Stress and Teen Acne: What Science Says About the Connection
Medically reviewed by Dr. Rachel Torres, MD, Pediatric Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated March 13, 2026
Key takeaways
- Stress doesn't just feel bad — it directly worsens acne through a well-documented hormonal cascade involving cortisol, CRH, and increased sebum production.
- The Stanford exam study confirmed it: students' acne severity significantly increased during high-stress exam periods compared to low-stress periods.
- Sleep deprivation is a major hidden driver — teens who sleep fewer than 7 hours show measurably higher cortisol levels and more inflammatory acne.
- Stress-related skin picking (excoriation) can cause scarring and infection, and may signal an anxiety disorder that deserves professional attention.
- Evidence-based stress management including regular exercise, consistent sleep, and even brief mindfulness practices have been shown to reduce both cortisol levels and acne severity.
You've got a big exam tomorrow. You barely slept last night. You looked in the mirror this morning and — right on cue — there's a fresh breakout on your chin.
If you've ever felt like your skin gets worse when life gets harder, you're not imagining it. Research consistently shows that psychological stress makes acne worse, and teenagers are uniquely vulnerable. Between school pressure, social dynamics, sleep deprivation, and the constant hum of social media, today's teens face a stress load that directly affects their skin.
Let's break down exactly what the science says — and, more importantly, what you can actually do about it.
How Stress Triggers Acne: The Science
To understand why stress causes breakouts, you need to understand a hormonal chain reaction that starts in your brain and ends in your pores.
Here's the pathway, step by step:
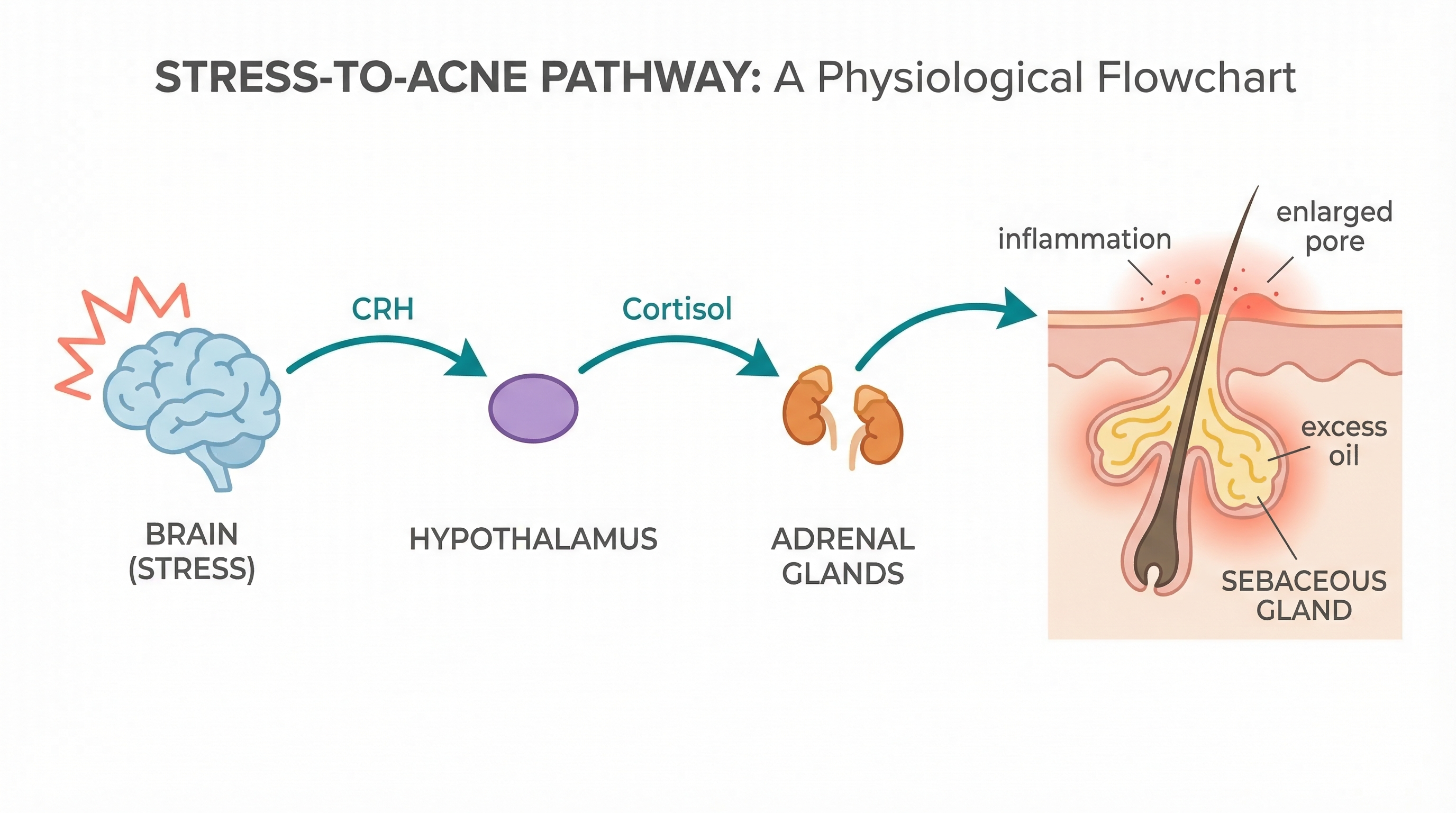
The Stress-Skin Axis
When you experience stress — whether it's a looming deadline, a fight with a friend, or scrolling through social media at 1 a.m. — your brain's hypothalamus sounds an alarm. It releases a hormone called corticotropin-releasing hormone (CRH), which kicks off your body's entire stress response.
Here's where it gets interesting for your skin: researchers have discovered that your sebaceous glands (the oil-producing glands in your skin) have their own CRH receptors. That means your skin cells can directly respond to stress hormones, independent of the rest of your body's stress response.
The cascade works like this:
- Stress activates the hypothalamus in the brain
- CRH is released, triggering the hypothalamic-pituitary-adrenal (HPA) axis
- Cortisol levels rise throughout the body
- CRH binds to receptors on sebaceous glands, stimulating them directly
- Sebum (oil) production increases, sometimes dramatically
- Inflammation ramps up as stress hormones activate pro-inflammatory pathways
- Excess sebum + inflammation = clogged, inflamed pores — in other words, acne
This is not folk wisdom or an old wives' tale. A landmark 2004 study published in Experimental Dermatology confirmed that sebocytes (the cells that make up your oil glands) are regulated by the neuroendocrine system and respond directly to stress hormones like CRH. The researchers described this as a "pathogenetic link between stress and acne."
It's Not Just Oil — It's Inflammation
Many people think stress acne is only about extra oil. But cortisol also suppresses your immune system's normal functioning while simultaneously increasing certain inflammatory responses in the skin. This creates the perfect storm:
- More sebum means more food for Cutibacterium acnes (the bacteria involved in inflammatory acne)
- More inflammation means existing pimples become redder, more swollen, and more painful
- Impaired skin barrier function makes your skin more reactive to irritants
- Slower wound healing means existing breakouts take longer to resolve
This is why stress acne often feels different — it tends to be more inflamed, deeper, and more painful than your everyday whiteheads.
The Stanford Exam Study
The most frequently cited research on stress and acne comes from Stanford University. In 2003, Dr. Annie Chiu and colleagues published a study in the Archives of Dermatology that tracked 22 university students through exam periods and compared their acne severity to non-exam (low-stress) periods.
The findings were clear:
- Acne severity increased significantly during exam periods compared to non-exam periods
- The correlation held true even after controlling for changes in sleep, diet, and skincare habits
- Students who reported higher perceived stress had correspondingly worse breakouts
- The relationship was strongest for inflammatory lesions (the red, painful kind) rather than non-inflammatory comedones (blackheads and whiteheads)
What made this study particularly compelling is that it measured perceived stress — not just the presence of exams. Students who felt more stressed showed more acne, even among students facing the same exams. This suggests that how you experience and manage stress matters as much as the stressor itself.
A 2007 study in Acta Dermato-Venereologica reinforced these findings, showing that increased sebum production in adolescents correlated with higher psychological stress levels. The link was consistent across different skin types and acne severities.
Types of Stress That Affect Teen Skin
Not all stress is created equal, and teens today face a uniquely complex web of stressors. Understanding what's driving your stress is the first step toward managing it — and your skin.
Academic Pressure
Exams, grades, college applications, AP classes, standardized testing — the academic pressure on today's teens is intense. This is often the most well-documented trigger for stress breakouts, partly because exam periods create a predictable, measurable stress timeline that researchers can study.
But it's not just exam week. The chronic, low-grade stress of staying on top of homework, maintaining a GPA, and meeting expectations creates a sustained cortisol elevation that keeps your oil glands in overdrive for weeks or months at a time.
Social Stress and Peer Dynamics
Friendships, romantic relationships, social hierarchies, bullying, and the constant performance of identity that adolescence requires — these are enormous stressors that adults often underestimate. Social rejection activates the same brain regions as physical pain, and for teens whose social world is their entire world, a falling-out with a friend can trigger a stress response as intense as any exam.
Social Media
This deserves its own category. Research increasingly links social media use to increased anxiety, poor self-esteem, and disrupted sleep — all of which independently worsen acne. The cruel irony is that many teens feel more stressed about their acne because of social media, where filtered skin is the norm and breakouts feel like a personal failure.
The comparison trap is real: you're seeing everyone else's best, most filtered moments while living your own unfiltered reality. That gap between expectation and reality is a potent source of chronic stress.
Family Stress
Parental conflict, divorce, financial strain, moving, or simply the friction that comes with growing up and wanting more independence — family stress is often invisible to outsiders but deeply felt by teens. Because it happens at home, where you're supposed to feel safe, family stress can be particularly corrosive.
Over-Scheduling
Sports, clubs, volunteering, part-time jobs, tutoring — many teens have schedules that would exhaust an adult. The resulting time pressure and lack of downtime keep cortisol levels elevated chronically, which is harder on your skin than a single stressful event.

The Stress-Acne Cycle
Here's where stress acne becomes particularly cruel: it feeds on itself.
- You're stressed → cortisol rises → oil production increases → you break out
- You notice the breakout → you feel self-conscious → stress increases further
- Increased stress → more cortisol → more oil → more breakouts
- Worsening skin → social anxiety → avoidance of activities → isolation → more stress
This cycle is well-documented in dermatology literature, and it's a major reason why stress-related acne can feel so much harder to manage than "normal" breakouts. You're not just fighting your skin — you're fighting a feedback loop.
A 2017 review in Acta Dermatovenerologica Croatica confirmed that the psychological impact of acne creates a self-reinforcing cycle: acne causes psychological distress, which worsens acne, which deepens distress. Breaking this cycle often requires addressing both the skin and the stress simultaneously.
If this sounds like you, know this: the cycle can be broken. It usually requires a two-pronged approach — treating the acne directly (with proven topical or oral treatments) while also addressing the stress. Neither alone is enough.
Sleep Deprivation and Breakouts
If stress is the fire, sleep deprivation is the gasoline.
The average teenager needs 8 to 10 hours of sleep per night, according to the American Academy of Sleep Medicine. Most teens get far less — surveys consistently show the average is closer to 6.5 to 7.5 hours on school nights.
Here's why that matters for your skin:
The Cortisol-Sleep Connection
A pivotal 1999 study in The Lancet by Spiegel, Leproult, and Van Cauter demonstrated that restricting sleep to 6 hours per night for just one week increased evening cortisol levels by a significant amount and slowed the rate at which cortisol cleared from the body. In other words, sleep-deprived people don't just make more stress hormones — those hormones hang around longer.
For teens, this is a double hit. You're already dealing with the hormonal upheaval of puberty, and then sleep deprivation layers additional cortisol on top of it.
Late-Night Screen Time
Most teens' sleep deprivation is driven, at least in part, by screens. Blue light from phones and laptops suppresses melatonin production, pushing your circadian rhythm later. But it's not just the light — it's the content. Social media, group chats, and the fear of missing out create psychological arousal that makes it harder to fall asleep, even after you put the phone down.
This creates its own vicious cycle: screen time → poor sleep → higher cortisol → worse acne → more stress about skin → more screen time to distract from the stress.
What Actually Helps
- Set a consistent bedtime — even on weekends, try to stay within an hour of your usual time
- Create a phone-free wind-down period of at least 30 minutes before bed
- Keep your bedroom cool and dark — your body temperature needs to drop to initiate sleep
- If you can't sleep, don't lie there stressing — get up, do something calm, and try again in 20 minutes
Stress Management Techniques That Help Your Skin
Not all stress management is created equal. Here are the approaches with the strongest evidence for reducing both stress and acne.
Exercise
Regular physical activity is one of the most potent cortisol regulators available to you — and it's free. Exercise reduces baseline cortisol levels, improves sleep quality, boosts mood through endorphin release, and increases blood flow to the skin.
You don't need to train like an athlete. Research shows that 30 minutes of moderate activity (a brisk walk, a bike ride, a casual swim) most days of the week is enough to meaningfully reduce stress hormone levels.
Important note: Sweat itself doesn't cause acne, but sitting in sweaty clothes or headbands can. Rinse your face (and body, if possible) soon after exercise. A gentle cleanser is all you need.
Mindfulness and Meditation
A 2015 meta-analysis in the Journal of Psychosomatic Research reviewed 29 studies on mindfulness-based stress reduction (MBSR) in healthy individuals and found consistent reductions in stress, anxiety, and cortisol levels.
You don't need to meditate for an hour or attend a retreat. Evidence suggests that even 5 to 10 minutes of guided breathing or mindfulness per day produces measurable stress reduction. Apps like Headspace, Calm, and Insight Timer offer teen-friendly guided sessions.
Here's a simple technique you can try right now:
- Breathe in for 4 counts through your nose
- Hold for 4 counts
- Breathe out for 6 counts through your mouth
- Repeat 5 times
This activates your parasympathetic nervous system — the "rest and digest" branch that directly counteracts the cortisol-producing stress response.
Journaling
Writing about stressful experiences has been shown to reduce cortisol levels and improve immune function. For teens, journaling can be as simple as spending 5 minutes before bed writing down three things that went well and one thing that stressed them out. The act of externalizing stress — getting it out of your head and onto paper — interrupts the rumination cycle that keeps cortisol elevated.

Skin Picking, Anxiety, and Acne
We need to talk about this, because it's far more common than most people realize.
Skin picking — known clinically as excoriation disorder or dermatillomania — is a body-focused repetitive behavior in which a person compulsively picks, squeezes, or scratches at their skin. It's closely linked to anxiety and often intensifies during stressful periods.
For teens with acne, the pattern usually looks like this:
- You notice a pimple or bump
- You feel an intense urge to squeeze, pop, or "fix" it
- You spend minutes (or even hours) in front of the mirror, picking
- Afterward, you feel temporary relief, followed by guilt, shame, and skin that looks worse
- The damaged skin becomes inflamed, scarred, or infected
- You feel more stressed about how your skin looks, which triggers more picking
When Picking Becomes a Problem
Occasional pimple-popping is common. But if you find yourself:
- Picking at your skin for extended periods, sometimes without even realizing it
- Unable to stop even when you know you're making it worse
- Avoiding social situations because of damage from picking
- Feeling significant distress or shame around the behavior
...it may be worth talking to a therapist who specializes in body-focused repetitive behaviors. Cognitive behavioral therapy (CBT), specifically a technique called habit reversal training, has strong evidence for treating skin picking. This is not about willpower — it's about rewiring a neurological pattern.
Tip for parents: If you notice your teen spending long periods in the bathroom, or if their acne seems disproportionately scarred relative to its severity, skin picking may be a factor. Approach the conversation with compassion, not criticism. "I've noticed you seem frustrated with your skin — can I help?" is much more effective than "Stop picking at your face."

When Stress Acne Might Signal Something Deeper
Sometimes persistent stress breakouts are telling you something important — not just about your skin, but about your mental health.
If your teen is experiencing:
- Persistent anxiety that doesn't go away, even when the stressor is removed
- Depressed mood, withdrawal from friends or activities, loss of interest in things they used to enjoy
- Panic attacks or physical symptoms of anxiety (racing heart, difficulty breathing, nausea)
- Disordered eating as a way to cope with stress or control their appearance
- Self-harm, including skin picking that feels compulsive or self-punishing
...the acne is not the primary concern. These are signs of a mental health condition that deserves professional support. A good dermatologist will recognize when skin symptoms are connected to psychological distress and may refer to a therapist or counselor.
The American Academy of Dermatology acknowledges the significant psychological burden of acne and recommends that dermatologists screen for depression and anxiety in patients with moderate to severe acne, particularly adolescents.
There is absolutely no shame in seeking help. Stress acne that resists all topical treatment is sometimes your body's way of telling you that the problem is deeper than your pores.

Daily Stress-Reduction Habits for Teens
Grand gestures are less effective than small, daily habits. Here are practical, sustainable stress-reduction strategies that are realistic for a teenager's life.
Morning
- Wake up 15 minutes earlier than you need to. Rushing produces cortisol before the day even starts.
- Eat breakfast. Blood sugar crashes worsen stress responses and trigger more cortisol. Even something small — yogurt, a banana, toast — helps stabilize your system.
- Do a 2-minute body scan. Before you reach for your phone, close your eyes and notice how your body feels. Tight shoulders? Clenched jaw? Just noticing is the first step to releasing.
During School
- Take 3 deep breaths before a test. Box breathing (in for 4, hold for 4, out for 4, hold for 4) activates the parasympathetic nervous system within seconds.
- Step outside between classes if possible. Even 60 seconds of natural light and fresh air lowers cortisol.
- Talk to someone. Social connection is one of the strongest stress buffers we have. One genuine conversation is worth more than an hour of scrolling.
After School
- Move your body for at least 20 to 30 minutes. It doesn't have to be intense — a walk with a friend or some stretching counts.
- Set a homework boundary. Work for 45 minutes, then take a 10-minute break. Your brain (and your cortisol levels) need recovery time.
- Limit social media to 30 minutes if possible. Use screen time tools to make this automatic rather than relying on willpower.
Evening
- Put your phone in another room at least 30 minutes before bed. This single change improves sleep quality more than almost anything else.
- Do something you enjoy that isn't a screen — read, draw, play an instrument, talk to someone in your family.
- Go to bed at the same time every night, including weekends. Consistency is more important than total hours.
A Note on "Productivity Culture"
Many teens have internalized the idea that rest is laziness. It is not. Rest is when your body repairs itself — including your skin. Collagen synthesis, immune regulation, and hormone balancing all happen during rest and sleep. Giving yourself permission to do nothing for a few minutes each day is not indulgent; it's biological maintenance.
Treating Stress Acne Directly
While managing stress is essential, you should also treat the acne itself. Stress acne responds to the same evidence-based treatments as other forms of acne:
- Benzoyl peroxide (2.5-5%) to kill acne-causing bacteria
- Adapalene (Differin) to unclog pores and reduce inflammation
- Niacinamide to help regulate oil production and calm redness
- Non-comedogenic moisturizer to support barrier function (stressed skin often has a compromised barrier)
Avoid the temptation to over-treat or add too many products at once. Irritated, over-stripped skin produces more oil and becomes more reactive — which is the opposite of what you need when your skin is already stress-sensitized.
If over-the-counter treatments aren't helping after 8 to 12 weeks of consistent use, see a dermatologist. Prescription options like topical retinoids, combination therapies, or in some cases oral medications can be highly effective, especially when combined with stress management.
Bottom Line
The connection between stress and acne is not in your head — it's in your hormones. The pathway from psychological stress to CRH release to sebum production to clogged, inflamed pores is well-established science.
But here's the empowering part: the same pathway works in reverse. When you reduce stress, cortisol drops, oil production normalizes, inflammation decreases, and your skin begins to heal.
You cannot eliminate stress from your life — and you shouldn't try to. Some stress is normal, even healthy. But you can change your relationship with stress. Consistent sleep, regular exercise, limited screen time, and the willingness to ask for help when you need it are not just "self-care buzzwords." They are evidence-based interventions that measurably improve both your mental health and your skin.
If your acne gets worse during exams, flares up after a bad week, or seems to follow your emotional state like a barometer — now you know why. And now you know what to do about it.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Chiu A, Chon SY, Kimball AB. The response of skin disease to stress: changes in the severity of acne vulgaris as affected by examination stress. Arch Dermatol. 2003;139(7):897-900https://pubmed.ncbi.nlm.nih.gov/12873885/
- Zouboulis CC, Böhm M. Neuroendocrine regulation of sebocytes — a pathogenetic link between stress and acne. Exp Dermatol. 2004;13(Suppl 4):31-35https://pubmed.ncbi.nlm.nih.gov/15507110/
- Ganceviciene R, et al. Skin anti-aging strategies. Dermatoendocrinol. 2012;4(3):308-319https://pubmed.ncbi.nlm.nih.gov/23467476/
- Yosipovitch G, et al. Study of psychological stress, sebum production and acne vulgaris in adolescents. Acta Derm Venereol. 2007;87(2):135-139https://pubmed.ncbi.nlm.nih.gov/17340019/
- Jović A, et al. The impact of pyschological stress on acne. Acta Dermatovenerol Croat. 2017;25(2):1133-141https://pubmed.ncbi.nlm.nih.gov/28871928/
- American Academy of Dermatology. Acne: Who Gets and Causes. 2024https://www.aad.org/public/diseases/acne/causes/acne-causes
- Leung DYM, Bieber T. Atopic dermatitis and stress. Lancet. 2003;361(9352):151-160https://pubmed.ncbi.nlm.nih.gov/12531593/
- Suh DH, et al. A multicenter epidemiological study of acne vulgaris in Korea. Int J Dermatol. 2011;50(6):673-681https://pubmed.ncbi.nlm.nih.gov/21595661/
- Albuquerque RG, et al. Could adult female acne be associated with modern life? Arch Dermatol Res. 2014;306(8):683-688https://pubmed.ncbi.nlm.nih.gov/24849308/
- Lim HW, et al. The burden of skin disease in the United States. J Am Acad Dermatol. 2017;76(5):958-972https://pubmed.ncbi.nlm.nih.gov/28259441/
- Spiegel K, Leproult R, Van Cauter E. Impact of sleep debt on metabolic and endocrine function. Lancet. 1999;354(9188):1435-1439https://pubmed.ncbi.nlm.nih.gov/10543671/
- Khoury B, et al. Mindfulness-based stress reduction for healthy individuals: A meta-analysis. J Psychosom Res. 2015;78(6):519-528https://pubmed.ncbi.nlm.nih.gov/25818837/
Read This Next

How to Get Rid of Chest Acne: What Works and What Doesn't
Read More →
How to Fade Acne Marks and Dark Spots: Realistic Timelines
Read More →
How to Get Rid of Forehead Acne: Causes and Fixes

Skincare Routine for Teens with Oily Skin: Morning and Night
