When to Take Your Teenager to a Dermatologist for Acne: A Parent's Decision Guide
Medically reviewed by Dr. Sarah Mitchell, MD, Board-Certified Dermatologist
Written by Teen Acne Solutions Editorial Team — Updated March 15, 2026
Key takeaways
- The average parent waits 18 months before seeking dermatological help for their teen — by then, scarring may have already started
- Any acne that's affecting your teen's mood, social life, or self-esteem is 'bad enough' for a dermatologist
- Moderate-to-severe acne rarely resolves with drugstore products alone — professional treatment saves time, money, and skin
- A good first appointment lasts 15-30 minutes and results in a clear, written treatment plan
- Many insurance plans cover dermatology visits for acne — it may be more affordable than you think
You've watched your teenager cycle through face washes, spot treatments, and half a dozen products recommended by friends or TikTok. Some mornings their skin looks a little better. Other mornings they won't make eye contact in the kitchen. You've told yourself it's normal — nearly every teenager gets acne, after all — but a quiet question keeps surfacing: should I take my teen to a dermatologist for acne, or am I overreacting?
You're not overreacting. And the fact that you're asking means you should probably keep reading.
Research suggests that the average parent waits roughly 18 months after acne first appears before seeking professional help. By that point, inflammatory acne may have already begun leaving permanent scars — scars that are far more difficult and expensive to treat than the acne itself. The American Academy of Dermatology recommends seeing a dermatologist when acne doesn't respond to over-the-counter treatments within 8 to 12 weeks, yet most families don't walk through a dermatologist's door until well past that window.
This guide is for parents who are on the fence. We'll walk through the specific signs that it's time, explain exactly what happens at a first dermatology appointment (no surprises), cover insurance and cost realities, and help you prepare your teen so the visit feels empowering rather than embarrassing.

Signs It's Time to Go
Not all acne requires a dermatologist. Mild breakouts — a few whiteheads or blackheads that come and go — often respond well to gentle cleansing and a benzoyl peroxide or salicylic acid product from the drugstore. But there's a clear line where over-the-counter efforts stop being enough, and recognizing that line is what separates months of frustration from a real solution.
Here are the signals that your teen's acne has crossed into territory that warrants professional evaluation.
Acne Has Persisted for More Than Three Months Despite OTC Treatment
If your teenager has been consistently using an appropriate over-the-counter acne product — not just washing their face, but actually applying a medicated treatment — for three months with no meaningful improvement, the acne is unlikely to resolve on its own. The key word is "consistently." If they've been using products correctly and the breakouts haven't budged, that's a clear signal.
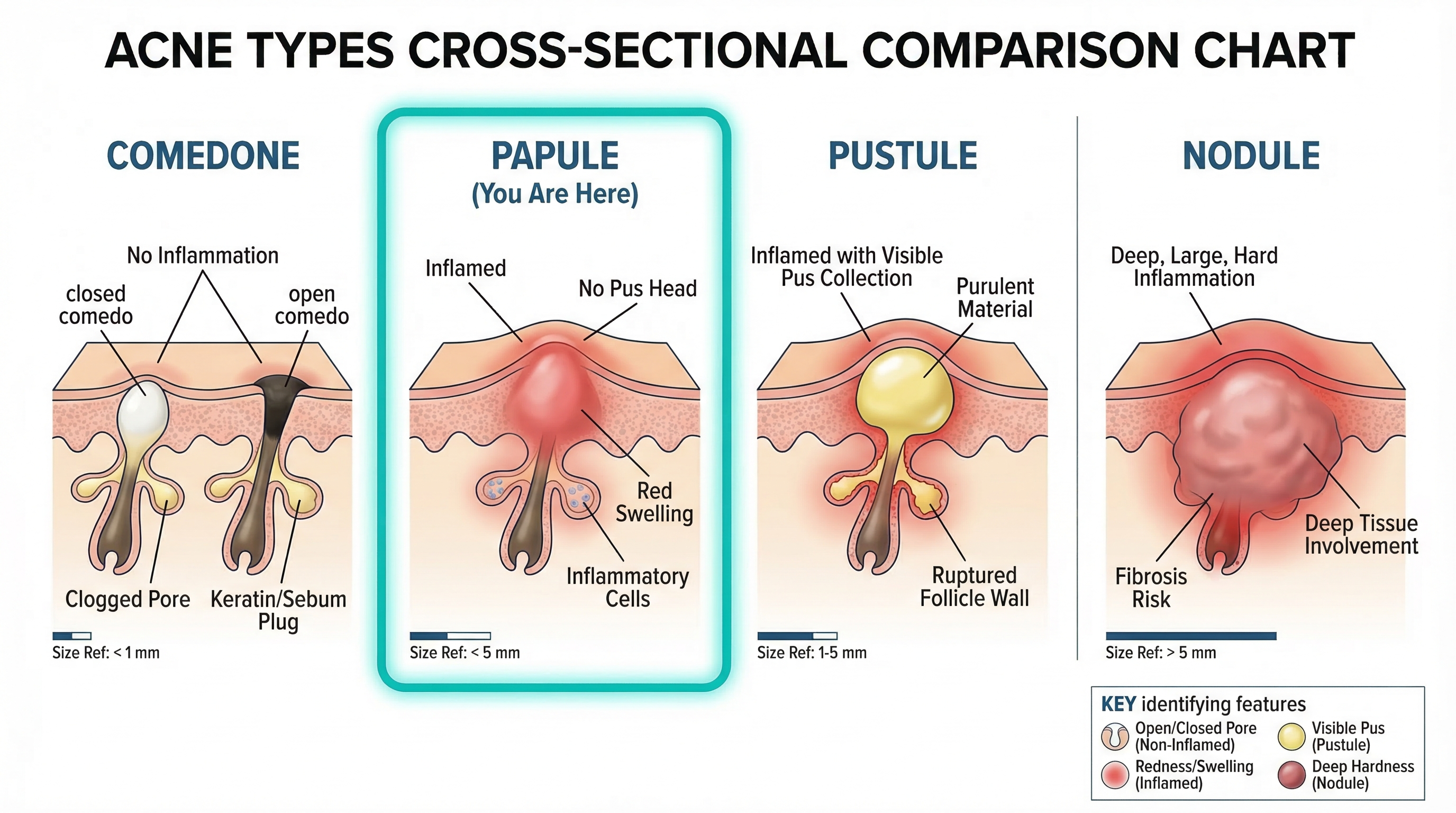
Painful, Deep, or Cystic Lesions
Surface-level pimples are one thing. Deep, painful bumps that sit under the skin — often called nodules or cysts — are another category entirely. These lesions form deep within the pore, involve significant inflammation, and carry a much higher risk of scarring. Drugstore products simply cannot penetrate deeply enough to treat them effectively. If your teen has even a few of these, a dermatologist visit is warranted.
Scarring Has Already Started
Run your fingertips gently across your teen's cheeks, jawline, or forehead. If you feel textural changes — small pits, raised bumps, or uneven terrain — scarring has begun. This is one of the most important reasons not to wait. Active acne can be treated and resolved. Scars are permanent alterations to the skin's structure. Every month of delay potentially means more scarring that your teen will carry into adulthood.
Emotional and Social Impact
This one doesn't come with a clinical measurement, but it may be the most important sign of all. Research published in the Journal of Investigative Dermatology found strong associations between adolescent acne and mental health problems, including anxiety, depression, and even suicidal ideation. You don't need a severity scale to justify a dermatologist visit. If acne is affecting your teen's mood, willingness to socialize, school participation, or self-esteem, it is severe enough to warrant professional treatment. Full stop.
Watch for: avoiding mirrors, refusing to be photographed, skipping social events, wearing hats or hair over the face to hide skin, increased irritability around the topic, or withdrawing from activities they used to enjoy.
Family History of Severe Acne
Acne has a strong genetic component. If you, your partner, or other close family members dealt with significant acne — especially the kind that left scars — your teen is at higher risk for a similar trajectory. Early intervention in these cases can prevent the same outcome.
Acne in Unusual Patterns or Locations
Acne concentrated along the jawline, hairline, or in a band across the forehead can sometimes indicate hormonal imbalances or external triggers (like a sports helmet or hair product) that a dermatologist can identify and address. Acne that appears suddenly, progresses rapidly, or shows up in unusual distributions deserves a trained eye.
Red Flags Checklist
Print this out or save it to your phone. If your teen meets two or more of these criteria, schedule a dermatology appointment this week:
- Acne has been present for 3+ months with no improvement from OTC products
- Deep, painful lumps under the skin (nodular or cystic acne)
- Any sign of scarring — pitting, discoloration that doesn't fade, textural changes
- Your teen is avoiding social situations, photos, or activities because of their skin
- You notice mood changes — increased anxiety, sadness, or irritability tied to breakouts
- Strong family history of severe or scarring acne
- Acne is spreading to new areas (back, chest, shoulders) or worsening despite treatment
- Your teen is picking or squeezing lesions frequently, causing further damage
- OTC products are causing significant dryness, irritation, or allergic reactions
- Your teen is under 10 or over 18 and experiencing a new onset of significant acne (may indicate hormonal issues)
If even one of the bolded items above applies — emotional impact or scarring — that alone is reason enough.
Why Parents Wait Too Long
If you've been putting off this appointment, you're in good company. Understanding why parents delay can help you push past the hesitation.
"It's Just a Phase"
Yes, acne is common during puberty. Around 85% of teenagers experience some form of acne. But "common" doesn't mean "harmless" or "self-limiting." Moderate-to-severe acne left untreated during adolescence can persist well into the twenties and leave lasting physical and emotional marks. The "they'll grow out of it" approach is a gamble — and the stakes are your teen's skin and self-confidence.
Cost Concerns
Many parents assume a dermatologist visit will be expensive, and without insurance, it can be. But here's what most parents don't calculate: the cumulative cost of OTC trial-and-error. Between cleansers, spot treatments, serums, and "acne systems" — many of which cost $20 to $50 each and get abandoned after a few weeks — families routinely spend $200 to $500 or more on drugstore products that don't work before finally seeing a professional. A single dermatology visit with a targeted prescription often costs less than a year of guessing. We'll break down costs in more detail below.
Not Wanting to "Medicalize" Normal Puberty
This is a thoughtful concern, and it comes from a good place. You don't want your teen to feel like something is wrong with them. But framing a dermatologist visit as "getting expert help for a really common skin issue" is very different from framing it as "fixing a problem." Teens see specialists for braces, sports injuries, and vision correction without stigma. Acne treatment is no different.
"I Had Acne and I Turned Out Fine"
Maybe you did. But memory is generous, and skin science has advanced significantly. The treatments available today — including topical retinoids, combination therapies, and carefully monitored oral medications — are safer, more effective, and faster-acting than what was available a generation ago. Your teen doesn't need to suffer through it the way you might have.
What to Expect at the First Visit
The unknown is a big part of what keeps families from booking. Here's exactly what a first teenage acne dermatologist visit looks like, step by step.
Before You Walk In
Most dermatology offices will ask you to fill out intake forms covering your teen's medical history, current medications, family skin history, and a description of their acne concerns. Some offices send these digitally before the appointment. Fill them out thoroughly — this information helps the dermatologist before they even enter the room.
The Examination
The dermatologist will examine your teen's skin, typically on the face, and often the chest, back, and shoulders as well. They'll look at the types of acne lesions present (comedones, papules, pustules, nodules, or cysts), their distribution, and any existing scarring. This part usually takes just a few minutes.
Many dermatologists use a standardized grading system to classify acne severity — mild, moderate, or severe — which helps guide treatment decisions and track progress over time. Some offices take clinical photographs at the first visit. This isn't to embarrass your teen; it's to create a baseline so improvement can be measured objectively at follow-up appointments.
The Conversation
A good dermatologist will spend time talking — not just to you, but to your teen. They'll ask about current skincare routines, products being used, how long the acne has been present, and how it's affecting daily life. This is the diagnostic conversation, and it matters as much as the physical exam.
Expect the appointment to last 15 to 30 minutes total. Some parents are surprised by how efficient it is. A skilled dermatologist can assess acne severity and formulate a treatment plan relatively quickly because they do this every single day.
The Treatment Plan
Before you leave, you should receive a clear treatment plan. This might include prescription medications (topical, oral, or both), specific product recommendations, lifestyle guidance, and a follow-up timeline. A good practice will provide written instructions — either printed or sent via a patient portal — so you're not relying on memory.
Questions to Ask the Dermatologist
Come prepared. Having a list of questions signals to the dermatologist that you're engaged and ensures you leave with the information you need. Here are the most important questions for a first teen acne visit:
- How would you classify my teen's acne severity? (Mild, moderate, or severe — this sets expectations.)
- What's causing this specific type of acne? (Hormonal? Bacterial? Product-related? Understanding the "why" helps everything else make sense.)
- What treatment do you recommend, and why this approach over alternatives?
- What side effects should we watch for? (Every medication has them. Know what's normal and what warrants a call.)
- How long before we should expect to see improvement? (Most acne treatments take 6 to 12 weeks to show meaningful results. Knowing this prevents premature discouragement.)
- Could acne get worse before it gets better on this treatment? (With retinoids, this is common and temporary. Being warned prevents panic.)
- Are there any foods, products, or habits that could be making this worse?
- When should we come back for a follow-up? (Typically 6 to 8 weeks for the first check-in.)
- What should we do if the treatment isn't working or side effects are too much? (Know the communication plan — portal message, phone call, urgent visit.)
- Is there anything we should avoid while on this treatment? (Sun exposure, certain supplements, other topical products.)
Write these down or save them on your phone. In the moment, it's easy to forget.
Understanding the Treatment Plan
Dermatologists have a well-established toolkit for teenage acne, and understanding the options helps you support your teen's treatment adherence.
Topical Treatments
These are the foundation of most acne treatment plans. Common prescriptions include:
- Topical retinoids (tretinoin, adapalene, tazarotene): These vitamin A derivatives increase skin cell turnover, prevent clogged pores, and reduce inflammation. They're considered the gold standard for acne treatment and are often the first line of defense. They can cause initial dryness and a temporary "purge" period.
- Topical antibiotics (clindamycin, erythromycin): Usually prescribed in combination with benzoyl peroxide to kill acne-causing bacteria while preventing antibiotic resistance.
- Combination products: Many prescriptions combine a retinoid with an antibiotic or benzoyl peroxide in a single application, simplifying the routine — which is critical for teenager compliance.
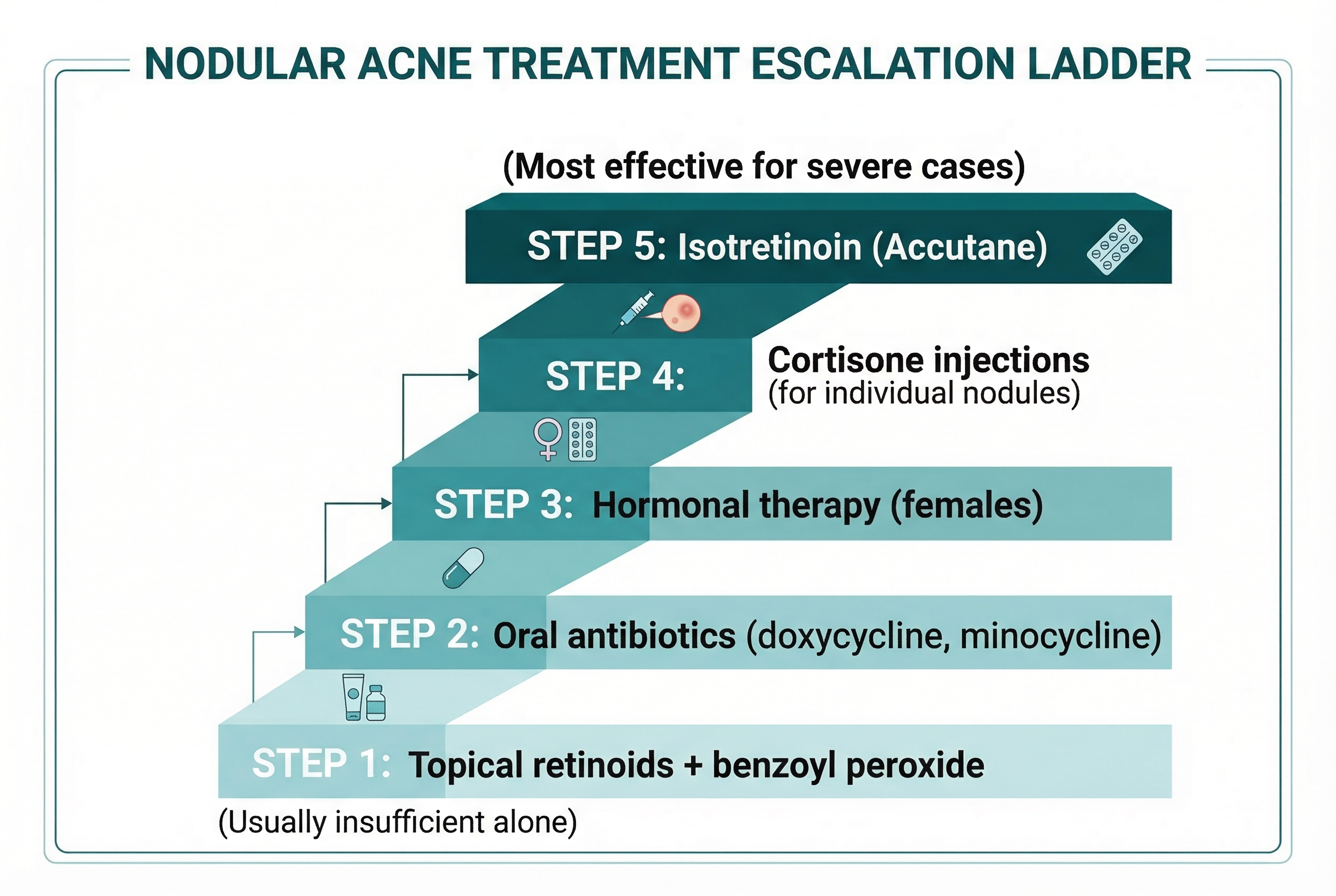
Oral Medications
For moderate-to-severe acne, oral medications may be added:
- Oral antibiotics (doxycycline, minocycline): Typically prescribed for a limited course (3 to 6 months) to reduce inflammation and bacteria. They're not a long-term solution but help bring severe acne under control while topicals take effect.
- Hormonal therapies (oral contraceptives, spironolactone): For female teens with hormonally driven acne, these can be highly effective. The dermatologist will discuss candidacy, benefits, and risks thoroughly.
- Isotretinoin (formerly brand-named Accutane): Reserved for severe, scarring, or treatment-resistant acne. It's the most powerful acne medication available and can produce long-term remission. It requires careful monitoring, including monthly blood tests and, for female patients, pregnancy prevention measures. Many parents feel anxious about isotretinoin, but when appropriately prescribed and monitored, it has an excellent safety profile and can be genuinely life-changing.
Timeline Expectations
This is critical: most acne treatments take 8 to 12 weeks to show significant improvement. Some treatments, particularly retinoids, may temporarily worsen acne in the first 2 to 4 weeks (the "purging" phase). Setting this expectation upfront prevents your teen from abandoning treatment too early — which is the single most common reason acne treatment "fails."
Plan for a follow-up appointment 6 to 8 weeks after starting treatment. The dermatologist will assess progress and adjust the plan if needed.
Insurance and Costs
Let's address the financial elephant in the room directly.
What Insurance Typically Covers
Most health insurance plans — including employer-sponsored plans, ACA marketplace plans, and Medicaid — cover dermatology visits for acne because acne is classified as a medical condition, not a cosmetic concern. Your copay for a specialist visit typically ranges from $30 to $75, depending on your plan.
Prescription medications are usually covered to some degree, though coverage varies. Generic topical retinoids and antibiotics are widely covered and affordable. Brand-name combination products may require prior authorization or have higher copays.
Without Insurance
An initial dermatology consultation without insurance typically costs $150 to $300, depending on your location. Follow-up visits are usually less. It's not nothing — but compare that to what you've already spent on products that didn't work.
Making Prescriptions Affordable
- Ask for generics. Most acne medications have affordable generic versions. A tube of generic tretinoin cream costs $20 to $40 with a coupon, compared to over $500 for some brand-name versions.
- Use discount programs. GoodRx, RxSaver, and manufacturer coupons can dramatically reduce out-of-pocket costs for prescriptions. Always check before filling.
- Ask about samples. Dermatologists often have samples of newer medications. These can help your teen try a product before you commit to a full prescription cost.
The Real Cost Comparison
Consider this: a family that spends 18 months trying OTC products at an average of $30 per product, switching every 4 to 6 weeks, will spend roughly $300 to $500 — with no improvement and possible scarring. A dermatologist visit ($40 copay) plus a generic prescription ($15 to $40/month) that actually works costs less over the same period and delivers results. The math almost always favors going to the dermatologist sooner.
Finding the Right Dermatologist
Not all dermatologists are equally experienced with teenage skin, and the right fit matters for your teen's comfort and compliance.
Pediatric Dermatologist vs. General Dermatologist
Pediatric dermatologists specialize in skin conditions in children and adolescents. They're excellent for teens, but they're relatively rare — there are fewer than 400 board-certified pediatric dermatologists in the U.S. A general dermatologist who regularly treats adolescent acne is perfectly appropriate and far more accessible.
What to Look For
- Board certification by the American Board of Dermatology. This is non-negotiable.
- Experience with teen patients. Look at the practice's website or call and ask: do they see a lot of teenagers?
- Communication style. A dermatologist who talks directly to your teen, explains things clearly, and doesn't rush the appointment is worth their weight in gold.
- Accessible follow-up. Does the practice have a patient portal? Can you message with questions between appointments? Good follow-up communication is critical for treatment success.
Telehealth Options
Dermatology is one of the specialties that has adapted well to telehealth. Many dermatologists now offer virtual initial consultations or follow-up appointments. For teens who are anxious about an in-person visit, a telehealth appointment can be a lower-pressure first step. The dermatologist can evaluate acne severity through video and photos, prescribe treatment, and schedule an in-person follow-up if needed.
Telehealth can also solve the access problem. If you live in a rural area or the nearest dermatologist has a months-long waitlist, a virtual visit can get treatment started much sooner.

Preparing Your Teen
How you approach the appointment with your teenager matters enormously. Done well, this visit can be empowering. Done poorly, it can feel like one more thing that's "wrong" with them.
Frame It as Help, Not Fixing
Language matters. Instead of "We need to do something about your skin," try "I've noticed your skin's been bothering you, and I'd like to get you some expert help — if you're open to it." The first framing makes the teen a problem to be solved. The second makes them a person being supported.
Give Them Ownership
Whenever possible, let your teen be part of the decision. Ask if they'd like to see a dermatologist. Share what you've read. Let them look up the dermatologist's website. The more agency they have in the process, the more likely they are to engage with treatment.
Let Them Speak at the Appointment
This is one of the most important things you can do: resist the urge to answer every question the dermatologist asks. Let your teen describe their skin concerns, their current routine, and how acne makes them feel. You're there as backup and support, not as spokesperson. A skilled dermatologist will direct questions to your teen, and your job is to allow that dynamic to unfold.
That said, you should absolutely speak up about things your teen might not mention: family history, insurance questions, practical concerns about the treatment plan, or anything you've observed about mood changes.
Normalize the Experience
If your teen seems embarrassed about the appointment, gentle normalization goes a long way. "Tons of people your age see dermatologists — it's like going to the eye doctor for your skin." If you've seen a dermatologist yourself, share that. If their friends have clear skin, it's worth noting that many of them may have gotten professional help, too — they just don't broadcast it.
Discuss Privacy
Older teens, especially, may want some privacy during the appointment. Let them know ahead of time that if they want a moment to talk to the dermatologist alone, that's completely fine. Some teens will share things with a doctor that they won't say in front of a parent — concerns about body image, mental health, or specific questions about treatment side effects. Giving them that space is a gift.
The Bottom Line: Earlier Is Almost Always Better
If you've read this far, you're the kind of parent who takes their teen's wellbeing seriously. Here's the honest truth: very few parents regret taking their teen to a dermatologist too early. Many regret waiting too long.
The American Academy of Dermatology's guidelines are clear: acne that doesn't respond to OTC treatment within two to three months, any acne causing emotional distress, and any acne showing signs of scarring should be evaluated by a dermatologist. These aren't arbitrary thresholds — they're evidence-based recommendations designed to prevent exactly the kind of unnecessary suffering and permanent damage that delayed treatment causes.
Your teen's acne may ultimately be straightforward to treat. A topical retinoid and some guidance might be all they need. Or it may require a more involved approach. Either way, a dermatologist can provide a clear answer and a clear plan in a single 30-minute appointment — something no amount of internet research or drugstore shopping can replicate.
You don't need to wait until acne is "bad enough." If it's bothering your teen, it's bad enough. If it's bothering you, it's worth investigating. Trust your instincts on this one. The dermatologist's office is a judgment-free zone, and no one has ever been turned away for caring too much about their kid's skin.
Make the appointment. Your future teen will thank you.
This article was medically reviewed by Dr. Sarah Mitchell, MD, a board-certified dermatologist with over 15 years of experience treating adolescent acne. It is intended for informational purposes only and should not substitute for professional medical advice. Always consult a qualified healthcare provider for diagnosis and treatment recommendations specific to your teen's skin.
How we reviewed this article:
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
- Zaenglein AL, et al. (2016). Guidelines of care for the management of acne vulgaris. JAAD.https://pubmed.ncbi.nlm.nih.gov/26897386/
- Halvorsen JA, et al. (2011). Suicidal ideation, mental health problems in adolescents with acne. JID.https://pubmed.ncbi.nlm.nih.gov/20944653/
- Tan JK, Bhate K. (2015). Epidemiology of acne. British Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/26031612/
- Kraft J, Freiman A. (2011). Management of acne. CMAJ.https://pubmed.ncbi.nlm.nih.gov/21398228/
- Strauss JS, et al. (2007). Guidelines of care for acne vulgaris management. JAAD.https://pubmed.ncbi.nlm.nih.gov/17276540/
- Gollnick H, et al. (2003). Management of acne. JAAD.https://pubmed.ncbi.nlm.nih.gov/12734496/
- Layton AM, et al. (1993). Acne vulgaris treatment review. Journal of Clinical Pharmacy and Therapeutics.https://pubmed.ncbi.nlm.nih.gov/8126048/
- American Academy of Dermatology. When to see a dermatologist.https://www.aad.org/public/diseases/acne/derm-treat/when-to-see
- Mallon E, et al. (1999). Quality of life in acne. British Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/10354575/
- Bhate K, Williams HC. (2013). Epidemiology of acne vulgaris. British Journal of Dermatology.https://pubmed.ncbi.nlm.nih.gov/23210645/
Read This Next

How to Help Your Teenager with Acne: A Complete Guide for Parents
Watching your teen struggle with acne is harder than most people realize. Here's a dermatologist-reviewed guide for parents who want to help — without overstepping, minimizing, or making things worse.
Read More →
How to Talk to Your Teenager About Acne Without Making It Worse
Bringing up acne with your teen is a minefield. Say the wrong thing and they shut down. Say nothing and they suffer alone. Here's how to start the conversation the right way.
Read More →
A Parent's Guide to Buying Acne Products for Your Teenager: What Actually Works
The skincare aisle is overwhelming and your teen is begging for help. Here's a no-nonsense guide to which ingredients actually work, what's a waste of money, and how to build a simple routine without breaking the bank.
Read More →
Is My Teenager's Acne Normal? When to Worry and When to Wait
Every parent wonders: is this normal teenage acne, or is something wrong? Here's how to tell the difference between typical puberty breakouts and acne that needs medical attention.
Read More →