Fungal Acne (Pityrosporum Folliculitis): Why Your 'Acne' Might Not Be Acne at All
Medically reviewed by Dr. James Chen, MD, Dermatology & Nutrition
Written by Teen Acne Solutions Editorial Team — Updated March 11, 2026
Key takeaways
- Fungal acne isn't actually acne — it's a yeast (Malassezia) infection of hair follicles called pityrosporum folliculitis
- It looks like uniform, small, itchy bumps — usually on the chest, back, shoulders, and forehead
- Traditional acne treatments (benzoyl peroxide, antibiotics) can actually make fungal acne WORSE
- Antifungal treatments (ketoconazole shampoo as body wash, oral fluconazole) are the correct approach
- Hot, humid weather, sweating, and antibiotics are common triggers
You've tried benzoyl peroxide. You've tried salicylic acid. You've tried switching cleansers, changing your pillowcase, cutting out dairy — and those small, stubborn bumps on your forehead or chest are still there. Maybe they've even gotten worse. If this sounds familiar, here's something that might change everything: what you're dealing with might not be acne at all.
Fungal acne — technically called pityrosporum folliculitis or Malassezia folliculitis — is one of the most commonly misdiagnosed skin conditions in teenagers and young adults. It looks a lot like acne. It shows up in the same places as acne. But it's caused by something completely different, and treating it like regular acne can actually make it worse. A lot worse.
This guide will help you figure out whether your breakouts might actually be fungal, what's going on beneath the surface, and exactly how to treat it if it is.
What Is Fungal Acne
Let's get the most important thing out of the way: fungal acne is not acne. The name is misleading, which is a big part of why it goes misdiagnosed so often. Dermatologists actually prefer the term pityrosporum folliculitis because it more accurately describes what's happening.
Regular acne (acne vulgaris) is caused by a combination of excess oil, dead skin cells, and the bacterium Cutibacterium acnes clogging your pores. Fungal acne is caused by an overgrowth of Malassezia yeast — a type of fungus that naturally lives on everyone's skin.
Malassezia: The Yeast That Lives on Your Skin
Here's something that might surprise you: Malassezia yeast is already on your skin right now. It's on everyone's skin. Research published in the International Journal of Dermatology has identified Malassezia species as part of the normal skin microbiome — the community of microorganisms that live on healthy human skin. Under normal circumstances, it's completely harmless.
The problem starts when something disrupts the balance. When Malassezia yeast is given the conditions to overgrow — warm, moist, oily environments — it starts colonizing hair follicles. The yeast feeds on oils (specifically triglycerides and fatty acids in sebum), and as it multiplies, it triggers an inflammatory immune response. Your body recognizes the overgrowth as a threat and reacts by sending inflammatory cells to the affected follicles.
The result? Itchy, inflamed bumps that look almost exactly like acne but don't respond to a single acne treatment you throw at them.
Who Gets Fungal Acne?
Pityrosporum folliculitis is particularly common in teenagers and young adults, which makes it even easier to confuse with regular hormonal acne. Studies have found that it's most prevalent in people between the ages of 13 and 45, with a significant concentration in the teen and young adult years — the exact age range where acne vulgaris is also at its peak.
It's also more common in warm, humid climates. Research from the Philippines found that pityrosporum folliculitis was one of the most frequently diagnosed follicular conditions in tropical regions, where heat and humidity create ideal conditions for Malassezia overgrowth. But you don't need to live in the tropics — any situation that creates a warm, sweaty environment on your skin can trigger it.
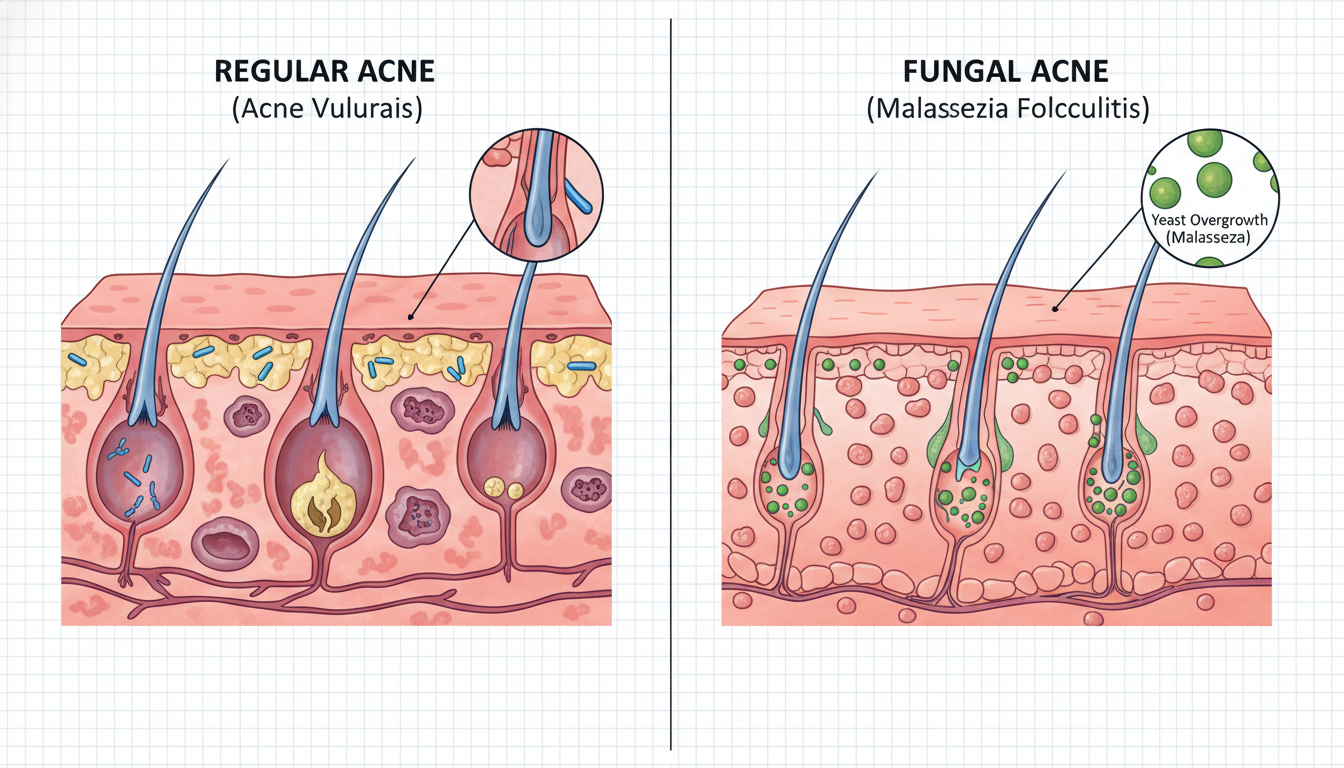
Fungal Acne vs Regular Acne
This is the question that matters most: how do you tell the difference? While a dermatologist can confirm the diagnosis with a skin scraping or biopsy, there are several visual and symptomatic clues that can help you figure out what you're dealing with.
Appearance
This is the biggest giveaway. Regular acne comes in a variety of shapes and sizes — blackheads, whiteheads, papules, pustules, cysts, nodules. You'll typically see a mix of lesion types on your face or body, and they tend to vary in size.
Fungal acne looks different. The bumps are:
- Uniform in size — typically 1-2mm, all roughly the same diameter
- Monomorphic — meaning they all look the same, rather than a mix of different lesion types
- Flesh-colored or slightly pink/red — sometimes with a tiny whitehead, but not the angry, varied redness of inflammatory acne
- Clustered together — often appearing in dense patches rather than scattered randomly
When dermatologists describe pityrosporum folliculitis in clinical literature, the word "monomorphic" comes up again and again. If your bumps all look eerily identical — like someone stamped them out with the same mold — that's a significant clue.
Location
Fungal acne has a strong preference for specific body areas:
- Chest and upper back — the most common sites
- Shoulders
- Forehead — especially along the hairline
- Upper arms
It tends to favor areas with a high density of oil glands and hair follicles, and areas where sweat and heat get trapped. It's less common on the cheeks, nose, and chin — the areas where regular acne typically concentrates.
That said, fungal acne can appear on the face, particularly the forehead. If you have persistent, tiny, uniform bumps across your forehead that won't budge no matter what acne treatment you use, fungal acne should be on your radar.
Itchiness
This is one of the most reliable distinguishing symptoms. Fungal acne itches. Regular acne can be tender, sore, or painful — but itching is not a hallmark of acne vulgaris. If your breakouts are consistently itchy, especially when you're sweating or in a warm environment, that strongly suggests a fungal component.
Multiple studies have identified pruritus (itching) as one of the most commonly reported symptoms of pityrosporum folliculitis, with some research finding that up to 80% of patients experience itchiness as their primary complaint.
Response to Treatment
Perhaps the most frustrating clue — and often the one that finally leads to a correct diagnosis — is how the bumps respond to treatment. If you've been diligently using acne treatments for weeks or months with zero improvement (or if things are getting worse), it's time to consider that you might not be dealing with acne.
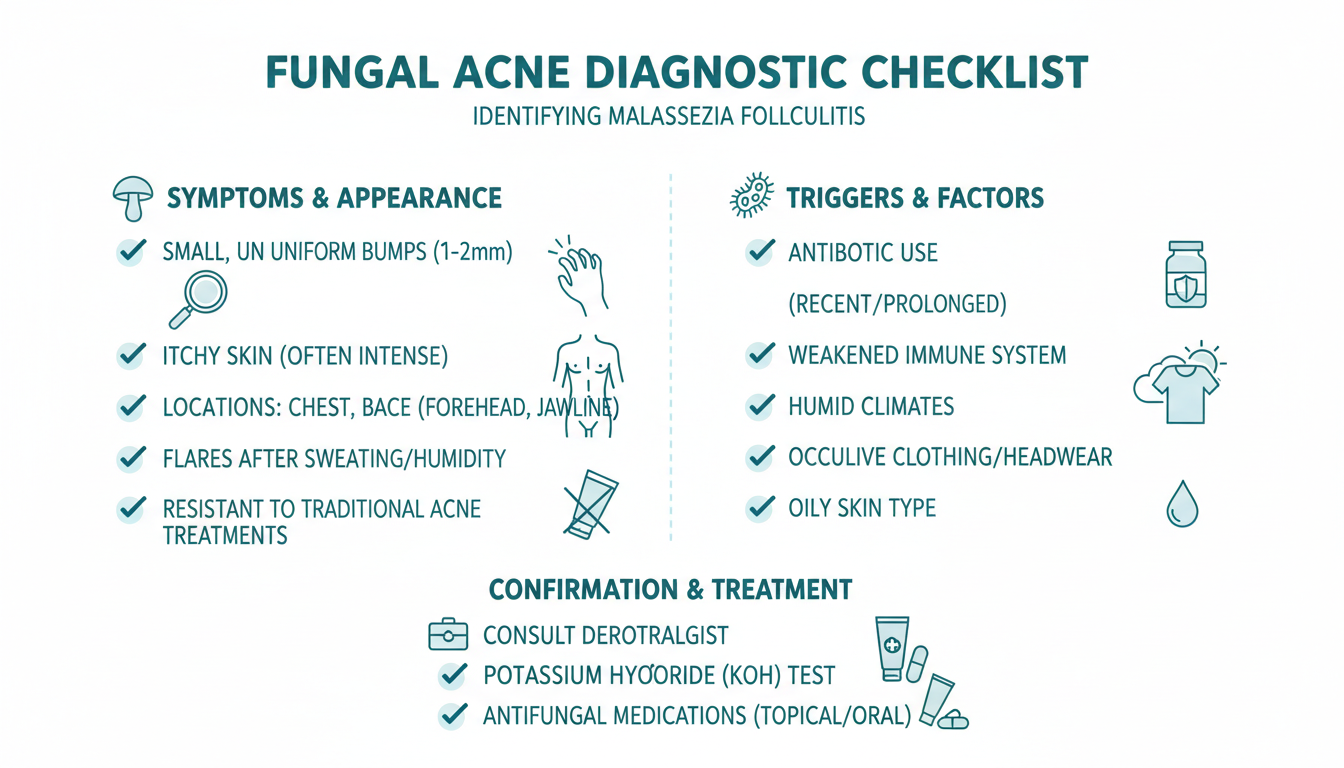
How to Tell the Difference
Here's a practical checklist you can use to evaluate your breakouts. The more boxes you check, the more likely your "acne" is actually pityrosporum folliculitis:
- Are the bumps itchy? Regular acne is tender or painful, not typically itchy. Itchiness is a hallmark of fungal acne.
- Are the bumps all the same size? Fungal acne produces monomorphic (uniform) bumps. Regular acne comes in a mix of types and sizes.
- Are they concentrated on your chest, back, shoulders, or forehead? These are the classic fungal acne zones.
- Do they get worse in hot, humid weather or after sweating? Heat and moisture fuel Malassezia overgrowth.
- Have you recently taken antibiotics? Antibiotics disrupt the skin's microbial balance, giving yeast an opportunity to overgrow.
- Have standard acne treatments failed to improve the breakouts? Benzoyl peroxide, salicylic acid, and topical retinoids don't address yeast — so they won't help.
- Do the bumps appear suddenly in clusters? Fungal acne often flares up quickly in dense patches, rather than developing gradually like most hormonal acne.
If you checked 3 or more of these, there's a reasonable chance your breakouts are fungal in nature. But the only way to confirm for certain is through a dermatologist visit. They can perform a simple skin scraping, examine it under a microscope using a KOH (potassium hydroxide) preparation, or use a Wood's lamp (a type of UV light) to look for Malassezia yeast.
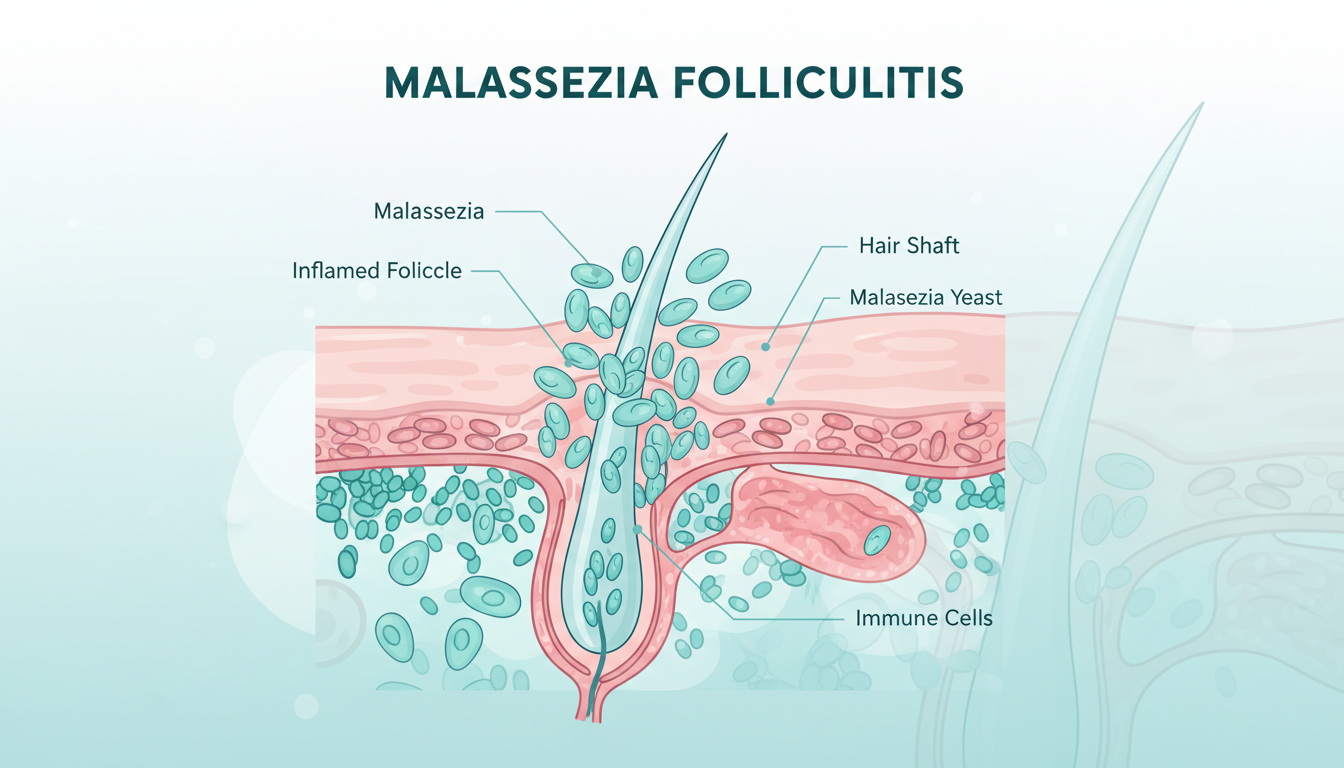
What Causes Fungal Acne
Understanding what triggers Malassezia overgrowth can help you figure out why this is happening — and how to prevent it from coming back.
Heat and Humidity
This is the most common trigger, especially for teens. Malassezia yeast thrives in warm, moist environments. If you live in a humid climate, sweat heavily during sports, or regularly wear clothes that trap heat against your skin, you're creating optimal conditions for yeast growth. Studies have consistently shown higher rates of pityrosporum folliculitis in tropical and subtropical regions.
Sweating and Occlusion
Sweat itself doesn't cause fungal acne, but when sweat is trapped against the skin — by tight clothing, athletic gear, backpack straps, or non-breathable fabrics — it creates the warm, moist microenvironment that Malassezia loves. This is why fungal acne often flares up during sports seasons, summer months, or after workouts.
Antibiotics
This is a big one, and it catches a lot of people off guard. When you take oral antibiotics — including antibiotics prescribed for acne like doxycycline or minocycline — they kill bacteria across your body. That includes the beneficial bacteria on your skin that naturally compete with Malassezia yeast and help keep its population in check.
Research published in the Journal of Clinical and Aesthetic Dermatology has documented cases where pityrosporum folliculitis developed or worsened directly after a course of antibiotics. This creates a frustrating paradox: you go to the doctor for "acne," get prescribed antibiotics, and the antibiotics actually make the problem worse because the problem was yeast-based, not bacterial, all along.
Occlusive Skincare and Makeup Products
Many skincare products, moisturizers, sunscreens, and makeup products contain ingredients that feed Malassezia yeast. Specifically, Malassezia feeds on certain fatty acids — particularly those with carbon chain lengths of 11-24. Products that contain these fatty acids (which is a large number of conventional skincare products) can literally be feeding the yeast on your skin.
Occlusive products that trap moisture against the skin — thick creams, heavy oils, petroleum-based products — also create the sealed, moist environment that promotes yeast growth.
Immunosuppression
People with weakened immune systems — whether from medical conditions, medications, or chronic stress — are more susceptible to Malassezia overgrowth because their immune system is less capable of keeping the yeast population under control. For most teens, this isn't the primary factor, but if you're dealing with high stress levels or an underlying health condition, it could be contributing.
Oily Skin
Since Malassezia feeds on the oils in sebum, people with naturally oily skin produce a larger food source for the yeast. Teenagers going through puberty often experience a significant increase in oil production due to hormonal changes — which is why fungal acne and regular acne can so easily coexist during these years.
Why Regular Acne Treatment Makes It Worse
This is the part that frustrates so many people — and it's worth understanding the mechanism so you can avoid the trap.
Antibiotics: Removing the Competition
As mentioned above, oral antibiotics kill bacteria — including the bacteria that naturally compete with Malassezia yeast on your skin. Think of your skin's microbiome as an ecosystem. Bacteria and yeast are constantly competing for the same resources (space, nutrients, oil). When you wipe out bacteria with antibiotics, the yeast suddenly has the field to itself. No competition means unchecked growth.
This is well-documented in dermatological literature. A 2020 review published in Frontiers in Cellular and Infection Microbiology noted that antibiotic use is a recognized predisposing factor for pityrosporum folliculitis precisely because it disrupts the microbial balance of the skin.
Benzoyl Peroxide: Wrong Target
Benzoyl peroxide is one of the most effective ingredients for regular acne because it kills Cutibacterium acnes bacteria. But Malassezia is a yeast, not a bacterium. Benzoyl peroxide doesn't address it. While it won't necessarily make fungal acne dramatically worse the way antibiotics can, using it as your primary treatment is essentially a waste of time when yeast is the underlying cause.
Heavy Moisturizers to Combat Dryness
Many acne treatments dry out the skin, so the standard advice is to use a moisturizer. The problem? Many conventional moisturizers contain fatty acids and oils that feed Malassezia. So you use a drying acne treatment that doesn't address the yeast, your skin gets dry and irritated, you apply a moisturizer that feeds the yeast, and the cycle continues. It's a lose-lose situation when you're fighting the wrong enemy.
How to Treat Fungal Acne
The good news is that once you identify the problem correctly, fungal acne responds remarkably well to the right treatment. Most people see significant improvement within 2-4 weeks.
Topical Antifungal Treatments
These are the first line of defense and often all you need.
Ketoconazole shampoo as body wash or face wash. This is the most commonly recommended approach by dermatologists. Over-the-counter ketoconazole shampoo (2%) — brands like Nizoral are widely available — can be used as a body wash or face wash on affected areas. Apply it to damp skin, let it sit for 3-5 minutes so the antifungal has time to work, then rinse thoroughly. Use it daily for 2-4 weeks, then reduce to 2-3 times per week for maintenance.
Zinc pyrithione wash. Another effective antifungal option that's available over the counter. Zinc pyrithione (found in some dandruff shampoos) has antifungal and antibacterial properties. It works well as an alternative if ketoconazole irritates your skin, or it can be used in combination — alternating between the two.
Selenium sulfide shampoo. Products containing 1-2.5% selenium sulfide (like Selsun Blue) also have antifungal properties and can be used as a body wash with the same leave-on technique.
Topical antifungal creams. Clotrimazole, miconazole, or ketoconazole cream can be applied directly to affected areas, especially on the face where using a shampoo might feel awkward. Apply a thin layer once or twice daily to clean skin.
Oral Antifungal Medications
For more stubborn or widespread cases, a dermatologist may prescribe oral antifungal medication.
Fluconazole is one of the most commonly prescribed options. A typical course might be 150-200mg once weekly for 2-4 weeks, or a shorter course of daily doses. Studies have shown high efficacy rates with oral fluconazole for pityrosporum folliculitis.
Itraconazole is another option, typically prescribed as 200mg daily for 1-2 weeks.
Important: Oral antifungals require a prescription and can interact with other medications. They also require monitoring in some cases. This is something to discuss with your dermatologist — don't try to self-treat with oral antifungals.
Adjusting Your Skincare Routine
This step is just as important as the antifungal treatment itself. If your skincare products are feeding the yeast, even the best antifungal won't fully solve the problem.
Switch to fungal-safe products. This means checking ingredient lists and avoiding products that contain Malassezia food sources. More on this in the next section.
Simplify your routine. While your skin is recovering, less is more. A gentle cleanser, antifungal treatment, and a simple, fungal-safe moisturizer is all you need.
Avoid heavy, occlusive products. Thick creams, heavy oils, and occlusive balms trap moisture and create the environment yeast loves. Opt for lightweight, gel-based, or oil-free products instead.
The Fungal-Safe Ingredient Checklist
Not all oils and fatty acids feed Malassezia, and learning which to avoid can make a big difference. Here's a practical guide:
Ingredients to AVOID (feed Malassezia):
- Fatty acids with carbon chain lengths of 11-24 (lauric acid, myristic acid, palmitic acid, stearic acid, oleic acid)
- Most plant oils (coconut oil, olive oil, sunflower oil, jojoba oil)
- Fatty alcohols in some formulations (cetearyl alcohol, cetyl alcohol — though these are debated and don't always cause issues)
- Esters derived from problematic fatty acids (isopropyl myristate, isopropyl palmitate)
- Polysorbates (polysorbate 20, polysorbate 60, polysorbate 80)
- Galactomyces and fermented ingredients (these may promote yeast growth in some individuals)
Ingredients that are generally SAFE:
- Squalane oil (a notable exception — it doesn't feed Malassezia)
- MCT oil (C8/C10 caprylic/capric triglycerides — shorter chain lengths that Malassezia can't metabolize)
- Mineral oil (not a food source for yeast)
- Hyaluronic acid
- Niacinamide
- Glycerin
- Aloe vera
- Salicylic acid (while it won't treat the yeast, it helps with follicular unclogging and won't worsen fungal acne)
- Sulfur-based treatments
- Zinc-based products
Tip: Websites and apps like "Folliculitis Scout" and "SkinSort" allow you to paste ingredient lists and check whether a product is fungal-safe. This can save you a lot of time when shopping for new skincare.
Prevention
Once you've gotten fungal acne under control, preventing recurrence is all about managing the conditions that let Malassezia overgrow in the first place.
Shower Promptly After Sweating
This is the single most important preventive habit. Don't let sweat sit on your skin. After gym class, sports practice, or any activity that makes you sweat, shower as soon as possible. If you can't shower right away, at minimum change into clean, dry clothes and use a body wipe on affected areas.
Use an Antifungal Wash for Maintenance
Even after your fungal acne has cleared, using a ketoconazole or zinc pyrithione wash 1-2 times per week on prone areas can keep Malassezia populations in check and prevent flare-ups. Think of it like maintaining the balance rather than fighting an active infection.
Wear Breathable Fabrics
Cotton, linen, and moisture-wicking athletic fabrics allow sweat to evaporate rather than getting trapped against your skin. Avoid wearing tight synthetic shirts for extended periods, especially in warm weather. If you wear a sports uniform made of non-breathable material, change out of it as soon as your game or practice ends.
Keep Your Skincare Fungal-Safe
Once you've identified products that work for your skin without feeding Malassezia, stick with them. This doesn't mean you need to obsessively check every single product — but for the products that go on your most prone areas (chest, back, forehead), it's worth making sure they're not undermining your efforts.
Be Cautious with Antibiotics
If a doctor prescribes antibiotics for any reason — whether for acne, a sinus infection, strep throat, or anything else — be aware that this can trigger a fungal acne flare. If you have a history of pityrosporum folliculitis, mention it to your doctor. They may recommend a preventive antifungal during or after your antibiotic course, or they may be able to choose an alternative treatment that doesn't carry the same risk.
Manage Oil Production
Since Malassezia feeds on sebum, managing excess oil can help starve the yeast. Washing prone areas with a gentle cleanser twice daily, using oil-free products, and in some cases using ingredients like niacinamide (which helps regulate oil production) can all contribute.
Change Out of Sweaty Clothes Quickly
This sounds obvious, but it's worth emphasizing because so many teens don't do it. Sitting in a sweaty gym shirt for the rest of the school day, sleeping in clothes you wore all day, or re-wearing athletic gear without washing it — these habits create the warm, moist conditions that Malassezia thrives in.
When Fungal Acne and Regular Acne Coexist
Here's a complication that makes this whole topic even trickier: you can have both fungal acne and regular acne at the same time. This is actually quite common in teenagers, since the hormonal changes of puberty drive both increased oil production (feeding Malassezia) and increased bacterial acne.
If this is the case, you'll need a treatment plan that addresses both conditions. A dermatologist can help you navigate this — typically by combining an antifungal treatment for the fungal component with a bacterial acne treatment that won't worsen the yeast issue. Salicylic acid and azelaic acid are often good choices here because they address acne without feeding Malassezia or disrupting the microbial balance the way antibiotics do.
See a Dermatologist If You're Unsure
While this guide can help you identify the signs of fungal acne and start taking the right steps, a dermatologist is the only person who can give you a definitive diagnosis. A simple skin scraping examined under a microscope can confirm whether Malassezia yeast is present in your follicles. This takes minutes and removes all the guesswork.
If your breakouts match the patterns described in this article — uniform bumps, itchiness, specific locations, failure to respond to acne treatments — bring up the possibility of pityrosporum folliculitis at your appointment. Unfortunately, fungal acne is still under-recognized, and some general practitioners may not consider it. Being your own advocate and asking the right questions can make the difference between years of frustrating misdiagnosis and a treatment that actually works.
Bottom Line
Fungal acne is one of the most frustrating skin conditions a teenager can face — not because it's hard to treat, but because it's so often treated as the wrong thing. If you've been fighting "acne" with every product on the shelf and nothing is working, the answer might not be a stronger acne treatment. It might be a completely different diagnosis.
The uniform bumps. The itching. The location on your chest, back, or forehead. The flares after sweating or taking antibiotics. The complete non-response to everything you've tried. These are the clues that your skin has been trying to tell you something — and now you know what to listen for.
The right antifungal treatment, combined with fungal-safe skincare and a few simple lifestyle adjustments, can clear pityrosporum folliculitis in a matter of weeks. After months or years of struggling, that kind of turnaround can feel life-changing. And it starts with asking one simple question: what if this isn't acne?
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Rubenstein RM, Malerich SA. (2014). Malassezia (Pityrosporum) folliculitis. Journal of Clinical and Aesthetic Dermatology.https://pubmed.ncbi.nlm.nih.gov/24688625/
- Saunte DM, et al. (2020). Malassezia-associated skin diseases. Journal of Investigative Dermatology.https://pubmed.ncbi.nlm.nih.gov/32087820/
- Prohic A, et al. (2016). Malassezia species in healthy skin and in dermatological conditions. International Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/26710919/
- Jacinto-Jamora S, et al. (1991). Pityrosporum folliculitis in the Philippines. International Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/1938052/
- Gupta AK, Batra R. (2004). Pityrosporum folliculitis. Skinmed.https://pubmed.ncbi.nlm.nih.gov/15476259/
- Bäck O, et al. (1985). Pityrosporum folliculitis: A common disease of the young and middle-aged. JAAD.https://pubmed.ncbi.nlm.nih.gov/3159701/
- Cohen PR. (2020). Pityrosporum folliculitis: A vignette. Skinmed.https://pubmed.ncbi.nlm.nih.gov/32738019/
- Saunte DM, Gaitanis G, Hay RJ. (2020). Malassezia-associated skin diseases, the use of diagnostics and treatment. Frontiers in Cellular and Infection Microbiology.https://pubmed.ncbi.nlm.nih.gov/32117804/
- American Academy of Dermatology. Acne look-alikes.https://www.aad.org/public/diseases/acne/really-acne/acne-look-alikes
- Zanelato TP, et al. (2015). Pityrosporum folliculitis: A retrospective study. Anais Brasileiros de Dermatologia.https://pubmed.ncbi.nlm.nih.gov/26375226/
Read This Next

Whiteheads (Closed Comedones): What They Are, Why They Form, and How to Get Rid of Them
Those small, flesh-colored bumps that won't pop? They're closed comedones — and they require a completely different approach than regular pimples. Here's what dermatologists recommend.
Read More →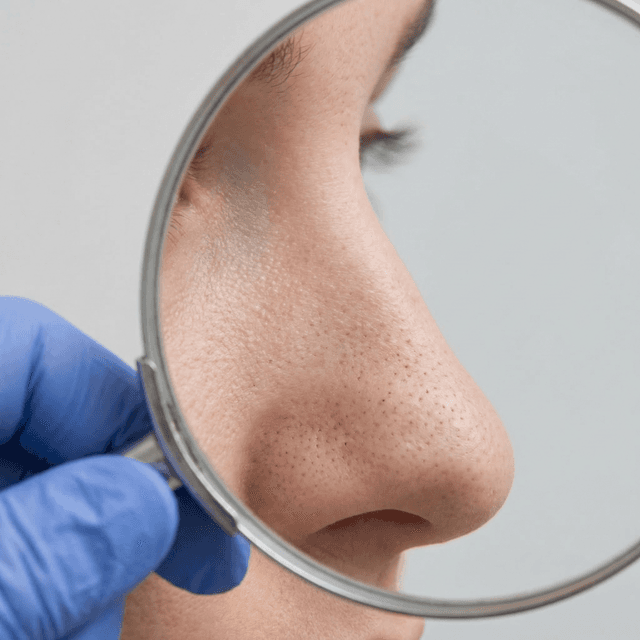
Blackheads (Open Comedones): Why They're Dark, How to Remove Them Safely, and What Actually Prevents Them
Blackheads aren't caused by dirt — they're oxidized oil plugs in open pores. Here's the science behind why they form and the dermatologist-approved ways to actually get rid of them.
Read More →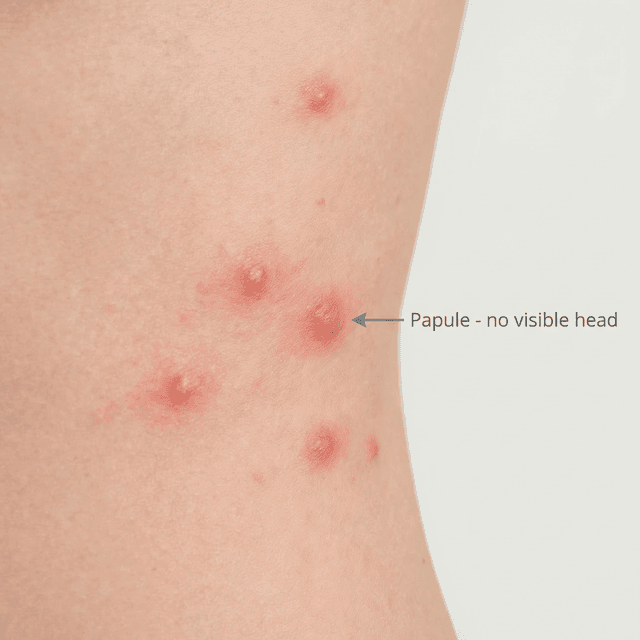
Papules: Understanding Small Red Acne Bumps and How to Treat Them
Those small, red, tender bumps without a visible head? They're papules — a sign your acne has become inflammatory. Here's what's happening beneath the surface and what to do about it.
Read More →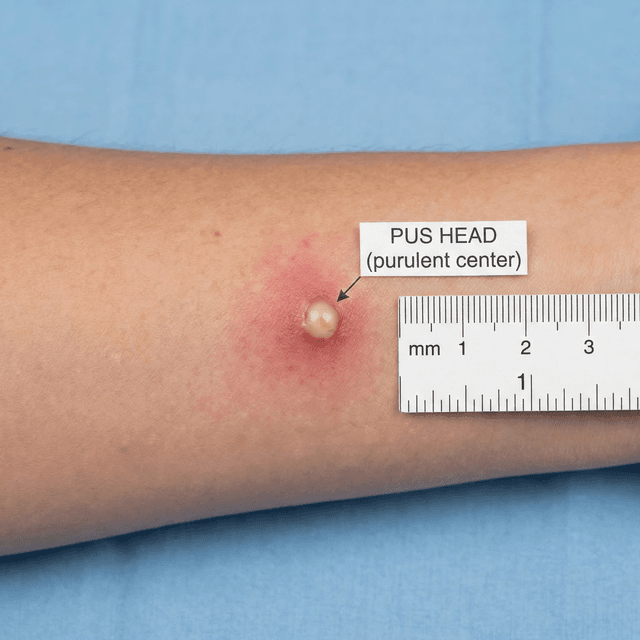
Pustules: The Classic Pimple — What's Inside, Should You Pop It, and How to Treat It
Pustules are what most people picture when they think 'pimple' — red bumps with a white or yellow center. Here's what's actually inside them, whether popping is ever okay, and what dermatologists recommend.
Read More →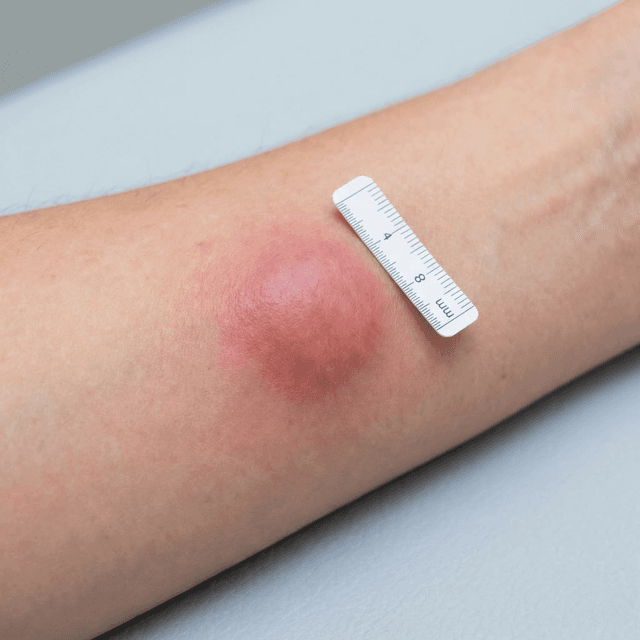
Nodular Acne: Understanding Deep, Painful Acne Bumps and Why They Need Professional Treatment
Hard, painful lumps deep under the skin that won't come to a head? That's nodular acne — a severe form that requires medical treatment. Here's what causes it and what actually works.
Read More →