acne — like a stubborn patch on the chest or a concentrated area on the shoulders. It is just not practical as a whole-trunk treatment for most people.
Shower Timing and Hygiene Adjustments
For body acne, when you shower matters almost as much as what you use. Key recommendations include:
- Shower immediately after sweating. Do not sit in sweaty clothes after sports practice, gym class, or physical activity. The combination of sweat, heat, and friction against the skin is a primary driver of body breakouts.
- Wash your body last in the shower. This ensures that any shampoo, conditioner, or hair product residue that has run down your back and chest is washed away in the final step.
- Use a clean towel and clean clothes after every shower. Reusing damp towels introduces bacteria back onto clean skin.
- Change out of wet swimsuits promptly. Prolonged occlusion from a wet swimsuit against the chest and back is a common summer trigger for body acne.
These hygiene-focused strategies have no real equivalent in facial acne care, where the skin is always exposed and the triggers are more about sebum and hormones than about clothing and sweat occlusion.

What You Can Use on Your Body but NOT Your Face
This section is critically important because one of the most common mistakes teens make is assuming that if a product is safe for the body, it must be safe for the face (or vice versa).
Higher-Strength Benzoyl Peroxide (Up to 10%)
As discussed, 10% benzoyl peroxide body washes and leave-on treatments are appropriate for trunk acne. Using 10% BP on the face is almost guaranteed to cause severe dryness, peeling, and irritation — and it is not more effective than 2.5% on facial skin.
Stronger Chemical Exfoliants
Body skin can tolerate higher concentrations of alpha-hydroxy acids (AHAs) like glycolic acid and lactic acid. Body lotions containing 10-12% glycolic acid can help with body acne and post-acne hyperpigmentation. These concentrations would be far too aggressive for the face, where 5-8% glycolic acid is typically the recommended range.
Medicated Body Sprays
Spray-on acne treatments containing salicylic acid or benzoyl peroxide are designed specifically for the body. They are formulated with alcohol bases that dry quickly on trunk skin but would be far too drying and irritating for the face. These sprays are particularly useful for hard-to-reach areas like the mid-back.
Physical Exfoliation
Gentle physical exfoliation with a long-handled body brush or exfoliating washcloth can be beneficial for body acne by removing dead skin cells that contribute to clogged pores. Physical exfoliation is generally discouraged on the face (especially acne-prone facial skin) because it can cause micro-tears and worsen inflammation. Body skin is tough enough to handle this approach when done gently and not more than two to three times per week.
Tea Tree Oil Body Washes
Tea tree oil at concentrations of 5% has shown some evidence for treating mild acne. Body washes containing tea tree oil can be a reasonable adjunct for body acne. However, tea tree oil at these concentrations applied directly to facial skin is more likely to cause contact irritation.
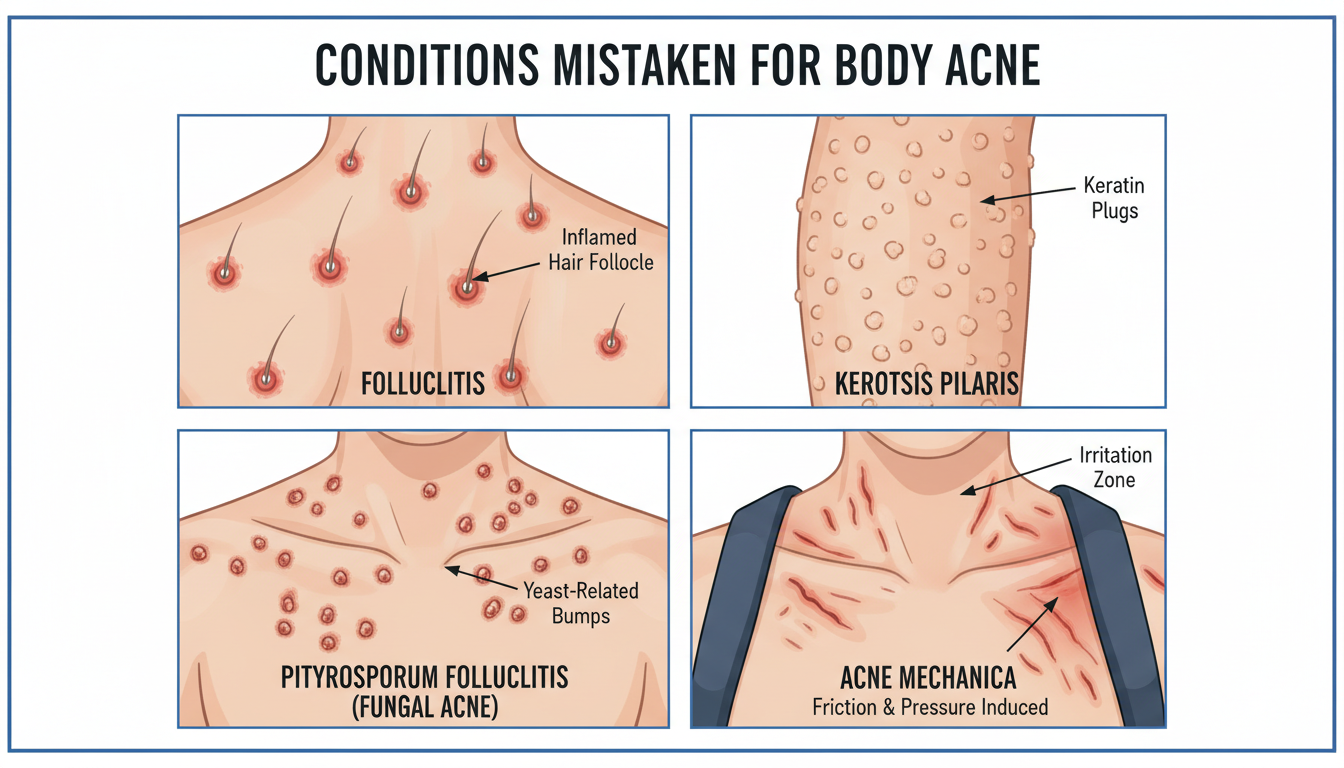
Conditions That Look Like Body Acne
One of the most important reasons to understand body acne is that several other conditions mimic its appearance on the trunk, and they require completely different treatment approaches. If your body acne is not responding to standard acne treatments, one of these conditions may be the actual cause.
Bacterial Folliculitis
Folliculitis is an infection of the hair follicles, usually caused by Staphylococcus aureus. It presents as small, red, often itchy bumps — sometimes with visible white or yellow pus — that look very similar to acne papules and pustules. Folliculitis is especially common on the buttocks, thighs, and areas subject to shaving or friction.
Key difference from acne: Folliculitis bumps tend to be uniform in size, are often itchy (acne is not usually itchy), and may have a visible hair at the center of each bump. Folliculitis is treated with antibacterial washes (like chlorhexidine or benzoyl peroxide wash), and sometimes oral antibiotics — not with retinoids or salicylic acid.
Fungal Folliculitis (Pityrosporum Folliculitis)
Caused by Malassezia yeast, fungal folliculitis is commonly misdiagnosed as acne. It presents as clusters of uniform, small, itchy bumps, usually on the chest, upper back, and shoulders — exactly where body acne also appears.
Key difference from acne: Fungal folliculitis does not respond to standard acne treatments and may actually worsen with antibiotic treatment (because killing competing bacteria allows the yeast to flourish). It is treated with antifungal agents such as ketoconazole shampoo used as a body wash, or oral antifungal medications in severe cases. If your body acne is itchy and consists of many small, uniform bumps that have not improved with benzoyl peroxide or salicylic acid, ask your dermatologist about fungal folliculitis.
Keratosis Pilaris (KP)
Keratosis pilaris causes small, rough, skin-colored or slightly reddish bumps, most commonly on the outer upper arms, thighs, and sometimes the buttocks and cheeks. It is caused by a buildup of keratin around hair follicles and is extremely common in teens.
Key difference from acne: KP bumps feel rough and sandpapery rather than inflamed or pus-filled. They are not caused by bacteria or excess sebum. KP is managed with gentle exfoliation (AHA or urea-based creams) and consistent moisturization — not with acne-specific treatments.
Hidradenitis Suppurativa (HS)
Hidradenitis suppurativa is a chronic inflammatory skin condition that causes painful, deep nodules and abscesses, typically in areas where skin rubs together — the armpits, groin, under the breasts, and inner thighs. In its early stages, HS can be mistaken for severe acne.
Key difference from acne: HS lesions tend to recur in the same locations, form sinus tracts (tunnels under the skin), and may drain foul-smelling fluid. HS requires specialized treatment and should be managed by a dermatologist. If you have recurring, painful deep lumps in your armpits, groin, or inner thighs that seem like they might be acne but never fully resolve, HS should be considered.
When Body Acne Signals Systemic Issues
In most teenagers, body acne is a normal — if frustrating — consequence of puberty. But in some cases, particularly severe or sudden-onset body acne can point to underlying systemic issues.
Hormonal Imbalances
In teen girls, severe body acne combined with other signs like irregular periods, excess body hair growth (hirsutism), or thinning scalp hair may suggest conditions such as polycystic ovary syndrome (PCOS) or other hormonal imbalances. These warrant evaluation by a healthcare provider.
Anabolic Steroid Use
In teenage boys, a sudden, severe outbreak of trunk acne — particularly large, inflamed nodular or cystic acne across the back, chest, and shoulders — can be associated with anabolic steroid use. This is sometimes called "steroid acne" and is a recognized clinical pattern. If a teen develops explosive body acne seemingly overnight, this possibility should be considered.
Medication Side Effects
Certain medications, including corticosteroids, lithium, some anticonvulsants, and testosterone-containing medications, can trigger or worsen body acne. If body acne worsened significantly after starting a new medication, discuss this with the prescribing doctor.
Prevention Strategies Specific to Body Acne
Because body acne has unique triggers, it also has unique prevention strategies that go beyond what you would do for your face.
Clothing and Fabric Choices
- Wear loose-fitting, breathable fabrics (cotton or moisture-wicking materials) during exercise and throughout the day
- Avoid wearing tight synthetic clothing for extended periods, especially in warm weather
- Change out of sweaty clothes immediately after physical activity
- Wash sports uniforms and workout clothes after every use — never rewear them without laundering
Shower Routine Optimization
- Shower as soon as possible after sweating
- Wash your body after rinsing out all hair products
- Use a medicated body wash containing benzoyl peroxide (5-10%) or salicylic acid (2%) on acne-prone areas
- Allow the medicated wash to sit on the skin for two to three minutes before rinsing
- Pat dry with a clean towel
Laundry Considerations
- Use fragrance-free, dye-free laundry detergent if you suspect laundry products are contributing to breakouts
- Skip fabric softeners and scented dryer sheets, which can leave residue on clothing that touches your skin
- Wash bedsheets at least once per week, and pillow cases even more frequently
Backpack and Equipment Adjustments
- Use padded backpack straps to reduce friction
- Wear a clean cotton t-shirt under sports equipment whenever possible
- Clean sports equipment regularly, as helmets, pads, and straps accumulate bacteria over time
- Consider switching to a rolling backpack if back and shoulder acne is severe
Hair Product Awareness
- If you use leave-in conditioners, oils, or styling products, be aware that these can run down your back in the shower or transfer to your skin during sleep
- Clip hair up or wrap it in a towel before applying body products
- Consider switching to lighter, non-comedogenic hair products if you notice a pattern between hair product use and back or shoulder breakouts
When to See a Dermatologist
Body acne is manageable at home in many cases, but certain situations call for professional evaluation.
See a dermatologist if:
- Over-the-counter treatments have not improved your body acne after 8 to 12 weeks of consistent use
- Your body acne is cystic or nodular — deep, painful bumps that do not come to a head
- You are developing scars from body acne (body acne scars on the chest and back can be particularly prominent and difficult to treat once established)
- Your body acne is widespread, covering large areas of the back, chest, and shoulders
- You suspect your bumps might be folliculitis, fungal acne, or another condition rather than true acne
- Body acne is significantly affecting your self-esteem, social participation, or daily life — avoiding swimming, not wanting to wear certain clothes, or skipping activities because of body acne are all valid reasons to seek help
- You notice signs of possible systemic issues, such as severe acne alongside irregular periods, excessive hair growth, or sudden changes in body acne severity
A dermatologist can prescribe treatments not available over the counter, including prescription-strength retinoids, oral antibiotics, hormonal therapies (for girls), and isotretinoin (Accutane) for severe, scarring body acne that has not responded to other treatments.
The Bottom Line
Body acne and facial acne may share the same underlying pathology, but they play out on fundamentally different skin with different triggers and different treatment needs. The skin on your trunk is thicker, can tolerate stronger products, and is subject to friction, occlusion, and sweat-related triggers that facial skin never encounters.
The most effective approach to body acne combines proper hygiene timing (shower after sweating, wash body last), appropriate-strength products (higher BP concentrations, medicated body washes, spray formulations for hard-to-reach areas), and trigger avoidance (breathable clothing, clean sports gear, mindful hair product use).
If your body acne is not responding to these strategies, do not just keep layering on more products. Consider whether the bumps might actually be folliculitis, fungal acne, or keratosis pilaris — conditions that look like body acne but require entirely different treatments. And if body acne is severe, scarring, or affecting your quality of life, a dermatologist visit is always worthwhile. Body acne is treatable, and you do not have to just wait for it to go away on its own.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. (2016). Guidelines of care for acne vulgaris. JAAD.https://pubmed.ncbi.nlm.nih.gov/26897386/
- Del Rosso JQ, et al. (2019). Status report on acne management. JCAD.https://pubmed.ncbi.nlm.nih.gov/30881582/
- Bhate K, Williams HC. (2013). Epidemiology of acne vulgaris. British Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/23210645/
- Kraft J, Freiman A. (2011). Management of acne. CMAJ.https://pubmed.ncbi.nlm.nih.gov/21398228/
- Gollnick H, et al. (2003). Management of acne. JAAD.https://pubmed.ncbi.nlm.nih.gov/12734496/
- Dréno B, et al. (2015). Understanding innate immunity and inflammation in acne. JEADV.https://pubmed.ncbi.nlm.nih.gov/25382740/
- Thiboutot DM, et al. (2009). New insights into acne management. JAAD.https://pubmed.ncbi.nlm.nih.gov/19467365/
- American Academy of Dermatology. Body acne.https://www.aad.org/public/diseases/acne/skin-care/body-acne
- Gallitano SM, Berson DS. (2018). How acne bumps cause the blues. JCAD.https://pubmed.ncbi.nlm.nih.gov/29844893/
- Tanghetti EA. (2013). The role of inflammation in acne pathology. JCAD.https://pubmed.ncbi.nlm.nih.gov/24062871/
Read This Next

Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →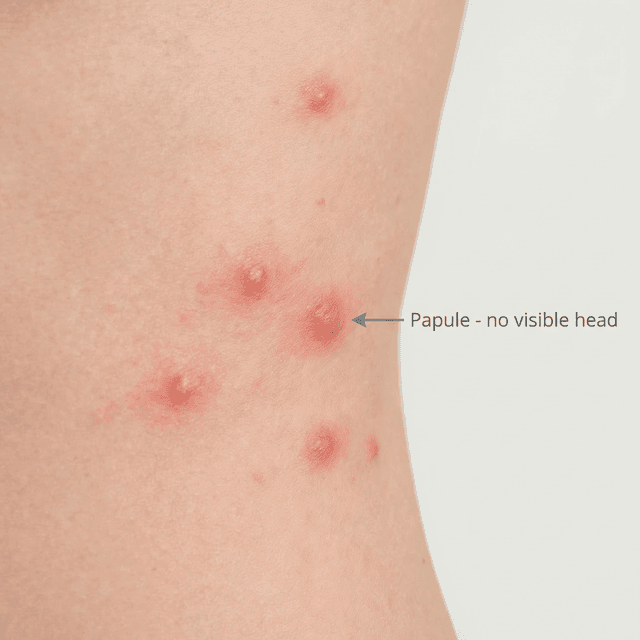
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →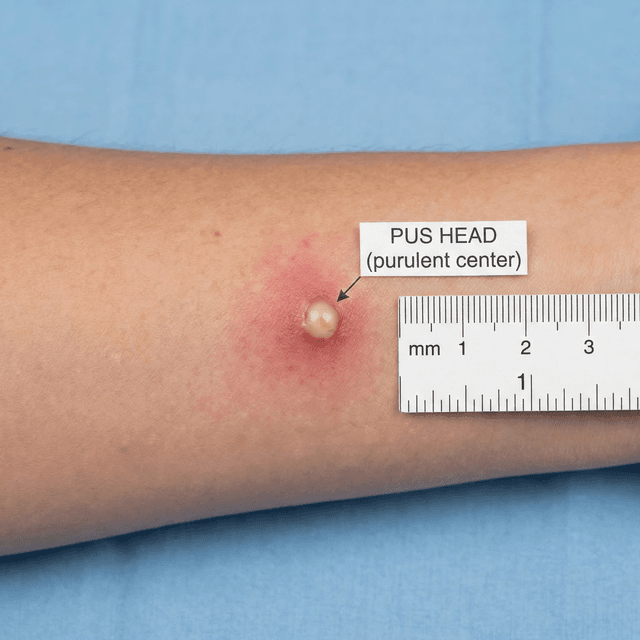
Pustules: The Classic Pimple — What's Inside, Should You Pop It, and How to Treat It
Pustules are what most people picture when they think 'pimple' — red bumps with a white or yellow center. Here's what's actually inside them, whether popping is ever okay, and what dermatologists recommend.
Read More →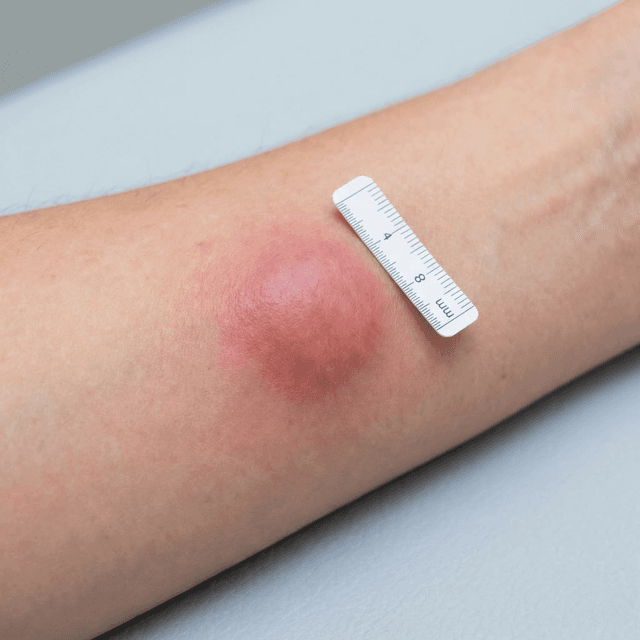
Nodular Acne: Understanding Deep, Painful Acne Bumps and Why They Need Professional Treatment
Hard, painful lumps deep under the skin that won't come to a head? That's nodular acne — a severe form that requires medical treatment. Here's what causes it and what actually works.
Read More →